| Author | Affiliations |
| Zachary D. Levy, MD | Hofstra North Shore-LIJ School of Medicine, Department of Emergency Medicine, Hempstead, New York |
| Richard E. Temes, MD | Hofstra North Shore-LIJ School of Medicine, Department of Neurology, Hempstead, New York |
| Amir R. Dehdashti, MD | Hofstra North Shore-LIJ School of Medicine, Department of Neurosurgery, Hempstead, New York |
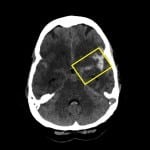
A 54-year-old woman presented to the emergency department with sudden onset severe headache, nausea and vomiting upon waking that morning. On examination, she was alert and oriented, with a mild right facial droop and a right upper extremity pronator drift. A non-contrast computed tomography (CT) of the head revealed diffuse subarachnoid blood, with a prominent triangular focus projecting into the left Sylvian fissure (Figure).
Figure. Left MCA arrow sign.
MCA, middle cerebral artery
Diagnosis
Patients with aneurysmal subarachnoid hemorrhage often present with acute headache and evidence of blood in the basilar cisterns on non-contrast CT.1 When aneurysms of the middle cerebral artery rupture, blood may pool in the area around the insular cortex and ipsilateral Sylvian cistern. The resulting hemorrhage takes on the appearance of an arrow pointing towards the side of the lesion, also known as the middle cerebral artery (MCA) arrow sign.2 Following non-contrast CT, the patient underwent cerebral angiography, which did indeed demonstrate an aneurysm at the distal M1 segment at the origin of the left anterior temporal branch. The patient subsequently underwent craniotomy and successful clipping of her aneurysm. She had normal post-operative neurologic function.
Footnotes
Supervising Section Editor: Sean O. Henderson, MD
Full text available through open access at http://escholarship.org/uc/uciem_westjem
Address for Correspondence: Zachary Levy, MD. 300 Community Drive, Manhasset, NY 11030. Email: zlevy@nshs.edu.
Submission history: Submitted September 13, 2014; Accepted September 23, 2014
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
- Van gijn J, Rinkel GJ. Subarachnoid haemorrhage: diagnosis, causes and management. Brain. 2001;124(Pt 2):249-78.
- Maramattom BV, Wijdicks EF. Arrow sign in MCA trifurcation aneurysm. Neurology. 2004;63(7):1323. [PubMed]