| Author | Affiliation |
|---|---|
| John Graneto, DO, MEd | Midwestern University, Department of Emergency Medicine, Downers Grove, Illinois |
| Tessa Damm, DO | Midwestern University, Department of Emergency Medicine, Downers Grove, Illinois |
Introduction
Methods
Results
Discussion
Limitations
Conclusion
Abstract
Introduction:
Noise in the emergency department (ED) may be perceived to be high by both patients and nurses alike. This increased noise level is hypothesized to be responsible for communication interference and subsequent disruption of complex procedures and decision-making. The objective of this study is to quantify ambient noise level in an ED while obtaining coincident subjective surveys from nurses in the assessment of actual versus perceived noise.
Methods:
Data collected from surveys of ED nurses on each of 3 different dates revealed that sound levels within the selected ED were consistently at or below 70 decibels (dB) of sound as measured by a sound level meter. This level of sound is of the same decibel of normal conversation at a 3–5 foot distance. Nurses surveyed overwhelmingly rated noise as “low” or “not loud” irrespective of a variance (though predominantly within a 10 dB range) in actual sound decibel measurements.
Results:
Years of experience of work within emergency departments proved the most consistent predictor of nurses’ opinions on the frequency with which noise levels within the ED were louder than they should be, with more experienced nurses all ranking noise levels as “frequently” or “always” louder than they should be.
Conclusion:
Individual variance existed in how nurses felt that noise level affected work function. ED nurses’ perception of noise is perceived to be low and generally not interfering with their cognitive function.
INTRODUCTION
Ambient noise in the work environment may be perceived as a nuisance which could negatively impact the well-being and productivity of those who are exposed to it.1 Noise in the emergency department (ED) may be perceived to be high by both patients and nurses alike.2 This increased noise level is hypothesized to be responsible for communication interference and subsequent disruption of complex procedures and decision-making.2 The objective of this study is to quantify ambient noise level in an ED while obtaining coincident subjective surveys from nurses in the assessment of actual versus perceived noise.
METHODS
A single hospital ED was selected for use in data collection. It is a busy urban teaching hospital with an annual patient volume approaching 50,000. The hospital’s institutional review board approved the study.
A multi-range sound level meter was calibrated and set to parameters consistent with Occupational Safety and Health Administration regulatory testing, both range/frequency rating (high) as well as response time (slow), on each of 3 separate dates on which data was collected. The sound level meter was then positioned adjacent to ED nurses on the counter top while they completed a survey regarding the current noise. The nurses verbally consented to participate in the survey. They were blinded to the purpose of the study and its attempts to correlate actual versus perceived noise levels. The surveys contained questions relating noise level to the medical work environment suitable for completing cognitive tasks as well as for a healing environment for patients.
Upon completion of the survey, the data collector recorded the corresponding sound level as displayed on the sound level meter during completion of the survey. Data was collected on 3 separate dates during April 2007 during shift change, between day shift and afternoon shift, and subsequently evaluated. A total of 55 surveys were completed for evaluation. Nurses were allowed to complete a survey only once per shift, though a few nurses completed an additional survey done on a different day.
RESULTS
Fifty-five ED nurses (RNs) were enrolled and completed surveys. All surveys were completed at a time when the sound level meter registered a sound level at or below 70 decibels (dB), a level consistent with normal conversation at a 3–5 feet distance.
In evaluating actual versus perceived noise, the registered sound level from the sound decibel reading device was compared to how staff subjectively rated the concomitant ambient noise level on a scale of low, not loud, moderate, loud, and very loud (Figure 1).
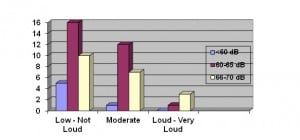
Actual sound level and number of response (y-axis) compared with subjective nurses reporting of noise level (x-axis).
The majority of staff surveyed ranked the ambient noise level at the time of the survey as “low” or “not loud”, regardless of the corresponding sound level as measured in dB by the sound level meter. All surveys were completed at times when the sound level meter registered sound levels at or below 70 dB. All but 6 of 55 total completed surveys were completed at a time when the sound level meter registered a reading between 60–70 dB. The 6 out-of-range readings were all less than 60 dB. The results of the subjective survey may reflect the fact that the human ear necessitates a decibel change of approximately 5 dB to notice a change in volume and 10 dB to judge a sound as twice as loud.5
All surveys and sound measurements were obtained in non-patient-care areas of the ED. The possibility that noise levels at the patient bedside, particularly during resuscitation situations when clinical decision-making is critical and patient demand for a healing environment high, may be different than those measured in non-patient-care areas.
Significantly, years of experience working within an ED appeared to be the most consistent predictor of how staff answered the question of whether noise levels within the ED were greater than they should be. Those nurses with greater than 10 years of experience working in emergency departments all answered that question as “frequently” or “always”, while none of the nurses with less than 1 year of experience answered the question as “always”.
Responses to staff answering the question, “Do you believe the noise in the Emergency Department is louder than it should be?” was compared with years of experience working in emergency medicine. In this case the nurses with the lower number of years working in the ED perceived the noise levels to be frequently higher than they should be.
Nurses’ responses were collected regarding the effect of ambient noise on work environment and perceived cognitive functioning during medication calculation, charting and phone report. These responses grouped together as a possible effect on cognitive function. The cognitive function results showed that 32% of nurses felt their cognitive function was never affected by noise, 21% answered “rarely” and 33% said “sometimes”. “frequently” and “always” only accounted for 14%.
The nurses were finally asked if they felt the noise levels affected the patients’ healing environment; 39% of responses were “never” or “rarely”, an additional 37% said “sometimes” and 24% responding “frequently” or “always”.
DISCUSSION
The impact of noise on clinical decision-making has previously been studied in operating rooms. A study by Murthy and Malhotra in India concluded that operating room noise reduced mental efficiency and short-term memory in anesthesia residents.3
The presumption that emergency departments are noisy has not previously been well described objectively in medical literature. However, a study by Park et al4 of radiology residents, ambient noise in the ED setting and its effect on the accuracy of diagnosing rib fractures was measured. In this study, it was concluded that physicians accustomed to reading x-rays in quiet environments performed better under quiet conditions than noisy conditions; whereas the accuracy of physicians accustomed to a noisy environment was unaffected by the presence of ambient noise.4
Sound level decibel loudness for environmental noise is well established for a variety of ranges.5 Included are those ranges specific to the sound level meter used in this study. Normal conversation at 3 feet is considered 60–70dB, while city traffic as experienced inside a car is 85dB and in a subway 95dB.
There was inconsistency with nurses reporting of noise level interfering with their work function. The only group of respondents that did not classify work interruption as “frequent” or “always” were those whose coincident sound levels (per the sound level meter) were less than 60 dB. A 2002 evaluation of noise within a post-anesthesia care unit suggests that excess noise, of which conversation is the most common cause, can cause adverse physiological and psychological effects on patients as well as increase mistakes amongst medical professionals.6
No consistent patterns existed in the data collected regarding nurses’ opinions on how current sound levels affected patients’ healing environment.
LIMITATIONS
Data collection occurred only in non-patient-care areas of the ED, e.g. at the nurses’ station and not in patient rooms. The use of the term “noise” in the survey may have been ambiguous as some nurses interpret noise to be routine ambient ED staff conversation as well as medical device alarms or even family members and telephone calls. “Noise” may be alternatively interpreted as any sound that results in interruption in cognitive function or transmission of messaging as opposed to just sounds.
CONCLUSION
This study intended to evaluate and quantify sound levels within a selected ED. These objective measurements were then correlated with nurses’ opinions regarding noise levels. Data collected on each of three different dates revealed that sound levels within the selected ED were consistently at or below 70 dB of sound as measured by a sound level meter. This level of sound is of the same decibel of normal conversation at a 3–5 foot distance. Nurses surveyed overwhelmingly rated noise as “low” or “not loud” irrespective of a variance (though predominantly within a 10 dB range) in actual sound decibel measurements. Years of experience of work within emergency departments proved the most consistent predictor of nurses’ opinions on the frequency with which noise levels within the ED were louder than they should be, with more experienced nurses all ranking noise levels as “frequently” or “always” louder than they should be. Individual variance existed in how nurses felt that noise level affected work function. Further studies could include physicians as part of the survey group and comparing their perceptions with nursing staff. Patients’ perceptions of noise levels could also be compared against ED noise and inpatient noise. Further studies are necessary to determine if a correlation exists between perceived sound level and actual work function as far as whether noise results in distractions significant enough for errors to occur.

Questionnaire.
Footnotes
Address for Correspondence: John Graneto, DO, MEd, Chicago College of Osteopathic Medicine, Midwestern University, Suite 302 Science Hall, 555 31st Street, Downers Grove, IL 60515. Email: jgraneto@midwestern.edu.
Submission history: Revision received October 22, 2012; Submitted February 21, 2013; Accepted May 28, 2013
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1 Hodge B, Thompson JF Noise pollution in the operating theatre. The Lancet. 1990; 335:891-894
2 Vincent C, Wears R Communication in the emergency department: separating the signal from the noise. The Medical Journal of Australia. 2002; 176:409-410
3 Murthy VSSN, Malhotra SK, Bala I Detrimental effects of noise in anaesthetists. Canadian Journal of Anesthesia. 1995; 42:608-611
4 Park SH, Song HH, Han JH Effect of noise on the detection of rib fractures by residents. Investigative Radiology. 1994; 29:54-58
5 Chasin M Decibel (Loudness) Comparison; Centre for Human Performance & Health, Ontario, Canada. . ;
6 Allaouchiche Noise in the postanaesthesia care unit. British Journal of Anaesthesia. 2002; 88:369-373


