| Author | Affiliation |
|---|---|
| Wesley H. Self, MD, MPH | Vanderbilt University School of Medicine, Department of Emergency Medicine, Nashville, Tennessee |
| Steven J. White, MD | Vanderbilt University School of Medicine, Department of Emergency Medicine, Nashville, Tennessee |
| Candace D. McNaughton, MD, MPH | Vanderbilt University School of Medicine, Department of Emergency Medicine, Nashville, Tennessee |
| Alan B. Storrow, MD | Vanderbilt University School of Medicine, Department of Emergency Medicine, Nashville, Tennessee |
| Corey M. Slovis, MD | Vanderbilt University School of Medicine, Department of Emergency Medicine, Nashville, Tennessee |
| Sean P. Collins, MD, MSC | Vanderbilt University School of Medicine, Department of Emergency Medicine, Nashville, Tennessee |
Introduction
Methods
Results
Discussion
Limitations
Conclusion
Abstract
Introduction:
The purpose of this study was to test if intravenous (IV) fluids warmed to body temperature are associated with greater patient comfort than room temperature IV fluids in adult emergency department (ED) patients.
Methods:
This was a pilot double-blind, crossover, randomized controlled trial. Enrolled subjects sequentially received boluses of body temperature (36°C) and room temperature (22 °C) IV fluid, with the order of boluses randomized. Each subject’s level of discomfort was assessed prior to and after each bolus, using a 10 cm visual analog scale (Discomfort VAS), with higher scores indicating greater discomfort. We calculated the change in Discomfort VAS score associated with body temperature IV fluid (ΔVASbody) and room temperature IV fluid (ΔVASroom) by subtracting the score reported before the bolus from the score reported after that bolus. We compared changes in Discomfort VAS score with body temperature and room temperature IV fluid using the Wilcoxon matched-pairs signed-rank test.
Results:
Twenty-seven subjects were included. Treatment with body temperature IV fluid was associated with a significant decrease in discomfort (median ΔVASbody: −0.7 cm; interquartile range (IQR): −4.5 cm to +0.4 cm) compared to room temperature IV fluid (median ΔVASroom: +1.2 cm; interquartile range: −0.1 cm to + 3.6 cm) (P = 0.001).
Conclusion:
In this small trial of adult ED patients, infusing IV fluids warmed to body temperature was associated with improved comfort compared to standard, room temperature IV fluids.
INTRODUCTION
Nearly one-quarter of emergency department (ED) patients in the United States are treated with intravenous (IV) fluids.1 These fluids are typically stored at room temperature and infused into patients without prior warming. During infusion of room temperature IV fluids, some patients experience shivering, chills and discomfort.2,3 Small studies of patients undergoing surgery suggest that warming IV fluids to body temperature prior to infusion may reduce shivering and improve patient comfort in the perioperative period.2–7 However, the effect of warming IV fluids on patient comfort in the ED has not been evaluated. In this pilot study of adult ED patients, we compared the level of discomfort associated with infusion of IV fluids warmed to body temperature with those infused at room temperature.
METHODS
We conducted a double-blind, crossover, randomized controlled trial to test the impact of warming IV fluids to body temperature on patient comfort. Prior to the clinical study, we validated our method for warming IV fluid in a pre-trial validation study.
Pre-Trial Validation Study
IV fluids were warmed using the Safe & Warm IV Fluid Warmer Device (Safe & Warm, Seattle, Washington). Prior to enrolling patients, we tested the temperature of fluids infused with this device with an infusion set-up identical to that used in the clinical study. A 500 mL bag of normal saline was inserted into the insulated warming jacket of the device and connected to 295 cm of IV tubing and an infusion pump. An electronic thermometer was inserted into the distal end of the IV tubing, the location where an IV catheter would be connected to infuse fluid into a patient. A neoprene insulating sleeve enclosed all the IV tubing, preventing bedside personnel from feeling the temperature of fluid in the tubing. The insulated warming jacket within the device contained two sodium acetate heat packs. When the device was turned “on,” the heat packs were activated and warmed the fluid. In simulated infusions, we pumped 500 mL bags of normal saline at 1000 mL/hour with the device turned on and off. With the device on, the temperature of fluid at the distal end of the tubing was 36°C (body temperature) throughout the simulated infusion. When the device was off, the temperature of fluid was 22°C (room temperature).
Clinical Study
This crossover, randomized controlled trial was approved by the local Institutional Review Board and conducted in a university-affiliated ED with approximately 61,000 visits annually. Inclusion criteria included: 1) acute illness preventing adequate oral hydration as judged by the treating physician; and 2) age 18–45 years. Exclusion criteria included: 1) critical illness requiring rapid IV fluid resuscitation; 2) severe (distracting) pain; 3) heart or kidney failure; and 4) cognitive impairment or language barrier preventing communication in English with investigators. All subjects sequentially received two 500 mL IV boluses of normal saline over 30 minutes, one warmed to body temperature (36°C) and one at room temperature (22 °C) (Figure 1). A dose of 500 mL of normal saline infused at 1000 mL/hour was chosen because this was the most common fluid bolus used clinically in our ED. The order of boluses was randomized in a simple 1:1 scheme with a random number generator. Randomization procedures and administration of the 2 fluid boluses were completed by a dedicated study nurse, the only person unblinded to fluid temperatures. Both body temperature and room temperature fluids were administered through the Safe & Warm IV Fluid Warmer Device as described in the Pre-Trial Validation Study. The device was turned on for infusion of body temperature fluid and off for room temperature fluid. Subjects reported their general level of bodily discomfort prior to and after each bolus, using a 10 cm visual analogue scale (Discomfort VAS), with 0 cm signifying no discomfort and 10 cm signifying the worst discomfort imaginable. The Discomfort VAS was modeled after the visual analog scale used for pain assessment.8,9 After finishing both boluses, subjects were also asked which treatment they preferred overall (bolus #1 or bolus #2).
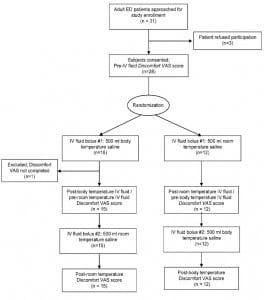
Flow diagram of subject participation.
Statistical Analysis
For each subject, we calculated the change in Discomfort VAS score associated with body temperature IV fluid (ΔVASbody) by subtracting the score reported before the body temperature bolus from the score reported after that bolus. Hence, a negative ΔVASbody indicated a decrease in discomfort associated with body temperature fluid treatment. Similarly, we calculated the change in Discomfort VAS score associated with the room temperature fluid (ΔVASroom) by subtracting the score reported before the room temperature bolus from the score reported after that bolus. The primary analysis involved comparing changes in Discomfort VAS associated with body temperature (ΔVASbody) and room temperature (ΔVASroom) fluid. We planned to perform this comparison with a paired t-test if the data were normally distributed or a Wilcoxon matched-pairs signed-rank test if the data were not normally distributed. We performed sample-size calculations using a paired t-test, type I error probability of 0.05, 80% power, and a standard deviation of 2 cm for the difference between ΔVASbody and ΔVASroom. At least 21 subjects were needed to detect a 1.3 cm difference in ΔVASbody and ΔVASroom. We based the goal of detectable difference of 1.3 cm on previous work showing that a 1.3 cm change on a visual analog scale for pain was clinically significant.8,9
We also calculated the proportion of subjects who stated a preference for body temperature over room temperature IV fluids and used the one-sample z-test to compare this to the null (proportion of 0.5). We completed statistical analyses using Stata 11.1 (Stata Corp, College Station, Texas). Two-tailed P-values < 0.05 were considered statistically significant.
RESULTS
Thirty-one patients were approached for enrollment; 28 patients consented, and 27 completed the protocol (Figure 1). Distributions for ΔVASbody and ΔVASroom did not approximate normal distribution, and analyses were completed with nonparametric statistics. Treatment with body temperature IV fluid was associated with a significant decrease in discomfort (median ΔVASbody: −0.7 cm; interquartile range (IQR): −4.5 cm to +0.4 cm) compared to room temperature IV fluid (median ΔVASroom: +1.2 cm; IQR: −0.1 cm to + 3.6 cm) (P = 0.001) (Figure 2). After receiving both boluses, 20/27 (74%; 95% confidence interval: 57% to 91%) subjects reported a preference for body temperature over room temperature fluid (P = 0.012).
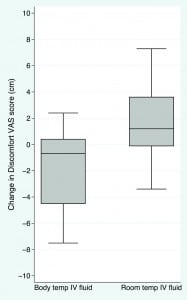
DISCUSSION
This pilot study suggests that warming IV fluids to body temperature before infusion is associated with improved comfort for ED patients compared to room temperature fluids. IV fluid treatment is often initiated in the ED to increase intravascular volume in dehydrated patients. In addition to achieving physiologic endpoints, such as normalization of vital signs, an important secondary goal of IV fluid treatment is to improve patient comfort. As the practice of emergency medicine has evolved, the specialty has increasingly recognized the importance of patient-centered care and promoting patient satisfaction and comfort.10 When assessing the effectiveness of medical interventions, considering patient-centered outcomes in addition to physiologic endpoints is essential for meaningful evaluation.11,12 Warming IV fluids prior to infusion may be a simple technique to improve the effectiveness of a commonly used ED treatment from the patient perspective. Given the promising results of this study, future research is indicated to study warmed IV fluids in the ED.
The median change on the Discomfort VAS associated with body temperature fluid was −0.7 cm, compared to +1.2 cm for room temperature fluid; therefore, body temperature fluid was associated with a median change of 1.9 cm toward less discomfort compared to room temperature fluid. The Discomfort VAS was modeled after the pain visual analog scale, which has been well-validated and is commonly used in the ED.8,9 A change of 1.3 cm on the pain visual analog scale is considered clinically significant. 8,9 Therefore, the magnitude of difference between VAS scores with body temperature and room temperature fluids suggests that the statistical difference we found in Discomfort VAS scores may correlate with an important clinical difference. Further suggesting the difference is clinically important is our finding that 74% of subjects reported an overall preference for body temperature fluids.
LIMITATIONS
Several limitations to our study should be highlighted. This was a small study conducted to help plan a larger trial by testing the methods of warming IV fluids and preliminarily evaluating the potential impact of warming fluids on patient comfort. While our results showed a statistically significant reduction in patient discomfort with warmed IV fluids, further research is needed evaluating larger samples sizes and other outcomes, including cost-effectiveness and ease of implementation. In this study, warmed IV fluids were administered to one patient at a time by a dedicated study nurse. Therefore, while we believe use of the device is simple and potentially feasible in the ED, we were unable to evaluate usability of the device by end-users in this study.
CONCLUSION
Warming IV fluids to body temperature prior to infusion was associated with improved comfort for adult ED patients compared to standard, room temperature IV fluids in this pilot study. Future research is warranted to further investigate the effect of warmed IV fluids on patient-centered outcomes and the feasibility of warming IV fluids in the ED setting.
Footnotes
FUNDING
The Safe & Warm IV Fluid Warmer Device used in this trial was provided by Safe & Warm, Inc. Safe & Warm, Inc. had no role in the conduct of the study, interpretation of the data, or preparation of this manuscript.
Address for Correspondence: Wesley H. Self, MD, MPH, Department of Emergency Medicine, Vanderbilt University, 1313 21st Ave; 703 Oxford House, Nashville, TN 37232-4700. Email: wesley.self@vanderbilt.edu.
Submission history: Revision received August 17, 2012; Submitted November 27, 2012; Accepted January 28, 2013
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. Safe & Warm, Inc. proided the warmers, but did not fund this research study.
REFERENCES
1 Nawar EW, Niska RW, Xu J National hospital ambulatory medical care survey: 2005 emergency department summary. Adv Data. 2007; :1-32
2 Workhoven MN Intravenous fluid temperature, shivering, and the parturient. Anesth Analg. 1986; 65:496-498
3 Woolnough M, Allam J, Hemingway C Intra-operative fluid warming in elective caesarean section: a blinded randomised controlled trial. Int J Obstet Anesth. 2009; 18:346-351
4 Hasankhani H, Mohammadi E, Moazzami F The effects of intravenous fluids temperature on perioperative hemodynamic situation, post-operative shivering, and recovery in orthopaedic surgery. Can Oper Room Nurs J. 2007; 25:20-24
5 Smith CE, Gerdes E, Sweda S Warming intravenous fluids reduces perioperative hypothermia in women undergoing ambulatory gynecological surgery. Anesth Analg. 1998; 87:37-41
6 Camus Y, Cohen DS, Lienhart A The effects of warming intravenous fluids on intraoperative hypothermia and postoperative shivering during prolonged abdominal surgery. Acta Anaesthesiol Scand. 1996; 40:779-782
7 Goyal P, Kundra S, Sharma S Efficacy of intravenous fluid warming for maintenance of core temperature during lower segment cesarean section under spinal anesthesia. J Obstet Anaesth and Crit Care. 2011; 1:73-77
8 Todd KH, Funk KG, Funk JP Clinical significance of reported changes in pain severity. Ann Emerg Med. 1996; 27:485-489
9 Gallagher EJ, Liebman M, Bijur P Prospective validation of clinically important changes in pain severity measured on a visual analog scale. Ann Emerg Med. 2001; 38:633-638
10 Govindarajan P, Larkin GL, Phodes KV Patient-centered integrated networks of emergency care: Consensus-based recommendations and future research priorities. Acad Emerg Med. 2010; 17:1322-1329
11 Stewart M, Brown JB, Weston WW . Patient-Centered Medicine: Transforming the Clinical Method. 2003;
12 Stewart M, Brown JB, Donner A The impact of patient-centered care on outcomes. J Fam Pract. 2000; 49:796-804


