| Author | Affiliation |
|---|---|
| Robin R. Hemphill, MD, MPH | Emory School of Medicine Chapin Hall Center for Children at the University of Chicago |
| Benjamin S. Heavrin, MD, MBA | Vanderbilt University |
| Joy Lesnick, PhD | Chapin Hall Center for Children at the University of Chicago |
| Sally A. Santen, MD, PhD | Emory School of Medicine Chapin Hall Center for Children at the University of Chicago |
ABSTRACT
Introduction:
Academic emergency physicians (EPs) often feel that the demands of clinical productivity, income generation, and patient satisfaction conflict with educational objectives. The objective of this study was to explore whether the quality of faculty bedside teaching of residents correlated with high clinical productivity, measured by relative value units (RVUs). We also explored the strategies of high-performing faculty for optimal RVU generation and teaching performance.
Methods:
We performed a mixed method study using quantitative and qualitative methods to analyze the relationship between RVUs, patient satisfaction, and teaching performance. We examined the relationship between teaching performance ratings, patient satisfaction, and RVUs per hour using correlations. Following this initial analysis, we conducted semi-structured interviews with the eight faculty members who have the highest clinical (RVU) and educational productivity ratings to learn more about their strategies for success. Our Institutional Review Board approved this study.
Results:
We correlated resident evaluations of faculty with RVUs billed per hour. We conducted semi-structured interviews of faculty who led in both RVU productivity and resident evaluations. From these interviews, several themes emerged. When asked about how they excel in billing, most said that they pay attention to dictating a thorough chart on every patient and try to “stay busy” throughout their entire shift. When asked how they excel at resident education, most leading faculty said that they try to find a “teaching moment” and find small “clinical pearls” to pass along. Nevertheless, all eight leading faculty members believe that as the emphasis on billing productivity increases, resident and student education will suffer.
Conclusion:
Contrary to the opinion of some physicians, faculty can excel at both clinical productivity and resident education. This study found that highly efficient clinical productivity correlated with excellent resident teaching. This high level of performance did not appear to be at the expense of other important measures such as patient satisfaction or student teaching.
INTRODUCTION
Emergency physicians (EPs) working in an academic medical setting may feel that the demands of seeing patients, documenting charts, and maintaining patient satisfaction conflict with the additional duty of teaching. As emergency department (ED) crowding increases there are additional pressures to maintain or increase revenue from clinical practice. As a result, faculty may feel that financial priorities are competing with their ability to adequately teach students and residents. In a survey given to Core Clerkship Directors of United States Medical Schools faculty expressed concern about balancing documentation requirements with the educational mission.1 This survey noted a concern about potential declines in the quality of patient care due to the increased focus on documentation. The major medical societies representing EPs have called for additional research on the impact that crowding may have on the educational mission.3 Given this belief among EPs, it is surprising to find that recent research does not suggest a sacrifice in resident education due to productivity concerns.3–5
Several research questions guided this exploratory study. For example, we sought to understand the relationship between high clinical productivity and the effects on teaching performance and patient satisfaction. In addition, we sought to better understand how physicians who are rated highly as teachers could also have high relative value units (RVUs).
METHODS
We performed a mixed method study using interview and retrospective data to explore the relationship between RVUs, patient satisfaction, and teaching performance. We collected the ratings of performance and productivity of 31 EPs from July 2006 to June 2007 at a large teaching hospital. We included all full-time EP faculty members who worked primarily in the adult ED. Since RVU generation is lower for our pediatric ED, the eight faculty members who work primarily in pediatrics were not included.
The variables we studied included measurements of RVUs billed per hour, patient satisfaction, student and resident evaluation of faculty. We estimated clinical productivity by the average faculty RVUs calculated based on the year. We based patient satisfaction scores on phone calls made by Professional Research Consultants (PRC) to patients seen in the ED. PRC placed a call an average of 1,035 times a month and reached 233 eligible adult ED patient participants. Two hundred of those patients answered survey questions. The department reported the percentage of patient evaluations where the care by the attending physician was rated as “excellent.” This score comprised the composite metric.
Emergency medicine (EM) is a mandatory fourth year rotation for all 104 medical students at our institution. Students rated faculty after their one-month rotation based on a five-point scale. Evaluations assessed content and availability of clinical teaching from “awesome, met expectations I didn’t even know I had” to “poor, didn’t meet any of my expectations.” All students completed evaluations, which were returned to faculty monthly. We averaged the student ratings to create an average for the year.
Residents evaluated faculty in February. The majority of residents completed faculty evaluations (87%). Their assessment was based on the question, “For the faculty member above, please rate him/her in terms of bedside teaching.” The student and resident teaching performances were estimated by the average scores of their respective evaluations.
We used Pearson’s Correlation to examine the relationship between performance ratings and productivity scores, using average RVUs per hour as the dependent variable. This portion of the study was determined to be Institutional Review Board (IRB) exempt.
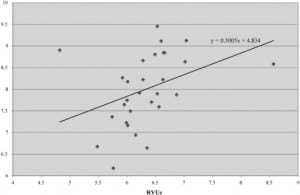
To learn more about how successful faculty members balance the dual responsibilities of teaching and patient care/revenue generation, we identified eight core faculty members with high average RVUs and high performance ratings. We graphed RVUs vs. resident teaching and selected faculty with high scores in both categories for semi-structured interviews. We recorded, transcribed and analyzed the interviews. We coded the interviews according to categories and recurring themes using the constant comparative method of analysis and grouping of data chunks.6 This portion of the study received IRB approval. A study member (BH) conducted interviews and was unaware of the specific performance metrics achieved by the faculty. The remainder of the study team was blinded to which faculty members were interviewed.
RESULTS
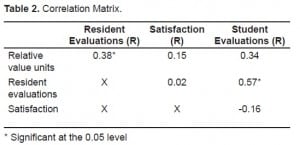
The distribution of the five variables appears in Table 1. Higher teaching performance ratings from residents were correlated with higher average RVUs per hour (Table 2, Figure 1). While resident bedside teaching correlated with student clinical teaching, student clinical teaching did not reach statistical significance with RVU performance. There was no correlation between RVUs and patient satisfaction.

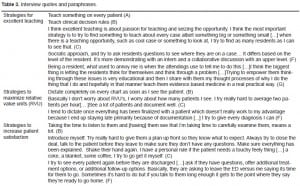
Among the semi-structured interviews of faculty who led in RVU productivity and resident evaluations, several themes emerged (Table 3). When asked how they excel in billing, most said that they do a thorough dictated chart on every patient and try to “stay busy” throughout their shift. When asked how they excel at resident education, most leading faculty said that they try to find a “teaching moment” on each patient, regardless of how big or small that may be. Many find small “clinical pearls” to teach. Nevertheless, all eight leading faculty members believe that as the emphasis on billing productivity increases, resident and student education will suffer.

DISCUSSION
Contrary to the belief of some physicians that increasing clinical productivity will decrease their ability to teach, we found that faculty with high RVU generation also had high resident bedside teaching scores. However, high clinical productivity did not correlate with excellence in student teaching scores or patient satisfaction. At the same time, there was no evidence that these performance dimensions suffered in the high performers.
A similar finding was noted in a general internal medicine clinic. Supervising resident physicians increased productivity by three fold as measured by RVUs, compared to independent delivery of patient care.4 That study also found that having residents in the clinic did not affect clinical productivity. Recent studies in EM have found little relationship between clinical productivity and student teaching evaluations.4 However, this study also noted a subset of the most highly productive faculty also rated highly as teachers by students.4 Kelly et al5 considered how workload effected physician’s teaching scores and attempted to control for individual teaching ability as well as resident grading tendencies. The study found that the abilities of the individual attending physician correlated to the overall teaching score, but that ED volumes and perceptions of workload had no significant effect on the overall teaching evaluation. Skilled instructors received better teaching scores regardless of how busy they were. However, this study did not use objective RVU metrics of clinical productivity. Instead, investigators chose self-reported measurements of productivity.
Our study extends the findings of prior studies. We note that physicians who were highly productive were perceived to be good bedside teachers. In addition, we found a correlation between resident and student teaching, suggesting that faculty who are strong resident bedside teachers also excel at teaching students. However, student interactions with attending physicians are limited compared to residents who get to know attending physicians over the duration of their residency. Patient satisfaction did not appear to suffer in the hands of the physicians who are generating the most RVUs, although the number of surveys completed by patients for each physician was small.
We conducted semi-structured interviews with the most productive faculty to better understand their approach to clinical activities. Several common themes emerged, including doing a complete dictation on every patient, seeing as many patients as possible rather than focusing on high RVU patients, and attempting to share a teaching point with residents on every patient. It appears that these faculty members are more efficient overall and better at utilizing their time to complete tasks related to documentation and teaching.
This study supports the idea that physicians do not have to sacrifice teaching to maintain clinical productivity. Those who are efficient practicing EM are also able to teach effectively. EPs may be overwhelmed by the current volume of need facing many EDs. However, this should not be an excuse to abdicate the responsibilities owed to both the patient and the learner. The skills of those who perform both functions well must be better understood so that they can be taught to the rest of the faculty.
LIMITATIONS
This study is limited by the design of our investigation. We conducted the study at a single center and obtained a small sample size, which allows only relatively high correlations to be significant. We also feel that the use of RVU data as a marker for clinical workload may be uni-dimensional. Further multi-institutional studies are needed to better understand the relationship between RVU productivity and teaching. The metrics studied were collected over different time periods and may be subject to variation. While there is evidence that learner perception of teaching is a reasonable model, our study did not go further to determine if faculty teaching translated into resident and student learning.7 While the interview process did bring out a few recurrent themes of what high performing physicians perceived they were doing well, these providers were not actually observed to determine if their perceptions were correct.
CONCLUSION
This study found that highly efficient clinical productivity correlated with excellent resident teaching. This high level of performance did not appear to be at the expense of important measures such as patient satisfaction. Therefore, attending physicians should expect that they could maintain their current clinical workload and still provide good teaching experiences to residents and students.
Footnotes
The authors would like to acknowledge Corey Slovis and Jim Bihun for assisting with provision of data.
Supervising Section Editor: Michael Epter, DO
Submission history: Submitted: February 22, 2010; Revision received November 15, 2010; Accepted December 20, 2010.
Reprints available through open access at http://escholarship.org/uc/uciem_westjem.
Address for Correspondence: Sally Santen, MD, PhD, Emory School of Medicine, 1648 Pierce Drive, Suite 453, Atlanta, GA 30322
Email: ssanten@emory.edu
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Fields SA, Morrison E, Yoder E, et al. Clerkship directors’ perceptions of the impact of HCFA documentation guidelines. Acad Med. 2002;77:543–6. [PubMed]
2. Albritton TA, Miller MD, Johnson MH, et al. Using relative value units to measure faculty clinical productivity. J Gen Intern Med. 1997;12:715–7. [PMC free article] [PubMed]
3. Heins A, Farley H, Maddow C, et al. A research agenda for studying the effect of emergency department crowding on clinical education. Acad Emerg Med. 2005;12:529–32. [PubMed]
4. Berger TD, Ander DS, Terrell ML, et al. The impact of the demand for clinical productivity in academic emergency departments. Acad Emerg Med. 2004;11:1364–7. [PubMed]
5. Kelly SP, Shapiro N, Woodruff M, et al. The effects of clinical workload on teaching in the emergency department. Acad Emerg Med. 2007;14:526–31. [PubMed]
6. Glaser BG, Strauss AL. The Discovery of Grounded Theory Strategies for Qualitative Research.Chicago: Aldine; 1967.
7. Steiner IP, Frnac-Law J, Kelly KD, et al. Faculty evaluation by residents in an emergency medicine program: a new evaluation instrument. Acad Emerg Med. 2000;7:1015–21. [PubMed]


