| Author | Affiliation |
|---|---|
| Jayten Shook, DO | Lakeland Regional Medical Center, Department of Emergency Medicine, St Joseph, Michigan |
| Christopher Trigger, MD | Lakeland Regional Medical Center, Department of Emergency Medicine, St Joseph, Michigan |
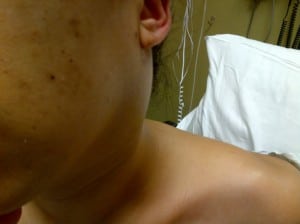
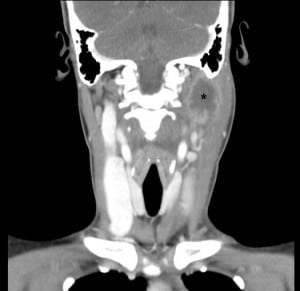
A 25-year-old woman presented to the emergency department (ED) with 4 days of progressive, left-sided neck pain and swelling. Additional symptoms included sore throat, dysphagia and left otalgia. On presentation she was tachycardic, hypotensive and had an exam notable for granular pharyngitis as well as a large area of nonfluctuant induration and swelling posterior to her left mandibular angle (Figure 1). Diffuse anterior and posterior cervical lymphadenopathy was palpable on the left. She had a white blood cell count of 13.4 with a left shift and no bandemia. A computed tomography (CT) of the neck with intravenous contrast was also performed (Figure 2).
Figure 1. Large mass on left lateral neck.
Figure 2. Coronal computed tomography of the neck with contrast demonstrating a 3.3 cm loculated abscess (*) in the left posterior triangle with adjacent cervical adenitis and left internal jugular vein occlusion.
Lemierre’s syndrome, also called postanginal septicemia, is a rare but potentially fatal disease characterized by septic thrombophlebitis of the internal jugular vein. Affected patients are typically young, otherwise healthy individuals with a recent history of tonsillitis (37%) or pharyngitis (30%) followed by severe sepsis. 1–2 Patients often present with complaints of sore throat, neck pain or neck mass as well as bone and joint pain related to septic emboli. The primary infection progresses to abscess formation within 1–3 weeks, facilitating invasion of the parapharyngeal space and internal jugular vein, leading to septic thrombophlebitis. The disease is often complicated by septic emboli traveling to the lungs and large joints. Isolated organisms include anaerobic pathogens, with Fusobacterium necrophorum being the most common.2
Early recognition and treatment are crucial as the mortality rate in untreated individuals approaches 17%. Antibiotic treatment should include intravenous anaerobic coverage with metronidazole or clindamycin which can be transitioned to oral with minimum treatment duration of 3 weeks. Anticoagulation in Lemierre’s syndrome remains controversial but should be considered if thrombosis extension is noted clinically.2 The imaging modality of choice is a contrast enhanced CT of the neck. Radiologic findings include intraluminal venous filling defects and peripheral rim enhancement of the involved segment which can measure 10–20 cm in length and most frequently includes complete occlusion.3
Footnotes
Address for Correspondence: Jayten Shook, DO, Lakeland Regional Medical Center, Department of Emergency medicine, 1234 Napier Ave, St Joseph, MI 49085. Email: jshook@lakelandregional.org. 3 / 2014; 15:125 – 126
Submission history: Revision received November 19, 2013; Accepted December 9, 2013
Conflicts of Interest : By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Karkos PD, Asrani S, Karkos CD, et al. Lemierre’s syndrome: A systematic review. Laryngoscope. 2009;119:1552-1559.
2. Johannesen K, Bødtger U, Heltberg O. Lemierre’s syndrome: the forgotten disease. J Thromb Thrombolysis. 2013 May 18.
3. Kim BY, Yoon DY, Kim HC, et al. Thrombophlebitis of the internal jugular vein (Lemierre syndrome): clinical and CT findings. Acta Radiol. 2013; 54:622-627.