| Author | Affiliation |
|---|---|
| Nathan J. Cleveland, MD, MS | Department of Emergency Medicine, University of Nevada School of Medicine, Las Vegas, Nevada |
| Melissa Beckmann, MD | Department of Emergency Medicine, University of Nevada School of Medicine, Las Vegas, Nevada |
ABSTRACT
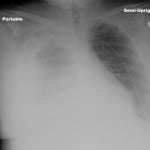
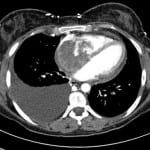
A 28-year-old female was transferred to the emergency department from her physician’s office for further evaluation of tachycardia. She was being seen for a recent illness which included nausea, vomiting, diarrhea and fevers. The patient endorsed fatigue, dyspnea on exertion, and extremity edema. She had no chest pain or cough. Exam revealed a pale, fatigued, mildly ill-appearing female with bilateral lower extremity edema and diminished breath sounds on the right. Chest radiograph revealed a large right pleural effusion (Figure 1). Computed tomographic angiography of the chest was performed (Figure 2).
Figure 1. Portable semi-upright chest radiograph showing large right pleural effusion.
Figure 2. Axial computed tomography angiogram of the chest showing intracardiac contrast-filling defect with an associated right-sided pleural effusion.
DIAGNOSIS
Cardiac Sarcoma
This is a rare form of primary invasive malignant tumor of the heart. Most cardiac tumors are secondary.1 Of primary tumors, benign myxomas are the most common.2 About 25% of primary cardiac tumors are malignant with 95% of those being sarcomas.3 Sarcomas often invade into adjacent structures including the myocardium, valves, vena cava and pericardium.3
The differential diagnosis for intracardiac contrast-filling defects includes thrombus, tumor and vegetations from endocarditis.4 Echocardiography, angiocardiography and magnetic resonance imaging may also be helpful in establishing a diagnosis.1,3 Large intracardiac tumors frequently result in inflow/outflow obstruction which can precipitate heart failure.2
Treatment of this condition is primarily operative.5 Heart transplantation (including autotransplantation) may even be necessary.5 Cardiac sarcomas often recur after resection. Post-surgical chemotherapy and radiation are of limited benefit.6
Our patient underwent surgical resection of the tumor, replacement of the tricuspid valve and reconstruction of the vena cava. She survived for several weeks after surgery but eventually succumbed to her illness.
Footnotes
Address for Correspondence: Nathan J. Cleveland, MD, MS, Department of Emergency Medicine, University of Nevada School of Medicine, Las Vegas, Nevada. Email: nathanjcleveland@gmail.com. 3 / 2014; 15:123 – 124
Submission history: Revision received November 25, 2013; Accepted December 10, 2013
Conflicts of Interest : By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Shapiro LM. Cardiac tumors: Diagnosis and management. Heart. 2001;85:218-222.
2. Butany J, Nair V, Naseemuddin A, et al. Cardiac tumours: diagnosis and management. Lancet Onc. 2005;6:219-228.
3. Sheppard MN, Mohiaddin R. Tumors of the heart. Future Cardiol. 2010;6:181-193.
4. Price S. Endocarditis: the complementary roles of CT and echocardiography. Br J Cardiol. 2012;19:7-9.
5. Blackmon SH, Reardon MJ. Surgical Treatment of Primary Cardiac Sarcomas. Tex Heart Inst J. 2009;36:451-452.
6. Putnam JB, Sweeney MS, Colon R, et al. Primary cardiac sarcomas. Ann Thorac Surg. 1991;51:906-910.