| Author | Affiliation |
|---|---|
| Zachary Levy, MD | Christiana Care Health System, Emergency Medicine Residency Program, Newark, Delaware |
| James Carroll, MD | Christiana Care Health System, Emergency Medicine Residency Program, Newark, Delaware |
| Heather Farley, MD | Christiana Care Health System, Emergency Medicine Residency Program, Newark, Delaware |
ABSTRACT
Acute prevertebral calcific tendonitis (APCT) is a rare condition, the exact incidence of which is unknown. It is of particular interest to the emergency physician owing to the other potentially devastating conditions in the differential diagnosis of neck stiffness and/or odynophagia (including retropharyngeal abscess, infectious spondylitis, and meningitis.) In contrast, APCT has a benign clinical course and can be easily managed in the emergency department. We will present a case of APCT, followed by a brief discussion of the disease and current literature.
CASE
A 66-year-old male presented to our emergency department (ED) with a chief complaint of nuchal rigidity and odynophagia. He had been seen earlier in the day by his primary care physician, who subsequently referred him to the emergency department for further work-up.
The patient reported that he had been in his usual state of health until 2 days before his visit, when he experienced the somewhat rapid onset of diffuse neck pain and stiffness, followed by significant pain upon swallowing and a nonproductive cough. He reported no chest pain, shortness of breath, headache, nausea, or vomiting. He did, however, report an intermittent low-grade fever at home since the onset of his symptoms. He reported no significant recent illness or hospitalization. His past medical history was notable only for hyperlipidemia and hypertension, both controlled by medications. He had no known drug allergies and was a nonsmoker.
On arrival, his vital signs were as follows: temperature (oral), 37.3°C; pulse, 97 beats per minute; respirations, 16 per minute; blood pressure, 125/91. His oxygen saturation was 96% on room air. On examination, he was awake, alert, oriented, and in no acute distress. He was able to phonate and was protecting his airway without difficulty. He had marked nuchal rigidity, which was associated with lateral soft tissue neck tenderness. His oropharyngeal examination was somewhat limited secondary to mild trismus, but there was no evidence of tonsilar exudate or peritonsilar abscess. There was no lymphadenopathy. His lungs were clear bilaterally. The remainder of his physical examination was unremarkable.
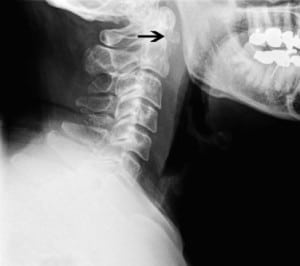
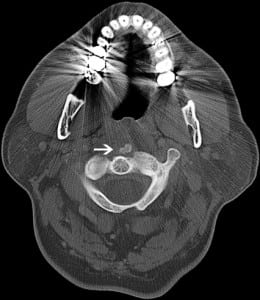
Lateral soft-tissue radiographs of his neck (Figure 1) revealed prominent prevertebral soft tissues with patent hypopharyngeal and proximal tracheal air columns. The epiglottis was unremarkable and no unusual gas patterns were present; however, abnormal ossification was noted along the inferior aspect of the anterior arch of C1. This prompted follow-up imaging with computed tomography of the neck (Figure 2), which showed an 8-mm retropharyngeal calcific focus with a small, nonloculated, fluid collection along the anterior aspect of the longus colli. Based on these findings, a diagnosis of acute prevertebral calcific tendonitis (APCT) was made.
The patient received 15 mg of intravenous ketorolac in the emergency department. Shortly afterwards, he reported marked alleviation of his symptoms and was able to tolerate per os fluids without difficulty. After a discussion with the on-call otolaryngologist, the patient was discharged home with a prescription for oral non-steroidal anti-inflammatory drugs (NSAID) and a recommendation for outpatient follow-up in the ear, nose, and throat clinic in 1 to 2 weeks as needed. The patient subsequently reported complete pain relief with oral NSAID therapy.
DISCUSSION
The longus colli traverses the anterior spinal column from C1 to T3 and is divided into 3 portions: superior oblique, inferior oblique, and vertical. Acute prevertebral calcific tendonitis (alternatively referred to as retropharyngeal tendonitis and longus colli tendonitis) is an inflammatory calcification of the longus colli and was first mentioned in 1964 when Hartley1 described a “large amorphous calcium deposit just anterior to the atlanto-axial joint.” Since that time, the disease has remained relatively obscure, and research on the subject has consisted primarily of case reports (although Hviid et al2 have suggested that this obscurity is primarily the result of underrecognition.)
Seventy-six patients diagnosed with APCT have been identified in the existing literature; in this group, the disease shows a slight female predominance (∼58%), with the average age of onset being 46 years. This is fairly consistent with the epidemiology intimated in prior reports,3 in which the disease is often described as afflicting females in the third through sixth decade of life.
The exact pathogenesis of the condition is unknown, although it is believed to be similar to other forms of tendinitis that occur in the body owing to hydroxyapatite deposition, dystrophic calcification, and subsequent inflammatory response.4 In particular, it is strikingly similar in epidemiology, pathogenesis, and clinical course to the equally obscure “crowned dens syndrome,” which involves calcification of the ligaments surrounding the odontoid process.5 Although typically occurring in the anterior C1 to C3 region, APCT has also been described at C5 to C6,6 at the origin of the vertical portion of the longus colli.
In APCT, nuchal rigidity and odynophagia are the 2 most commonly reported chief complaints. Fever and leukocytosis may be present,7 as well as elevated levels of C-reactive peptide,8 often prompting a more extensive work-up in search of an infectious etiology. Imaging will usually demonstrate the pathognomonic calcium deposit9 and, coupled with the physical examination, will usually allow the clinician to confirm the diagnosis. Computed tomography is more sensitive7 than plain radiography for detecting the condition, owing to better contrast resolution, and is the confirmatory scan of choice. Plain films, however, will often end up being the initial screening examination and will demonstrate a significantly abnormal expansion of the retropharyngeal space (by as much as 1.5 to 2.0 cm, as reported by Haun9), with or without visible calcification. Use of magnetic resonance imaging (MRI) has also been described, showing characteristic edema confined to the longus colli.10 Vollmann et al11 have suggested that MRI with diffusion-weighted imaging is the preferred modality when available.
The clinical course of APCT appears universally benign and self-limited,12 in that no fatalities or significant complications have been described; however, the sample size on which this assumption is based is quite small, and the possibility of significant airway compromise cannot be entirely dismissed. Nevertheless, symptoms resolve in about 1 to 2 weeks, correlating with calcium deposit resorption9 (although the resorption process itself may not be radiologically complete for several months.) As mentioned above, oral NSAIDs are the hallmark of outpatient treatment and are usually sufficient monotherapy for pain control. Occasionally, a short course of corticosteroidsa13 may be appropriate when NSAIDs provide suboptimal relief. Follow-up with an otolaryngologist may be offered but is usually unnecessary.
Footnotes
Supervising Section Editor: Sean Henderson, MD
Submission history: Submitted April 9, 2011; Accepted April 18, 2011
Reprints available through open access at http://escholarship.org/uc/uciem_westjem
DOI: 10.5811/westjem.2011.4.6766
Address for Correspondence: Zachary Levy, MD
Christiana Care Health System, Emergency Medicine Residency Program, 4755 Ogletown-Stanton Rd, Newark, DE 19713
E-mail: levy.zachary@gmail.com
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding, sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Hartley J. Acute cervical pain associated with retropharyngeal calcium deposit a case report. J Bone Joint Surg Am. 1964;46:1753–1754. [PubMed]
2. Hviid C, Salomonsen M, Gelineck J, et al. Retropharyngeal tendinitis may be more common than we think: a report on 45 cases seen in Danish chiropractic clinics. J Manipulative Physiol Ther.2009;32:315–320. [PubMed]
3. Shin DE, Ahn CS, Choi JP. The acute calcific prevertebral tendinitis: report of two cases. Asian Spine J. 2010;4:123–127. [PMC free article] [PubMed]
4. Ring D, Vaccaro AR, Scuderi G, et al. Acute calcific retropharyngeal tendinitis: clinical presentation and pathological characterization. J Bone Joint Surg Am. 1994;76:1636–1642.[PubMed]
5. Scutellari PN, Galeotti R, Leprotti S, et al. The crowned dens syndrome: evaluation with CT imaging. Radiol Med. 2007;112:195–207. [PubMed]
6. Park SY, Jin W, Lee SH, et al. Acute retropharyngeal calcific tendinitis: a case report with unusual location of calcification. Skeletal Radiol. 2010;39:817–820. [PubMed]
7. Eastwood JD, Hudgins PA, Malone D. Retropharyngeal effusion in acute calcific prevertebral tendinitis: diagnosis with CT and MR imaging. AJNR Am J Neuroradiol. 1998;19:1789–1792.[PubMed]
8. Homma Y, Itoi A, Muta T, et al. Acute posterior neck pain in adult: a case series. Cases J.2009;2:8103. [PMC free article] [PubMed]
9. Haun CL. Retropharyngeal tendonitis. AJR Am J Roentgenol. 1978;130:1137–1140. [PubMed]
10. Gelineck J, Salomonsen M, Hviid C. Retropharyngeal tendinitis: radiographic and magnetic resonance imaging findings. Acta Radiol. 2006;47:806–809. [PubMed]
11. Vollmann R, Hammer G, Simbrunner J. Pathways in the diagnosis of prevertebral tendonitis. Eur J Radiol. 2011]. published online ahead of print March 23.
12. Chung T, Rebello R, Gooden EA. Retropharyngeal calcific tendinitis: case report and review of literature. Emerg Radiol. 2005;11:375–380. [PubMed]
13. Razon RV, Nasir A, Wu GS, et al. Retropharyngeal calcific tendonitis: report of two cases. J Am Board Fam Med. 2009;22:84–88. [PubMed]


