| Author | Affiliation |
|---|---|
| Arun Nagdev, MD | Alameda County Medical Center–Highland General Hospital, Department of Emergency Medicine, Oakland, California; University of California, San Francisco, Department of Emergency Medicine, San Francisco, California |
| Jeanine Ward MD | Brown University School of Medicine, Department of Emergency Medicine, Providence, Rhode Island |
ABSTRACT
Acalculous cholecystitis is thought to occur in patients with a severe systemic illness or during long periods of intravenous nutrition. We discuss a case of acalculous cholecystitis secondary to Epstein-Barr virus detected by bedside ultrasound. We hope to alert clinicians who are actively using bedside ultrasound of an important, yet not commonly discussed, association.
INTRODUCTION
An 18-year-old woman with a history of hypothyroidism, tonsillectomy, and adenoidectomy at age 4 years presented to the emergency department (ED) with complaints of abdominal pain, diaphoresis, and fevers approximately 1 week prior to arrival. The patient had been seen in the ED 2 days prior for similar complaints. Abdominal and pelvis computed tomography scans with intravenous contrast were performed in the ED and read by an attending radiologist as negative for presence of intra-abdominal pathology. The patient returned to the ED because of continued fever and abdominal pain.
Signs and Symptoms
On her second visit, the patient was in moderate discomfort. Initial vital signs were temperature 99.7°F, heart rate 80 beats per minute, blood pressure 113/62 mm Hg, respiration rate 18 breaths per minute, oxygen saturation 96% on room air, and blood glucose level 125 mg/dL. The patient complained of continued abdominal pain, specifically in the right upper quadrant, with no nausea, vomiting, chest pain, dysuria, pelvic pain, or vaginal discharge. The patient did complain of diffuse myalgias and fevers but denied a sore throat or neck pain. The patient also had no history of being immunocompromised, had no history of recent severe infection, and was tolerating food by mouth.
Physical Examination
Initial external inspection of the abdomen was normal. Bowel sounds were active throughout the abdomen, without tenderness to light palpation. The patient’s abdomen was not peritoneal, but right upper quadrant tenderness was noted on deep palpation. The chest, cardiac, and pelvic examinations were normal. The patient did not have any lymphadenopathy or scleral icterus. Despite being status-post tonsillectomy, the rest of her oropharyngeal examination was otherwise normal.
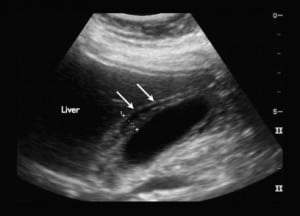
The emergency physician performed a bedside ultrasound examination in an attempt to determine the presence of acute cholecystitis as the cause of the right upper quadrant tenderness. The examination indicated no gallstones but a thickened gallbladder wall (greater than 1 cm) with mild pericholecystic fluid, making the diagnosis of acute cholecystitis secondary to gallstones unlikely. The common bile duct was measured to be 4 mm in diameter (Figure). Her white blood cell count was 10.4 K/μL on admission, without presence of immature cells. Her aspartate aminotransferase was 118 IU/L, alkaline phosphatase 146 IU/L, bili total 1.2 mg/dL, and bili direct 0.6 mg/dL on admission. Her serum lipase was normal.
A monospot was sent from the ED based on the patient’s signs and symptoms of a diffuse viral illness with signs of acalculous cholecystitis. After surgical consultation, the patient was eventually admitted to the medical service for supportive therapy and confirmatory testing. The patient was started on antibiotics (Zosyn 3.375 mg intravenously every 6 hours) based on the uncertain cause of the acalculous cholecystitis without confirmatory viral testing.
During the patient’s hospital stay, the Epstein-Barr viral antigen IgG returned negative, but the viral antigen IgM was positive, indicating an acute infectious process. Her hospital course was uneventful, consisting of supportive therapy, with the patient discharged after 5 days.
DISCUSSION
Acalculous cholecystitis secondary to an Epstein-Barr virus (EBV) infection is an uncommon entity, with only 4 previous cases (all since 2007) being reported in the general medical literature.1 Our case is the first to be detected in the ED with the aid of bedside ultrasound. Generally, acalculous cholecystitis occurs secondary to sepsis, total parenteral nutrition, or gallbladder dysmotility due to primary gallbladder infection (ie, Salmonella, Staphylococcus, Brucella, cytomegalovirus, or cryptosporidium).2,3 Rarely occurring in previously healthy young adults, acalculous cholecystitis can be a diagnostic challenge for the clinician unfamiliar with its association with EBV.
A paucity of information is available detailing the mechanism of EBV-induced acalculous cholecystitis. The presumed mechanism is thought to be either EBV-associated bile stasis with resultant gallbladder inflammation or direct viral gallbladder invasion.4,5 Ultrasound findings of acalculous cholecystitis include gallbladder wall thickening (greater than 4 mm) and/or pericholecystic fluid.1 Emergency physicians commonly searching for gallstones when performing a gallbladder examination should be aware of subtle findings of acalculous cholecystitis when evaluating patients with suspected gallbladder disease, especially young patients with signs and symptoms of a diffuse viral illness and a mild to moderate transaminitis. Historically, acalculous cholecystitis is treated with antibiotics and/or cholecystectomy, but no clear treatment plan exists for viral acalculous cholecystitis. Antibiotic therapy is not recommended after viral confirmation but may not be clear to the emergency provider during the initial evaluation. Also, in all previous cases, patients required inpatient admission without surgical intervention, but these guidelines are based on only 4 cases, and repeat ultrasounds to determine resolution of disease may be prudent.1,4
With an increasing number of emergency physicians integrating bedside ultrasound into their practice, we hope to alert the clinician of an unrecognized cause of acalculous cholecystitis. Acalculous cholecystitis can be a critical condition in seriously ill elderly patients, but minimal outcome data have been reported in acute viral episodes in previously healthy young individuals. Currently, early detection and supportive therapy may be the mainstay of treatment once the etiology is determined, since all reported cases have not needed surgical intervention. Emergency physicians should be aware of the association of acalculous cholecystitis and EBV infection when performing bedside ultrasound in the evaluation of the patient with abdominal pain.
Footnotes
Supervising Section Editor: Seric S. Cusick, MD
Submission history: Submitted March 20, 2010; Revision received June 6, 2010; Accepted July 12, 2010
Reprints available through open access at http://escholarship.org/uc/uciem_westjem
DOI: 10.5811/westjem.2010.7.1914
Address for Correspondence: Arun Nagdev, MD
Alameda County Medical Center–Highland General Hospital, Department of Emergency Medicine, 1411 E 31st St, Oakland, CA 94602
E-mail: arunnagdev@gmail.com
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Iaria C, Arena L, Di Maio G, et al. Acute acalculous cholecystitis during the course of primary Epstein-Barr virus infection: a new case and a review of the literature. Int J Infect Dis. 2008;;12:391–395. [PubMed]
2. McChesney JA, Northup PG, Bickston SJ. Acute acalculous cholecystitis associated with systemic sepsis and visceral arterial hypoperfusion: a case series and review of pathophysiology. Dig Dis Sci.2003;;48:1960–1967. [PubMed]
3. Shridhar Ganpathi I, Diddapur RK, Eugene H. et al. Acute acalculous cholecystitis: challenging the myths. HPB (Oxford) 2007;;9(2):131–134. [PMC free article] [PubMed]
4. Prassouli A, Panagiotou J, Vakaki M, et al. Acute acalculous cholecystitis as the initial presentation of primary Epstein-Barr virus infection. J Pediatr Surg. 2007;;42:E11–E13. [PubMed]
5. Lagona E, Sharifi F, Voutsioti A, et al. Epstein-Barr virus infectious mononucleosis associated with acute acalculous cholecystitis. Infection. 2007;;35:118–119. [PubMed]


