| Author | Affiliation |
|---|---|
| Ryan Patrick Radecki, MD | The University of Texas Health Science Center at Houston, Department of Emergency Medicine, Houston, Texas |
ABSTRACT
Introduction:
The efficacy of thrombolytic therapy for acute ischemic stroke remains controversial in emergency medicine and has not been fully endorsed by either the American College of Emergency Physicians or the American Academy of emergency medicine. A growing recognition exists of the influence of pharmaceutical sponsorship on the reported findings of published clinical trials. Sponsorship bias has been suggested as a potential criticism of the literature and guidelines favoring thrombolytic therapy. The objective of this study is to review the most influential literature regarding thrombolytic therapy for acute ischemic stroke and document the presence or absence of pharmaceutical sponsorship.
Methods:
A publication-citation analysis was performed to identify the most frequently cited articles pertaining to thrombolytic therapy for acute ischemic stroke. Identified articles were reviewed for disclosures of pharmaceutical funding.
Results:
Of the 20 most-cited articles pertaining to thrombolytic therapy for acute stroke, 17 (85%) disclosed pharmaceutical sponsorship. These disclosures range from general sponsorship to direct employment of authors by pharmaceutical companies.
Conclusion:
An overwhelming predominance of the most influential literature regarding thrombolytic therapy for acute ischemic stroke is susceptible to sponsorship bias. This potential bias may provide a basis for physician concern regarding the efficacy and safety of thrombolytic therapy. Further, large, independent, placebo-controlled studies may be required to guide therapy and professional guidelines definitively for acute ischemic stroke.
INTRODUCTION
Stroke is one of the leading causes of death and disability in developed countries.1 Recombinant tissue plasminogen activator (rTPA) is an approved thrombolytic therapy for use in acute ischemic stroke, approved by the Food and Drug Administration in 1996 and endorsed in guidelines from the American Heart Association (AHA).2,3 However, 15 years after the original National Institute of Neurologic Disorders Study (NINDS) of rTPA for acute stroke, only 2% to 3% of eligible patients receive thrombolytic treatment.4
A 2006 survey of members of the American College of Emergency Physicians (ACEP) found that 40% of physicians would not use thrombolytic therapy for acute stroke, even under ideal conditions.5 The professional societies ACEP and the Academy of Academic Emergency Medicine (AAEM) decline to endorse thrombolytic therapy fully as the standard of care.6,7 One source of reticence to the use of thrombolytic therapy stems from concern over the role of pharmaceutical financial interests in establishing treatment guidelines.8,9 Critics cite Genentech contributions to the AHA totaling $11 million in the years preceding the issuance of stroke guidelines; a majority of panelists voting on the guidelines had ties to Genentech. More recently, the AHA has again come under scrutiny for extensive conflicts of interest in their Clinical Practice Guidelines, raising “disturbing questions about the independence and reliability” of the guidelines.10,11 The influence of financial ties is well documented in the medical literature, with meta-analyses and systematic reviews showing strong associations between pharmaceutical funding and favorable published outcomes.12,13
The goal of this study was to describe the role, if any, of pharmaceutical financial interests in the medical literature regarding the use of thrombolytic therapy in acute stroke. Citation analysis is an accepted, if controversial, method for evaluating the impact of journals and faculty.14,15 Although not specifically described in the literature as applied to individual articles, the same principles were extended in an attempt to identify the most influential literature regarding the use of thrombolytic therapy in acute ischemic stroke. The ISI Web of Science® citation index was chosen because of ease of use and completeness relative to competing sources.16 Each article was reviewed for financial interests associated with the publication, and the results used to discuss the potential conflict of interest this may represent.
METHODS
An Internet search for articles concerning the use of thrombolytic therapy for acute stroke was undertaken in February 2011 at the ISI Web of Science web site. “All years” of the Science Citation Index-Expanded database from 1945 to the present was searched by using the following search string: “Title=(stroke AND (thrombolysis OR thrombolytic OR TPA OR rTPA OR rt-PA OR tissue-plasminogen OR plasminogen OR alteplase OR desmoteplase OR prourokinase OR streptokinase)) AND Document Type=(Article OR Proceedings Paper).” The resulting search results were sorted in descending order by the number of citations. After a qualitative reading, articles that did not report on efficacy of thrombolysis as an intervention for acute stroke were excluded. Twenty articles with the highest citation counts from this remaining set were included for analysis.
Each article was reviewed for mention of pharmaceutical financial disclosures. A pharmaceutical financial interest was judged to be present if the text of the publication reported:
- Direct or indirect funding of a study by the pharmaceutical company manufacturing the study drug.
- The pharmaceutical company manufacturing the study drug was involved in subject recruitment and site monitoring.
- Any study authors or members of the study group reported as a conflict of interest disclosure of receiving employment by, professional association with, or receipt of honoraria or grant funding from the pharmaceutical company manufacturing the study drug.
Provision of the study drug without mention of other study involvement was judged not to represent significant disclosure.
RESULTS
Initial search for the query string on the ISI Web of Science showed 2,513 results. These results were ordered by number of citations. One of the initial top 20 results concerned risk of stroke and circulating endogenous tissue plasminogen activator and was excluded.17 A second article present in the top 20 results concerned neuroradiologic features of ischemic stroke and was excluded.18 The subsequent top 20 search results constituted the main results and are listed in Table 1.

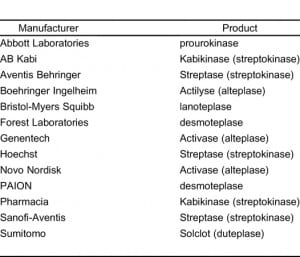
Pharmaceutical financial disclosures are noted in 17 (85%) of 20 articles reviewed. The companies named in disclosures for each publication are listed in the table. If multiple companies are listed in disclosures, they are listed in alphabetic order. A guide to manufacturers of tissue plasminogen activator study drugs used in these studies is listed in Table 2. All publications reporting disclosures had at least 1 disclosure involving the pharmaceutical company manufacturing the study drug.
The type of disclosure identified in each article is shown in Table 1. Of the articles with no disclosures, 1 was funded by the Burroughs-Wellcome Company, an independent scientific sponsor without industry associations.19 The other 2 articles judged to have no significant disclosures each received a supply of study medication. The first specifically states the supplier did not participate in data monitoring or data analysis. The last makes no disclosures related to sponsorship. However, although not providing a specific statement clarifying a lack of conflict of interest, no further information is available, and it will be assumed for the purposes of this article that none exists.
DISCUSSION
A worrying level of pharmaceutical financial disclosure is associated with the literature regarding thrombolysis in acute stroke. Although pharmaceutical sponsorship is critical to the approval of new medical therapies and the advancement of medical sciences, this influence raises an unavoidable specter of sponsorship bias. Sponsorship bias has been associated with restriction of publication of negative results, alteration of the primary outcomes after study completion, decreased adverse event reporting, and discordance between author conclusions and statistical results.20–23 A meta-analysis revealed that industry funding is significantly associated with greater chances of pro-industry results, with an odds ratio of 3.60 (95% confidence interval, 2.63–4.91). The degree to which sponsorship bias is present in the reviewed studies represents the extent to which this literature may mislead clinicians regarding the safety and efficacy of thrombolysis in acute stroke. It has been stated, “The real scandal in acute stroke care is not that thrombolytic therapy is being used, but that it is not being used often or wisely enough.”24 A possible barrier to physician adoption of stroke guidelines, following from the pervasiveness of pharmaceutical funding, may be suggested to have roots in physician distrust of the results.25
In a specific example, based on the European Cooperative Acute Stroke Study (ECASS III), the time window for treatment of acute stroke is now expanded beyond the original 3 hours, allowing treatment up to 4.5 hours after stroke onset.26 Review of the disclosures for the ECASS III publication indicates that the study was sponsored by Boehringer Ingelheim, the manufacturer of the study drug. Several authors of the study serve as paid consultants to Boehringer Ingelheim, receive financial honoraria from Boehringer, or receive grant funding support from Boehringer. Additionally, other authors of the study are directly employed by Boehringer. Although none of these disclosures proves a lack of integrity in the reporting of results, it is prudent to interpret the reported outcomes with caution, given the multifactorial risk of sponsorship bias.
A second barrier to the use of thrombolytic therapy remains controversy within the specialty of emergency medicine. The ACEP clinical policy regarding use of thrombolytic therapy in acute stroke states that further data are needed to define patients who will clearly benefit from thrombolytics, and that insufficient evidence exists to support thrombolytic use outside the conditions described in NINDS. The AAEM policy statement specifically alludes to the financial interests at work in the guidelines. Additional authors suggest caution regarding the AHA guidelines, with the contention that the NINDS study was too small, and that baseline differences are found between the treatment and placebo groups in both NINDS and ECASS III that account for the entire apparent treatment effect.27,28
Of further concern to physicians, despite the apparent benefit, may be the magnitude of the harm. Intracranial hemorrhage is a grave and frequently fatal complication of thrombolytic therapy, and many physicians may be hesitant to associate themselves with this readily observable deterioration. Emerging data appear to show that elderly patients are at significantly higher risk for deterioration with thrombolytic therapy.29 It may be prudent for proponents of thrombolytic therapy to focus on narrowing the treatment group to patients with more-favorable risk/benefit profiles, rather than seeking to expand the potential treatment group through time-window extension.
Proponents of thrombolytic therapy may argue that it is unethical to withhold an approved and “proven” treatment from stroke victims to perform further trials. However, a favorable outcome may have a positive effect on widespread adoption of thrombolytic therapy. This resulting increase in the use of thrombolytics may benefit countless stroke victims who might be denied therapy at present, far outnumbering the cohort of patients who would be enrolled in an additional clinical trial. An independent, randomized, controlled trial, such as the ongoing International Stroke Trial-3,30may bring clarity.
Last, despite the ongoing controversy over efficacy, guideline-directed thrombolytic therapy is in use for acute stroke. Its approval by the AHA as “definitely recommended” (Class I) therapy places individual physicians at risk for litigation; physicians have been successfully sued both for use of thrombolytic therapy in acute stroke and for its omission.31 Professional organizations should take leadership roles in protecting their constituents from litigation. This includes encouraging further research to quell debate over efficacy, as well as issuing clear guidance on the standard of care that aids physician defense during litigation.
LIMITATIONS
This study has several limitations. Citation count in the Web of Science is used as a surrogate marker for influence over physician perception and decision making. It has been used to define journal impact factor and as a tool in evaluating faculty performance; however, citation count is not described as a method to similarly quantify the influence of individual articles.
Citation analysis by this method skews results by publication age, as publications that have been available longer are more likely to have increased numbers of citations. This is most apparent when observing that only 5 of the 20 articles reviewed were published in the last decade, whereas the remaining 15 are more than 10 years old. Whereas articles published longer in the past may form the foundation for current research and standard of care, their actual influence over physician perception and decision making may be limited, as they, theoretically, reflect fewer contemporary data and less practice.
The documentation of pharmaceutical financial disclosures is limited to that specifically stated in publication. Omissions, unintentional or not, from the publication text may underrepresent the degree to which pharmaceutical interests influence the study.
Only 20 articles were reviewed for this analysis, rendering the results more qualitative than quantitative.
CONCLUSION
Pharmaceutical financial disclosures are prevalent in the investigation of thrombolytic therapy for acute stroke. Evidence from reviews of sponsorship bias suggests that it is reasonable to question the outcomes as interpreted in these studies. Individual physicians and professional associations should encourage further independent, randomized, controlled study of this intervention.
Footnotes
Supervising Section Editor: John Sarko, MD
Submission history: Submitted December 29, 2010; Revision received March 9, 2011; Accepted May 5, 2011
Reprints available through open access at http://escholarship.org/uc/uciem_westjem
DOI: 10.5811/westjem.2011.5.2166
Address for Correspondence: Ryan Patrick Radecki, MD
The University of Texas Health Science Center at Houston, Department of Emergency Medicine, 6431 Fannin St, Houston, TX 77030-1503
E-mail: Ryan.P.Radecki@uth.tmc.edu
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The author has no conflicts of interest, financial or otherwise, to disclose.
REFERENCES
1. Truelsena T, Ekmanb M, Boysena G. Cost of stroke in Europe. Eur J Neurol. 2005;;12((suppl 1)):78–84. [PubMed]
2. Adams HP, Jr, Adams RJ, Brott T, et al. Guidelines for the early management of patients with ischaemic stroke: a scientific statement from the Stroke Council of the American Stroke Association.Stroke. 2003;;34:1056–1083. [PubMed]
3. The European Stroke Initiative Executive Committee and European Stroke Initiative Writing Group. European stroke initiative recommendations for stroke management: update 2003.Cerebrovasc Dis. 2003;;16:311–337. [PubMed]
4. Chan YF, Kwiatkowski TG, Rella JG, et al. Tissue plasminogen activator for acute ischemic stroke: a New York City Emergency Medicine Perspective. J Emerg Med. 2005;;29:405–408. [PubMed]
5. Wals M, Fromm G. Emergency physician survey: recombinant tissue plasminogen activator for stroke. Ann Emerg Med. 2005;;47:296–297.
6. Goyal DG, Li J, Mann J, et al. Position statement on the use of intravenous thrombolytic therapy in the treatment of stroke. American Academy of Emergency Medicine Web site. Available at:http://www.aaem.org/positionstatements/thrombolytictherapy.php. Accessed April 2011.
7. ACEP Board of Directors. American College of Emergency Physicians Web site; Use of intravenous tPa for the management of acute stroke in the emergency department. Available at:http://www.acep.org/practres.aspx?id=29834. Accessed April 2011.
8. Lenzer J. Alteplase for stroke: money and optimistic claims buttress the “brain attack” campaign.BMJ. 2002;324:723–726.
9. Annual Report 1999. American Heart Association; Dallas: AHA, 2000.
10. Nissen SE. Can we trust cardiovascular practice guidelines? Arch Intern Med. 2011;;171:584–585. [PubMed]
11. Mendelson TB, Meltzer M, Campbell EG, et al. Conflicts of interest in cardiovascular clinical practice guidelines. Arch Intern Med. 2011;;171:577–584. [PubMed]
12. Bekelman JE, Li Y, Gross CP. Scope and impact of financial conflicts of interest in biomedical research: a systematic review. JAMA. 2003;;289:454–469. [PubMed]
13. Sismondo S. Pharmaceutical company funding and its consequences: a qualitative systematic review. Cont Clin Trials. 2007;;29:109–113.
14. Moed HF. New developments in the use of citation analysis in research evaluation. Arch Immunol Ther Exp. (Warsz) 2009;;57:13–18. [PubMed]
15. Pendlebury DA. The use and misuse of journal metrics and other citation indicators. Arch Immunol Ther Exp. (Warsz) 2009;;57:1–11. [PubMed]
16. Falagas ME, Pitsouni El, Malietzis R, et al. Comparison of PubMed, Scopus, Web of Science, and Google Scholar: strengths and weaknesses. FASEB J. 2008;;22:338–342. [PubMed]
17. Ridker PM, Hennekens CH, Stampfer MJ, et al. Prospective-study of endogenous-tissue plasminogen-activator and risk of stroke. Lancet. 1994;;343:940–943. [PubMed]
18. Von Kummer R, Alle KL, Holle R, et al. Acute stroke: usefulness of early CT findings before thrombolytic therapy. Radiology. 1999;;205:315–318.
19. Burroughs-Wellcome Fund. Fact sheet. Burroughs-Wellcome Fund Web site; Available at:http://www.bwfund.org/pages/58/Fact-Sheet. Accessed April 2011.
20. Popelut A, Valet F, Fromentin O, et al. Relationship between sponsorship and failure rate of dental implants: a systematic approach. PLoS ONE. 2010;;5:e10274. [PMC free article] [PubMed]
21. Golder S, Loke Y. Is there evidence for biased report of published adverse effects data in pharmaceutical industry-funded studies? Br J Clin Pharmacol. 2008;;66:767–773.[PMC free article] [PubMed]
22. Boutron I, Dutton S, Ravaud P, et al. Reporting and interpretation of randomized controlled trials with statistically nonsignificant results for primary outcomes. JAMA. 2010;;303:2058–2064.[PubMed]
23. DeAngelis CD, Fontanarosa PB. Impugning the integrity of medical science: the adverse effects of industry influence. JAMA. 2008;;299:1800–1812. [PubMed]
24. Saver J, Kidwell C, Starkman S. Commentary: thrombolysis in stroke it works! BMJ.2002;;324:727–729.
25. Glick M. Whether industry-supported or otherwise, trust is key to the acceptance of all research.JADA. 2010;;141:127–128. [PubMed]
26. Del Zoppo GJ, Saver J, Jauch EC. et al. Expansion of the time window for treatment of acute ischemic stroke with intravenous tissue plasminogen activator: a science advisory from the American Heart Association/American Stroke Association. Stroke. 2009;;40:2945–2948.[PMC free article] [PubMed]
27. Hoffman J, Schriger DL. A graphical re-analysis of the NINDS Trial. Ann Emerg Med.2009;;54:329–336. [PubMed]
28. Bluhmki E, Chamorro A, Davalos A, et al. Stroke treatment with alteplase given 3.0–4.5 h after onset of acute ischaemic stroke (ECASS III): additional outcomes and subgroup analysis of a randomized controlled trial. Lancet Neurol. 2009;;8:1095–1102. [PubMed]
29. Alshekhlee A, Mohammadi A, Mehta S. Is thrombolysis safe in the elderly? Analysis of a national database. Stroke. 2010;;41:2259–2264. [PubMed]
30. Sandercock PA, Wardlaw J, Lindley R. Third International Stroke Trial (IST-3) Internet Stroke Center Web site. Available at: http://www.strokecenter.org/trials/TrialDetail.aspx?tid=81. Accessed March 2011.
31. Weintraub M. Thrombolysis (tissue plasminogen activator) in stroke: a medicolegal quagmire.Stroke. 2006;;37:1917–1922. [PubMed]
32. [No authors listed] Tissue plasminogen activator for acute ischemic stroke. The National Institute of Neurological Disorders and Stroke rt-PA Stroke Study Group. N Engl J Med.1995;;333:1581–1587. [PubMed]
33. Hacke W, Kaste M, Fieschi C, et al. Intravenous thrombolysis with recombinant tissue plasminogen activator for acute hemispheric stroke. The European Cooperative Acute Stroke Study (ECASS) JAMA. 1995;;274:1017–1025. [PubMed]
34. Furlan A, Higashida R, Wechsler L, et al. Intra-arterial prourokinase for acute ischemic stroke. The PROACT II study: a randomized controlled trial. Prolyse in Acute Cerebral Thromboembolism.JAMA. 1999;;282:2003–2011. [PubMed]
35. Hacke W, Kaste M, Fieschi C, et al. Randomised double-blind placebo-controlled trial of thrombolytic therapy with intravenous alteplase in acute ischaemic stroke (ECASS II). Second European-Australasian Acute Stroke Study Investigators. Lancet. 1998;;352:1245–1251. [PubMed]
36. Hacke W, Donnan G, Fieschi C, et al. Association of outcome with early stroke treatment: pooled analysis of ATLANTIS, ECASS, and NINDS rt-PA stroke trials. Lancet. 2004;;363:768–774.[PubMed]
37. Clark WM, Wissman S, Albers GW, et al. Recombinant tissue-type plasminogen activator (Alteplase) for ischemic stroke 3 to 5 hours after symptom onset. The ATLANTIS Study: a randomized controlled trial. Alteplase Thrombolysis for Acute Noninterventional Therapy in Ischemic Stroke. JAMA. 1999;;282:2019–2026. [PubMed]
38. del Zoppo GJ, Poeck K, Pessin MS, et al. Recombinant tissue plasminogen activator in acute thrombotic and embolic stroke. Ann Neurol. 1992;;32:78–86. [PubMed]
39. Hacke W, Kaste M, Bluhmki E, et al. Thrombolysis with alteplase 3 to 4.5 hours after acute ischemic stroke. N Engl J Med. 2008;;359:1317–1329. [PubMed]
40. Hacke W, Albers G, Al-Rawi Y, et al. The Desmoteplase in Acute Ischemic Stroke Trial (DIAS): a phase II MRI-based 9-hour window acute stroke thrombolysis trial with intravenous desmoteplase.Stroke. 2005;;36:66–73. [PubMed]
41. Candelise L, Aritzu E, Ciccone A, et al. Randomised controlled trial of streptokinase, aspirin, and combination of both in treatment of acute ischemic stroke. Multicentre Acute Stroke Trial–Italy (MAST-I) Group. Lancet. 1995;;346:1509–1514. [PubMed]
42. Katzan IL, Furlan AJ, Lloyd LE, et al. Use of tissue-type plasminogen activator for acute ischemic stroke: the Cleveland area experience. JAMA. 2000;;283:1151–1158. [PubMed]
43. Albers GW, Bates VE, Clark WM, et al. Intravenous tissue-type plasminogen activator for treatment of acute stroke: the Standard Treatment with Alteplase to Reverse Stroke (STARS) study.JAMA. 2000;;283:1145–1150. [PubMed]
44. Alexandrov AV, Molina CA, Grotta JC, et al. Ultrasound-enhanced systemic thrombolysis for acute ischemic stroke. N Engl J Med. 2004;;351:2170–2180. [PubMed]
45. Marler JR, Tilley BC, Lu M, et al. Early stroke treatment associated with better outcome: the NINDS rt-PA stroke study. Neurology. 2000;;55:1649–1655. [PubMed]
46. Brott TG, Haley EC Jr, Levy DE, et al. Urgent therapy for stroke. Part I. Pilot-study of tissue plasminogen activator administered within 90 minutes. Stroke. 1992;;23:632–640. [PubMed]
47. Wahlgren N, Ahmed N, Davalos A, et al. Thrombolysis with alteplase for acute ischaemic stroke in the Safe Implementation of Thrombolysis in Stroke-Monitoring Study (SITS-MOST): an observational study. Lancet. 2007;;369:275–282. [PubMed]
48. Hommel M, Cornu C, Boutitie F, et al. Thrombolytic therapy with streptokinase in acute ischemic stroke. The Multicenter Acute Stroke Trial–Europe Study Group. N Engl J Med. 1996;;335:145–150.[PubMed]
49. Mori E, Yoneda Y, Tabuchi M, et al. Intravenous recombinant tissue plasminogen-activator in acute carotid-artery territory stroke. Neurology. 1992;;42:976–982. [PubMed]
50. Lewandowski CA, Frankel M, Tomsick TA, et al. Combined intravenous and intra-arterial r-TPA versus intra-arterial therapy of acute ischemic stroke: Emergency Management of Stroke (EMS) Bridging Trial. Stroke. 1999;;30:2598–2605. [PubMed]
51. Donnan GA, Davis SM, Chambers BR, et al. Streptokinase for acute ischemic stroke with relationship to time of administration: Australian Streptokinase (ASK) Trial Study Group. JAMA.1996;;276:961–966. [PubMed]


