| Author | Affiliation |
|---|---|
| Matthew J. Pirotte, MD | Loyola University Medical Center, Department of Emergency Medicine, Maywood, Illinois |
| D. Mark Courtney, MD | Northwestern Memorial Hospital, Department of Emergency Medicine, Chicago, Illinois |
| Michael J. Schmidt, MD | Northwestern Memorial Hospital, Department of Emergency Medicine, Chicago, Illinois |
| Rachel Davis Mersey, PhD | Northwestern University, Medill School of Journalism, Chicago, Illinois |
ABSTRACT
Introduction:
On March 18, 2009, actress Natasha Richardson died after a head injury. It is possible that the rate of patients presenting with mild head injury and receiving computed tomographies (CTs) may have been influenced by the Richardson event. We hypothesized that there was a statistically significant increase in the rate of census-adjusted head CTs performed for mild trauma after March 16, 2009, compared to prior to this date.
Methods:
We included all with a non-contrast head CT performed from the emergency department (ED) between March 1 and April 15, 2009, for minor trauma. The primary outcome was the census-adjusted rate of head CTs per time (# of head CTs/census). We compared the census adjusted rate for the 2 weeks prior to 2 weeks after the accident. To document media dissemination we searched Lexis-Nexis for news stories mentioning “Richardson.”
Results:
In the 2 weeks prior to March 16, 2009, the census-adjusted rate was 0.81% (95% CI 0.54–1.16) and there were no stories. The first media reports appeared on March 16, 2009, (n = 19) and quickly doubled (n = 40, n = 43) over the subsequent 2 days. The rate of CTs nearly doubled during the 2 weeks post accident 1.46% (1.10–1.91%). This absolute increase in rate percentage was statistically significant. (0.65%; 0.17 to 1.14%).
Conclusion:
The percentage of all ED patients seen with mild trauma tested with head CT almost doubled when comparing the pre-Richardson accident vs. post time periods. There was an increase in media reports of the accident that occurred rapidly after the event and peaked on day 3.
INTRODUCTION
The number of visits and length of stay in emergency departments (ED) are increasing, and so are computerized tomography (CT) use.1–4 CT of the brain is an important tool for diagnosing significant traumatic brain injury, but overuse is concerning due to the resultant increase in healthcare costs and risks of exposure to ionizing radiation.5
At the same time, the public increasingly uses popular media as a source of healthcare information. This has been shown to be true both for people actively seeking information about a particular topic and for those who passively receive information relating to health.6 Although media may be used as a source of healthcare information, the ability of the national media to report on health topics in proportion to their risk to public health has been called into question in prior studies.7
Stories in the national media relating the health problems of celebrities are common in both print and broadcast media. Celebrity involvement in a particular malady has been shown to increase media attention to that topic, as has been particularly well demonstrated with cancer.8 Anecdotally, healthcare providers at our institution reported an increase in the number of patients requesting CT of the head after minor head injury in the days and weeks following the story of actress Natasha Richardson’s tragic death on March 18, 2009. Ms. Richardson suffered what may have been an epidural hematoma after a blow to the head sustained while skiing. The story received wide attention in the national media with some outlets characterizing her condition as the “talk and die” or the “walk and die” syndrome.9–10
It may be hypothesized that some patients who sought care for mild head injury in the days and weeks following Ms. Richardson’s injury were influenced by media sources. Although there is some evidence to suggest that celebrity health issues have an impact on the health-associated behaviors of the general public,11 it is yet unclear to what effect media reports on healthcare-related topics have on short-term emergency healthcare use by the public.
We hypothesized that there would be an increase in the census-adjusted rate of head CTs (CARHCT) performed at our institution and that this increase would show some relationship to media coverage of Ms. Richardson’s injury.
METHODS
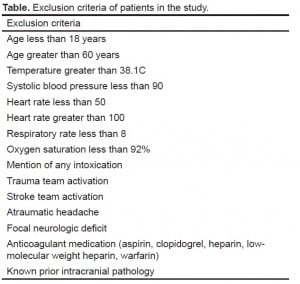
This was a retrospective chart review approved by the Institutional Review Board at Northwestern. We searched the electronic medical record database (Enterprise Data Warehouse, or EDW) at Northwestern Memorial Hospital to find patients who had a head CT performed from the ED between March 1, 2009 and April 15, 2009. We then performed chart review to exclude any patient meeting exclusion criteria in Table. Patients not excluded were considered to be those for whom a head CT had been ordered from the ED for minor head trauma and were included in the final analysis. A total of 662 patient encounters met initial screening criteria, and of those 123 were included in the final analysis. The most common reasons for exclusion were atraumatic headache and mention of a focal neurological deficit. We also collected data on daily ED census during the time period in question.
We performed statistical analysis to determine the CARHCT per day. The month following Ms. Richardson’s injury was divided into 15-day sections, and we compared the rate of CARHCTs to the 16 days prior to the injury.
To determine the frequency of media coverage of Ms. Richardson’s accident and its effect, we extracted a raw count of stories about Natasha Richardson from a purposive sample of national newspapers, network television stations, a cable news network, and a radio network. Frequency in this research was a corollary for amount of media coverage. The purposive sample was designed to represent those outlets with the largest audiences. They were the four major United States newspapers (New York Times, USA Today, Wall Street Journal, and Washington Post), the morning and evening news programs of the four national networks (ABC, CBS, NBC, and FOX), one cable news network (CNN), and one national radio network (NPR).
The unit of analysis was the individual story, defined as a news or opinion piece and excluding paid death notices, in the Lexis-Nexis Academic Universe database mentioning “Richardson” anywhere in the text or transcript. Stories that were not about Natasha Richardson (Bill Richardson, governor of New Mexico, for example) were then excluded from the data set, which ran from March 1, 2009, to April 15, 2009 (n = 193). Data collected before the accident established a baseline of media coverage.
RESULTS
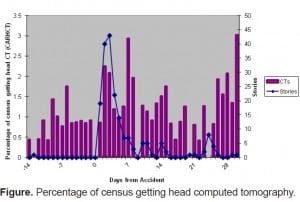
Figure 1 shows the CARHCT and the number of media stories. CARHCT in the 2 weeks leading up to the accident was 0.81% (95% confidence interval [CI] 0.54–1.16). In the 15-day period following the accident CARHCT was nearly double at 1.46% (95% CI 1.10–1.91). In the next 15-day period the CARHCT was 1.13% (95% CI 0.80–1.55). Absolute increase in CARHCT for the 30-day period prior to the accident compared to the period after was statistically significant (0.65%; 95% CI 0.17 to 1.14%).
Media reports about Ms. Richardson’s injury peaked on March 19, 2009, and quickly decreased over the next few days. During that time there was still an increase in CARHCT. All 10 news outlets covered the Richardson story, although frequency of coverage varied significantly. Only 1 story appeared in the Wall Street Journal to a high of 74 stories on CNN. Coverage peaked on March 19, 2009, at 43 stories.
DISCUSSION
We demonstrated a statistical increase in the CARHCT in a single ED in the immediate period following heavy media coverage of a celebrity injury. While similar work has been done documenting this increase in both CT and ED use, this is the first study to show a temporal relationship between media coverage and ED use.
It is unclear to what extent this increase in CARHCT was due to patient factors, clinician factors or both. Few data exist as to what extent such media attention has on clinician behavior, although it may function as a kind of bias.
Our data suggest that patient and clinician behavior continues to be affected by media stories even as the story becomes less active. More work would need to be done to explore this relationship.
LIMITATIONS
Our study has several limitations. It is retrospective and single centered. In addition, while we designed exclusion criteria meant to exclude CTs performed for obvious reasons other than minor head trauma, we did not analyze the individual clinical decisions leading up the ordering of a brain CT. It is possible that for some of the encounters in our sample neither the clinician nor the patient had ever heard of Ms. Richardson, and her accident had no bearing on their interaction. On the media side of the project, a simple count of stories about Ms. Richardson has its own set of limitations. We did not do story-level analysis for content, and as such some stories may have made little or no mention of her accident.
CONCLUSION
There was a statistically significant increase in head CT utilization in our ED following media coverage of a celebrity head injury.
Footnotes
Supervising Section Editor: John Sarko, MD
Submission history: Submitted April 4, 2012; Accepted August 13, 2012
Reprints available through open access at http://escholarship.org/uc/uciem_westjem
DOI: 10.5811/westjem.12299
Address for Correspondence: Matthew J. Pirotte. MD. Department of Emergency Medicine, 2160 S. First Ave., Maywood, IL 60153
Email: mpirotte@lumc.edu
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Derlet R, Richards J, Kravitz R. Frequent overcrowding in U.S. emergency departments. Acad Emerg Med. 2001;8:151–5. [PubMed]
2. Herring A, Wilper A, Himmelstein DU, et al. Increasing length of stay among adult visits to U.S. Emergency departments, 2001–2005. Acad Emerg Med. 2009;16:609–16.[PubMed]
3. Hospital-based Emergency Care: At the Breaking Point. National Academy of Sciences; Washington DC: 2006.
4. Korley FK, Pham JC, Kirsch TD. Use of advanced radiology during visits to US emergency departments for injury-related conditions, 1998–2007. JAMA.2010;304:1465–71. [PubMed]
5. Brenner DJ, Hall EJ. Computed tomography–an increasing source of radiation exposure. N Engl J Med. 2007;357:2277–84. [PubMed]
6. Dutta-Bergman MJ. Primary sources of health information: comparisons in the domain of health attitudes, health cognitions, and health behaviors. Health Commun.2004;16:273–88. [PubMed]
7. Bomlitz LJ, Brezis M. Misrepresentation of health risks by mass media. J Public Health.2008;30:202–4.
8. Corbett J. Medicine, media, and celebrities: News coverage of breast cancer, 1960–1995. Journalism and Mass Communication Quarterly. 1999;76:229–249.
9. Maugh T. La Times Health Blog. Los Angeles: 2009. Natasha Richardson’s condition likely due to delayed bleeding.
10. Ochs R. Chicago Tribune. Chicago, IL: 2009. Doctor: Natasha Richardson likely had ‘talk and die’ syndrome.
11. Lane DS, Polednak AP, Burg MA. The impact of media coverage of Nancy Reagan’s expereince on breast cancer screening. American Journal of Public Health.1989;79:1551–155. [PMC free article] [PubMed]