| Author | Affiliation |
|---|---|
| Jennifer G. Wilson, MD, MS | University of Calfornia San Francisco, Department of Internal Medicine, Division of Critical Care, San Francisco, California |
| Sara M. Epstein, MD | University of California San Francisco, Department of Internal Medicine, San Francisco, California |
| Ralph Wang, MD | University of California San Francisco, Department of Emergency Medicine, San Francisco California |
| Hemal K. Kanzaria, MD | University of California Los Angeles, Department of Emergency Medicine, Division of General Internal Medicine and Health Service Research, Los Angeles, California |
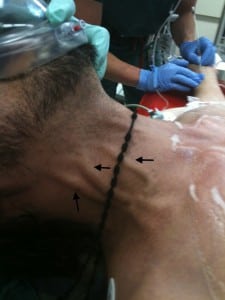
A 49-year-old man was brought to the emergency department by ambulance after he sustained a stab wound to the chest. He was alert but diaphoretic, with an initial systolic blood pressure of 90 by palpation and a heart rate of 110. A 1 cm laceration was noted at the left lower sternal border. Lung sounds were clear bilaterally, and heart sounds were muted. His cervical collar was removed, revealing distended neck veins (Figure). A bedside ultrasound demonstrated pericardial fluid (Video).
The patient had a pericardial effusion from penetrating chest trauma, causing cardiac tamponade. Cardiac tamponade is caused by fluid trapped in the pericardial space, compressing the heart, compromising ventricular filling, and therefore cardiac output.1 Acute traumatic cardiac tamponade presents with chest pain and respiratory distress.2 Beck’s triad may be present on exam, as it was in our case: muffled heart sounds, distended jugular veins, and hypotension.1 A narrow pulse pressure and pulsus paradoxus may also be observed.2 The diagnosis can be rapidly confirmed by bedside ultrasound.3 In traumatic cardiac tamponade, the treatment is thoracotomy in unstable or pulseless patientsor median sternotomy.4 Pericardiocentesis is indicated only if operative intervention is not immediately available.5 This patient was transferred directly to the operating room where a median sternotomy was performed. A 1 cm laceration to the right ventricle was identified and successfully repaired. The patient had an uneventful postoperative course and recovered well.
Footnotes
Supervising Section Editor: Sean O. Henderson, MD
Submission history: Submitted June 7, 2012; Revision received: July 5, 2012; Accepted August 3, 2012
Full text available through open access at http://escholarship.org/uc/uciem_westjem
DOI: 10.5811/westjem.2012.8.12919
Address for Correspondence: Hemal K. Kanzaria, MD, Robert Wood Johnson Foundation Clinical Scholar®, Department of Emergency Medicine, University of California Los Angeles, 10940 Wilshire Boulevard, Suite 710, Los Angeles, CA 90024. Email:hkanzaria@mednet.ucla.edu.
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Roy CL, Minor MA, Brookhart MA, et al. Does this patient with a pericardial effusion have cardiac tamponade? JAMA. 2007 Apr 25;297(16):1810–1818. [PubMed]
2. Spodick DH. Acute cardiac tamponade. N Engl J Med. 2003 Aug 14;349(7):684–690. [PubMed]
3. Boulanger BR, Kearney PA, Tsuei B, et al. The routine use of sonography in penetrating torso injury is beneficial. J Trauma. 2001 Aug;51(2):320–325. [PubMed]
4. Hunt PA, Greaves I, Owens WA. Emergency thoracotomy in thoracic trauma-a review. Injury.2006 Jan;37(1):1–19. [PubMed]
5. Karrel R, Shaffer MA, Franaszek JB. Emergency diagnosis, resuscitation, and treatment of acute penetrating cardiac trauma. Ann Emerg Med. 1982 Sep;11(9):504–517. [PubMed]