| Author | Affiliation |
|---|---|
| Chad S Kessler, MD, MHPE | The Jesse Brown VA Hospital, Department of Emergency Medicine, Chicago, Illinois |
| Andrew A Gonzalez, MD, JD, MPH | University of Illinois, Chicago, Department of Surgery, Chicago, Illinois |
| Leonard A Stallings, MD | East Carolina University, Brody School of Medicine, Departments of Emergency and Internal Medicine, Greenville, North Carolina |
| Todd A Templeman, MD | Georgetown University Hospital/Washington Hospital Center, Department of Emergency Medicine, Washington, DC |
ABSTRACT
Introduction:
This study seeks to evaluate the practice patterns of current combined emergency medicine/internal medicine (EM/IM) residents during their training and compare them to the typical practice patterns of EM/IM graduates. We further seek to characterize how these current residents perceive the EM/IM physician’s niche.
Methods:
This is a multi-institution, cross-sectional, survey-based cohort study. Between June 2008 and July 2008, all 112 residents of the 11 EM/IM programs listed by the Accreditation Council for Graduate Medical Education were contacted and asked to complete a survey concerning plans for certification, fellowship, and practice setting.
Results:
The adjusted response rate was 71%. All respondents anticipated certifying in both specialties, with 47% intending to pursue fellowships. Most residents (97%) allotted time to both EM and IM, with a median time of 70% and 30%, respectively. Concerning academic medicine, 81% indicated intent to practice academic medicine, and 96% planned to allocate at least 10% of their future time to a university/academic setting. In evaluating satisfaction, 94% were (1) satisfied with their residency choice, (2) believed that a combined residency will advance their career, and (3) would repeat a combined residency if given the opportunity.
Conclusion:
Current EM/IM residents were very content with their training and the overwhelming majority of residents plan to devote time to the practice of academic medicine. Relative to the practice patterns previously observed in EM/IM graduates, the current residents are more inclined toward pursuing fellowships and practicing both specialties.
INTRODUCTION
In 1991, the American Board of Emergency Medicine (ABEM) and the American Board of Internal Medicine (ABIM) first approved requirements for a combined residency as a means of preparing trainees “for practice/academic careers addressing the spectrum of illness and injury from the emergent to the chronic.”1 However, nearly 2 decades later, there are only 11 combined emergency medicine/internal medicine (EM/IM) residency programs in the country. In the 2009 match, there were 87 applicants, including allopathic, osteopathic, and international candidates who applied for the 24 combined EM/IM positions nationwide.2,3
In 2002, Katz and Katz4 examined the practice habits of the first 4 classes (1995–1998) of combined EM/IM residency graduates. In this cohort, the most common reason for choosing combined training was a belief that it would make the graduate a better physician. Additionally, 87% of respondents took EM board examinations and 70% took IM board examinations. Finally, although only 30% of EM/IM graduates reported practicing both specialties, 48% would have preferred a practice incorporating both EM and IM.4
Recent research by Kessler et al1 reexamined practice patterns of graduates between 1998 and 2008. While 37% of responding graduates practiced both specialties, the bulk of clinical time was spent practicing EM. While the study of Katz and Katz4 showed that only 4% of respondents enter a fellowship, the graduate study of Kessler et al1 showed that nearly a quarter had pursued a fellowship. Lastly, in the cohort of Kessler et al,1 69% of graduates devoted at least 10% of their time to academic medicine, compared to 43% in the Katz and Katz study.4
To date there are no published studies detailing the practice patterns of EM/IM physicians during residency training. This study investigates the extent to which current EM/IM residents (1) plan to enter academics, (2) believe that it is feasible to practice both EM and IM, and (3) contemplate pursuing fellowship training. Taken together, these data will help to shed light on the EM/IM physician niche as perceived by residents during training. Ultimately, these findings can provide some insight into the difference between in-training ideology and in-practice reality. Such insight would likely prove quite useful to medical students considering pursuing an EM/IM residency.
METHODS
Study Design and Population
This is a multi-institution, cross-sectional, survey-based cohort analysis. A pilot survey was distributed to postgraduate years 1 through 5 (PGY-1–PGY-5) residents in the combined EM/IM residency. From the pilot survey, 21 questions were selected for the final survey. The final survey covered demographics, certification plans, desire to pursue fellowship training, desired practice setting (location, specialty, academic affiliation), residency satisfaction, and preparation for practice (see online supplement).
Between June 2008 and July 2008, the final survey was e-mailed to all 112 residents of the 11 EM/IM programs listed by the Accreditation Council for Graduate Medical Education during the 2007–2008 academic year.5–7 Owing to the response time lag, some residents had graduated by the time of survey completion. The responses for these residents were excluded from this current study and have been previously reported in the EM/IM graduate study of Kessler et al.1 For practice setting, 1 resident was excluded from analysis because the sum of this resident’s academic and community time exceeded 100%. Two residents were also excluded from analysis of geography preference on similar grounds.
Additionally, the resident cohort did not include trainees who had already completed their primary EM/IM residency and were in a fellowship year as part of a “5+1”-year EM/IM/critical care program. Follow-up e-mails via residency program directors and coordinators were sent to nonrespondents within 2 weeks if the survey was not completed. Participation in the study was completely voluntary and unremunerated. The University of Illinois at Chicago Institutional Review Board waived the project from review.
We used Microsoft Excel (Redmond, Washington) to compile results and to calculate mean, standard deviation, median, and mode for the quantitative data. We used the Statistical Package for the Social Sciences software (SPSS, Inc, Chicago, Illinois) to calculate frequencies and descriptive statistics. We applied a chi-square analysis to assess the association between intent to practice academic medicine and enter a fellowship and compared current residents and 1998–2008 graduates about fellowship intentions, willingness to repeat an EM/IM residency, and belief that an EM/IM residency has advanced their career. Similarly we compared associations between fellowship intention, inclination to practice academic medicine, satisfaction, and PGY.
We also used statistical analysis to assess the differences between residents who intended academic careers versus those who did not, with respect to time devoted to (1) EM versus IM, (2) academic institutions versus community institutions, and (3) urban versus suburban versus rural geographic locations.
Statistical significance for differences in use of time was also assessed between current resident expectations and the 1998–2008 graduates. It is important to note that the survey tools used for both the graduates and residents contained identical questions. This allows for some comparisons to be drawn between the resident perceptions and graduate realities. Similar statistics were calculated for residents interested in fellowship training versus those without such an inclination. Unified themes were determined via independent analysis and via a 3-author majority consensus for qualitative responses to open-ended questions.8
RESULTS
Demographics
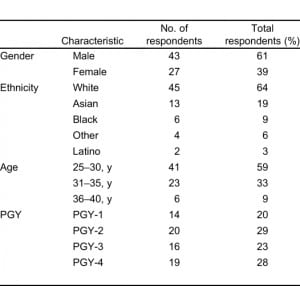
After excluding the July 2008 graduates, surveys were returned by 70 of 99 (adjusted response rate = 71%) PGY-1 through PGY-4 residents in the 11 accredited EM/IM training programs during the 2007–2008 academic year. Respondents were evenly distributed among postgraduate year. Detailed demographic data are supplied in Table 1.
Certification and Fellowship Plans
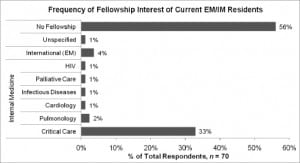
All surveyed residents anticipated gaining primary board certification in both specialties. Nearly half (n = 33; 47%) indicated an interest in pursuing subspecialty training, with 3 residents indicating multiple fellowship interests. Figure 1 presents a detailed breakdown of residents’ fellowship interest by primary certification requirement.
Fifty percent of residents (n = 28) who anticipated a career in academia planned to pursue a fellowship after residency, compared to 33% (n = 4) of residents planning a career in community practice. Of note, there is also a trend toward decreasing fellowship interest as a resident progresses through the training (50% for PGY-1 residents versus 37% for PGY-4 residents).
Intended Practice Characteristics
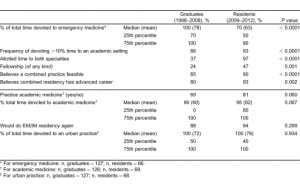
For statistical purposes, we excluded 4 residents whose total anticipated clinical time (sum of EM time and IM time) exceeded 100%. Sixty-three of 66 residents (97%) who responded to this question allotted time to both specialties. Sixty-three of 70 residents (90%) believe that it is practical to practice both EM and IM simultaneously. Forty-three residents (65%) indicated that they plan to devote more time to EM than IM, while 15 (23%) indicated that they plan to devote equal time. The median amount of time residents anticipated devoting to IM and to EM was 30% and 70%, respectively. There was no statistically significant difference (P = 0.664) in median time devoted to EM versus IM for those who intend to have an academic career (EM = 68%, IM = 33%) versus those who do not (EM = 73%, IM = 28%). There was a marginally significant (P = 0.041) difference in the median time devoted to academic medicine between residents anticipating a fellowship (95%) versus those not anticipating a fellowship (90%). Residents overwhelmingly exhibited a preference for urban, academic medical centers (Table 2).
As between residents who reported intending on a career in academic medicine versus those who did not, the former devoted more median time to an urban geographic location (100% versus 40%). Similarly, residents anticipating a fellowship versus those who did not devoted more median time to an urban geographic location (100% versus 90%). Residents most commonly anticipated acting as clinicians (n = 61; 87%) and educators (n = 26; 37%) in their future careers (Figure 2). Residents were permitted to select more than 1 practice role.
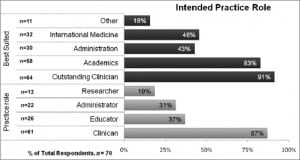
What are EM/IM Graduates Best Suited to Do?
Residents most frequently felt EM/IM training best suits graduates for clinical (n = 64; 91%) and academic (n = 58; 83%) roles. Exact percentages for other practice roles are detailed in Figure 2. Eleven residents (16%) filled in the free-response option. These replies largely fell into 3 categories: (1) ideally suited to critical care (n = 6; 55%), (2) will serve as a catalyst for integration between specialties (n = 3; 27%), and (3) will serve as a catalyst for integration between specialties and research (n = 2, 18%). Concerning integration between specialties, an archetypal response was: “[t]he EM/IM physician has a broader perspective and has a complete understanding of the limitations of each field.”
Residency Satisfaction and Perception of Training
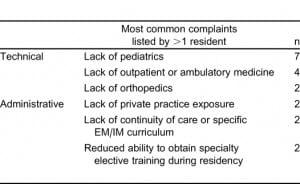
Residents overwhelmingly indicated that they (1) were satisfied with their residency choice (n = 65; 94%), (2) would do a combined program again if given the opportunity (n = 65; 94%), and (3) believed that a combined residency will help advance their career (n = 65; 94%). The open-ended responses for perceived gaps in training and for excesses in training demonstrated that some residents believe that their training could benefit from some changes. The most notable were a call for more pediatrics training (n = 7) and more experience in outpatient/ambulatory medicine (n = 4). The most common responses are categorized and tabulated in Table 3.
DISCUSSION
Our current resident study builds on prior work by Katz and Katz4 and Kessler et al1 by analyzing the future intentions of current EM/IM residents. Three major points are seen in the data: (1) current EM/IM residents favored academic medicine, (2) they perceived it feasible to practice both specialties, and (3) they indicated increased interest in fellowship certification relative to prior graduates of EM/IM residencies.
Academic Medicine
Emergency medicine/internal medicine–trained physicians have always indicated a preference for an academic environment. The study of Katz and Katz4 reported that 43% of the 1995–1998 graduates designated their practice as “academic,” with between 68% and 88% practicing at a teaching hospital. Similar figures were observed for the 1998–2008 graduates who are involved in academic practice, with 69% of graduates devoting at least 10% of their time to an academic/university setting.1 Ninety-six percent of current residents anticipated devoting at least 10% of their future career working in an academic/university practice setting. However, on a per-physician basis, both groups who are, or plan to be, involved in academic practice devoted a median of at least 90% of their time to an academic setting. This suggests that while a greater proportion of current residents anticipate devoting some time to academic medicine, on an individual basis, residents foresee spending a similar amount of time as the graduates currently working at academic institutions. This hypothesis is strengthened by the finding that in subset analysis, interns and PGY-2 residents indicated a greater preference for academic medicine versus their PGY-3 and PGY-4 counterparts.
Combined Practices
In examining this issue, we felt it useful to assess resident preference with respect to (1) board-certification patterns, (2) practice patterns, and (3) residency satisfaction. The study of Katz and Katz4 reported that in the 1995–1998 classes, 87% of residents took EM board examinations, 70% took IM board examinations, and no individuals reported not passing board examinations.3 While not directly reporting the number of residents who only sat for 1 or the other board certification examination, the data permit the inference that there is a sizable population of graduates who obtained certification in only 1 specialty. In the more recent graduate study of Kessler et al,1 the numbers had increased to 99% (EM board examinations) and 96% (IM board examinations). In the current residents group, 100% of resident anticipated gaining board certification in both specialties.
In terms of practice patterns, in the 1995–1998 cohort of graduates, 65% practiced EM exclusively, and only 30% practiced in both fields even though 48% would prefer to practice in both fields.4Similarly, with the 1998–2008 graduates, although 64% stated that it was feasible to practice both specialties, only 37% actually practiced both specialties.1 Interestingly, 97% of the residents planned to devote clinical time practicing both specialties, as compared to the 37% of graduates who actually practiced both specialties (P < 0.00001) (Table 2). Additionally, there was a statistically significant difference (P < 0.0001) in the median time devoted to EM by graduates (100%) as compared with residents (70%). This finding may represent discordance between the enthusiasm of the PGY-1–4 residents and job market realities. An alternative possibility is that the financial and lifestyle lure of EM-only practice may be stronger than the desire to engage in dual practice as a resident approaches training completion and enters clinical practice as an attending physician.
As the issue of perceived feasibility of a future dual practice is intertwined with that of current satisfaction with a combined residency, it is promising to observe that the already high levels of training satisfaction seen in the initial classes have continued with a decidedly upward trend over the years. Of the 1998–2008 graduates, 80% believed their residency choice had advanced their career; for the current residents this figure was 93% (P = 0.019). While there was a generally upward trend in residents indicating that they would repeat their residency if given the chance, there was no statistically significant difference in this response as between the 1998–2008 graduates and the current PGY-1–4 residents.
One unique comment elicited in the free-response query of residency satisfaction was that “[there] needs to be some mechanism to allow fifth year residents to have a full medical license to assume more responsibility [ie,] attending privileges for inpatient services or in the ED setting.” It should be noted that programs have a heterogeneous approach with respect to attending physician privileges. Some allow chief residents to function solely as senior house staff; however, at least 1 program has chiefs “function as ward attending physicians for at least 1 month.”9 A 2006 ABEM survey found that “94% of residents … were ‘satisfied’ to ‘very satisfied’ with their residency” and that “95% of first-year residents … probably or definitely would select EM again.”10 Thus, the high level of satisfaction observed in EM/IM residents is promising but not particularly striking relative to categorical EM counterparts. However, this does suggest that there is not a trade-off in terms of satisfaction for the longer combined route (5 years) relative to the categorical route (3–4 years).
Fellowships
A final observation from the current resident data is that there appears to be an increasing trend toward seeking fellowship training. In the 1995–1998 study, only 1 physician pursued a fellowship of any kind.4 The data from the next decade of graduates reported that 24% of all respondents pursued fellowship training.1 Strikingly, in our study of current residents, 47% anticipated seeking additional postresidency training with a clear preference for critical care (Figure 1). We found the difference between fellowship intention of current residents and fellowship completion of the 1998–2008 graduates to be statistically significant (P = 0.001) (Table 2).
LIMITATIONS
This study was not without limitations, as it required current residents to make a prediction of their future practice patterns. Thus, any comparison of current residents to graduates evaluates actual practice by attending physicians versus anticipated future practice by residents. In 1 survey of 2,638 internal medicine residents, of the 86% PGY-3 residents with specific career plans, 62% had changed their career plans at least once during residency.11 Secondly, this study includes data from 71% current EM/IM residents and makes comparisons with 78% of physicians who graduated from EM/IM training programs during the previous decade. It remains unknown if the results mirror those of the complete EM/IM certified workforce, including physicians who certified in both specialties through either independent residencies or examination (without completing an EM residency). Nonetheless, the data in this study are useful if only to provide a benchmark by which to compare the actual practice patterns of the current PGY-1–4 cohort once they become established attending physicians.
One key finding of this study is that the overwhelming majority of EM/IM residents intend on practicing in an academic setting. However, further examination is required to determine if EM/IM residents are receiving the administrative support (such as dedicated research time, funding, faculty mentorship) to prepare them for careers in academia. In 1 article on academic career development for EM residents, it was noted that fellowships are “increasingly viewed as a key component to a successful academic career and clearly significantly enhances the competitiveness of the applicant seeking an academic post.”12 While we found that more than 90% of EM/IM residents believed combined training will advance their career relative to categorical training, there is not yet any empirical data from a head-to-head comparison to substantiate this ideation.
Given that combined EM/IM residencies have only existed since the early 1990s, it would be valuable to survey dually board-certified attending physicians who went through separate residencies as a point of comparison to those who went through combined training. Such research may help to elicit methods of optimizing the integration of the 2 specialties during training.
With regard to EM/IM graduates seemingly developing a predilection for EM-only practice once they leave residency, a future study could further evaluate the etiology of this phenomenon. The central question could address if it is discordance between resident ideals versus practice realities, or rather lifestyle and financial remuneration, that leads EM/IM residents to engage in EM-only practice. In addition, a follow-up study could be designed to survey the responding residents later in their careers to compare their expectations as residents with how they chose in reality to pursue clinical practice.
Selection bias and response bias were also factors that manifested themselves in the study. The selection bias arose from the need to include the graduating fifth-year resident class in the EM/IM graduate cohort rather than the resident cohort owing to the lag in response time, causing these individuals to be already in clinical practice. Since a fourth-year resident responder is still a resident, they may be counted as a fourth-year resident even with the lag in response time. The authors concede that this issue was not foreseen at the studies inception. Though unintended, it may have had an effect on the study results. The response bias could have affected the study, as the nonresponding residents may have had vastly different opinions and, had they responded, interyear comparisons could have been more effectively done with the boost in power. Also, no adjustments for multiple hypotheses were made during this study owing to concern about decreasing the power of the study.
Finally, given that a significant percentage of EM/IM residents are interested in critical care, it may be helpful to determine how such combined residencies will be affected by the October 2009 agreement between the ABIM and ABEM, allowing EM-trained physicians to become certified in IM critical care.13 It is unknown if under these conditions this sizable minority of EM/IM residents (39%) would choose the shorter categorical EM route rather than longer combined training. As the first group of EM-only critical care trainees will not sit for the certification examination until 2012, the impact of this change on EM/IM residencies remains to be seen.14
CONCLUSION
While 2 previous studies, those of Katz and Katz (2002)4 and Kessler et al (2009)1, investigated the practice habits of EM/IM attending physicians, this is the first and only study of the practice patterns of EM/IM residents during training. We feel that this data set yields several key observations. First, EM/IM residents exhibit a distinct desire to practice academic medicine. Beyond being clinicians, they see themselves acting in roles required of academic physician leaders—administrators (31%) and program directors/associate program directors (37%). Second, residents were optimistic concerning their ability to practice both specialties. All residents anticipated becoming certified in both EM and IM, and 97% anticipated allocating some of their future time to each specialty. Notwithstanding the 5-year combined residency, there was a strong interest in pursuing fellowship training, especially in critical care. Finally, residents were very satisfied with their training, given that 93% indicated being “happy,” believed a combined program had advanced their career, and if given the choice, would repeat a combined EM/IM residency.
Footnotes
Supervising Section Editor: Laleh Gharahbaghian, MD
Submission history: Submitted August 30, 2010; Revision received November 1, 2010; Accepted November 22, 2010
Reprints available through open access at http://escholarship.org/uc/uciem_westjem
DOI: 10.5811/westjem.2010.11.2082
Address for Correspondence: Chad S. Kessler, MD, MHPE
Jesse Brown VA Hospital, Department of Emergency Medicine, 820 S Damen Ave, M/C 111, Chicago, IL 60612
E-mail: Chad.Kessler@va.gov
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Kessler CS, Stallings LA, Gonzalez AA, et al. Combined residency training in emergency medicine and internal medicine: an update on career outcomes and job satisfaction. Acad Emerg Med.2009;;9:894–899. [PubMed]
2. American Medical Association. FREIDA online search. American Medical Association Web site.Available at: https://freida.ama-assn.org/Freida/user/viewProgramSearch.do. Accessed July 1, 2009.
3. National Resident Matching Program. Advance data tables: 2009 main residency match, Table 1. National Resident Matching Program Web site. Available at:http://www.nrmp.org/data/advancedatatables2009.pdf. Accessed June 1, 2010.
4. Katz ED, Katz JT. Career graduates of combined emergency medicine/internal medicine programs.Acad Emerg Med. 2002;;9:1457–1459. [PubMed]
5. Accreditation Council for Graduate Medical Education. Reports of programs by specialty: internal medicine/emergency medicine (non-accredited). Accreditation Council for Graduate Medical Education Web site. Available at: http://www.acgme.org/adspublic/reports/program_specialty.asp. Accessed July 1, 2009.
6. Brotherton SE, Etzel SI. Graduate medical education, 2006–2007. JAMA. 2007;;298:1081–1096.[PubMed]
7. Brotherton SE, Etzel SI. Graduate medical education, 2007–2008. JAMA. 2008;;300:1228–1243.[PubMed]
8. Kennedy TJ, Lingard LA. Making sense of grounded theory in medical education. Med Ed.2006;;20:101–108.
9. University of California Los Angeles. Curriculum: R-5 year. University of California Los Angeles Combined IM/EM Residency Web site. Available at:http://www.uclacombinedimem.org/uclacombinedimem/Curriculum.html. Accessed July 1, 2009.
10. American Board of Emergency Medicine. Satisfaction among emergency medicine residents in 2006. American Board of Emergency Medicine Web site. Available at:http://www.abem.org/PUBLIC/portal/alias__Rainbow/lang__en-US/tabID__3889/DesktopDefault.aspx. Accessed June 1, 2010.
11. West CP, Popkave C, Schultz HJ, et al. Changes in career decisions of internal medicine residents during training. Ann Int Med. 2006;;145:774–779. [PubMed]
12. Stead LG, Sadosty AT, Decker WW. Academic career development for emergency medicine residents: a road map. Acad Emerg Med. 2005;;12:412–416. [PubMed]
13. Wright BJ. Critical care medicine section newsletter – April 2010 – Vol 11, #2. American College of Emergency Physicians Web site. Available at: http://www.acep.org/ACEPmembership.aspx?id=48340&terms=abim. Accessed June 1, 2010.
14. Ault A. ABIM and ABEM agree on critical care certification pathway, May 7, 2010. MD Consult Web site. Available at: http://www.mdconsult.com/das/stat/view/0/mnfp?nid=218494&date=week. Accessed June 1, 2010.


