| Author | Affiliation |
|---|---|
| Alexander R Jack, MD | University of Southern California, Department of Dermatology, Los Angeles, California |
| Allyson A Spence, MD | University of Southern California, Department of Dermatology, Los Angeles, California |
| Benjamin J Nichols, MD | University of Southern California, Department of Emergency Medicine, Los Angeles, California |
| Summer Chong, BA | University of Southern California, Department of Emergency Medicine, Los Angeles, California |
| David T Williams, MD | University of Southern California, Department of Emergency Medicine, Los Angeles, California |
| Stuart P Swadron, MD | University of Southern California, Department of Emergency Medicine, Los Angeles, California |
| David H Peng, MD, MPH | University of Southern California, Department of Dermatology, Los Angeles, California |
ABSTRACT
Introduction:
We established the most common cutaneous diseases that received dermatology consultation in the adult emergency department (ED) and identified differentiating clinical characteristics of dermatoses that required hospital admission.
Methods:
A retrospective chart review of 204 patients presenting to the ED who received dermatology consultations at Los Angeles County/University of Southern California Medical Center, an urban tertiary care teaching hospital.
Results:
Of all patients, 18% were admitted to an inpatient unit primarily for their cutaneous disease, whereas 82% were not. Of nonadmitted patients, the most commonly diagnosed conditions were eczematous dermatitis not otherwise specified (8.9%), scabies (7.2%), contact dermatitis (6.6%), cutaneous drug eruption (6.0%), psoriasis vulgaris (4.2%), and basal cell carcinoma (3.6%). Of patients admitted for their dermatoses, the most highly prevalent conditions were erythema multiforme major/Stevens-Johnson syndrome (22%), pemphigus vulgaris (14%), and severe cutaneous drug eruption (11%). When compared with those of nonadmitted patients, admitted skin conditions were more likely to be generalized (92% vs 72%; P = 0.0104), acute in onset (<1 month duration) (81% vs 51%; P = 0.0005), painful (41% vs 15%; P = 0.0009), blistering (41% vs 7.8%; P < 0.0001), and ulcerated or eroded (46% vs 7.8%; P < 0.0001). They were more likely to involve the mucosa (54% vs 7.2%; P < 0.0001) and less likely to be pruritic (35% vs 58%; P = 0.0169).
Conclusion:
We have described a cohort of patients receiving dermatologic consultation in the ED of a large urban teaching hospital. These data identify high-risk features of more severe skin disease and may be used to refine curricula in both emergency and nonemergency cutaneous disorders for emergency physicians.
INTRODUCTION
Dermatology is often thought of as a nonacute, outpatient-centered specialty. It has been reported, however, that approximately 5% to 8% of all emergency department (ED) visits are due to skin complaints.1 Despite the high prevalence of skin conditions in patients presenting to the ED, few studies have attempted to characterize these dermatoses. In a study performed at a tertiary care center in India, Gupta et al2 reported that 21 of 100 emergency outpatient consultations qualified as “true dermatologic emergencies.” A similar analysis of patients presenting to an ambulatory dermatology clinic in Greece reported that 4.8% of patients had skin diseases that required hospital admission.3 Previous authors also characterized the spectrum of cutaneous disorders encountered in pediatric ED settings.4-6 Yet, to our knowledge, no studies described dermatoses in adults seen in EDs in the United States.
The Model of the Clinical Practice of Emergency Medicine (EM Model), a collaborative of 6 major American EM organizations, defines the practice based on data from ED visits, as well as expert panels.7 The EM Model is used by residency training programs throughout the United States as a guide for core curricula and by the American Board of Emergency Medicine as a basis for standardized examinations. In its most recent update, it defines a range of cutaneous conditions with which emergency physicians (EP) are expected to be familiar. These include conditions that are classified as critical, emergency, and of lesser acuity. Moreover, appropriately detailed EM textbook chapters and published journal articles describe clinical presentations, physical findings, diagnostic tests, and treatment approaches to both common and life-threatening skin diseases that an EP might encounter.1,8–10 Despite these resources, it is often challenging to diagnose skin disease in the ED, especially when limited time is available to evaluate each individual case. The goals of performing the current study were twofold: first, to establish the most common emergency and nonemergency consulted skin conditions evaluated in the ED; second, to identify specific characteristics of dermatoses requiring admission to aid EPs in differentiating true dermatologic emergencies from nonemergency skin conditions.
METHODS
We performed an explicit, retrospective chart review of all dermatology consultations performed in the ED between November 1, 2004, and June 8, 2007, at Los Angeles County/University of Southern California (LAC+USC) Medical Center, an urban tertiary care teaching hospital. All consultations performed in the adult, psychiatric, and jail areas of the ED at LAC+USC were included, whether the patient walked in or was transported by paramedics. The study was approved by the University of Southern California Health Sciences Institutional Review Board.
We reviewed 204 ED consultations, producing 181 definitive diagnoses, as 23 cases were inconclusive. Of note, to be considered definitive, a diagnosis must have been determined clinically without differential diagnosis or confirmed by biopsy or culture. All diagnoses were made by the consultation team comprising a rotating dermatology resident, an attending dermatologist, and, in cases in which biopsies were taken, an attending dermatopathologist. The attending dermatology consultant remained the same throughout the time period, except during rare emergency consultations initiated during holiday and weekend hours. Digital images of clinical findings were provided to the dermatopathologist for review of difficult cases. Further, difficult cases were presented by the consulting resident and discussed at monthly grand rounds for a consensus diagnosis.
We obtained data regarding patient demographics, location, history, physical examination, clinical diagnosis, and reason for consultation from records maintained by the department of dermatology. We acquired information concerning biopsy and culture results, laboratory data, and admission to an inpatient hospital unit from electronic medical records.
Authors A.J., A.S., and B.N. subsequently abstracted a number of variables pertaining to each patient, by using predefined definitions. Skin lesions were recorded as either localized or generalized. A localized lesion was defined as occupying only 1 of the following body-surface areas: head/neck, anterior trunk, posterior trunk, groin/buttock, upper extremities, or lower extremities. We did consider laterality as a criterion. Thus, a lesion that involved both legs below the knees was considered localized because it occupied only the lower extremities. In contrast, we classified a lesion on 1 leg that extended to the buttocks as generalized because it occupied 2 body-surface areas.
Next, we determined the acuity of each patient’s skin condition. We defined an acute condition as cutaneous symptoms beginning less than 1 month before presentation, whereas a chronic condition was defined as symptoms beginning longer than or equal to 1 month before presentation.
Note that no consensus definitions regard the distribution and acuity of skin lesions. We have attributed specific definitions to these terms to maintain consistency when reviewing each case.
In each case, we abstracted several clinical variables with respect to symptoms and physical examination findings. Pruritis or pain associated with the skin lesions was assessed. Additionally, we noted physical examination findings consistent with blistering (vesicles and/or bullae), erosive (erosions and/or ulcerations), or mucosal lesions (any finding, including ulcerating, blistering, and desquamating on any mucosal surface). The number and size of these lesions were not considered. For example, both a patient with a solitary blister and another with generalized blistering would be considered to have blistering in our binary analysis.
Last, we examined electronic medical records to determine whether admission to the hospital occurred immediately after the ED evaluation. For each admitted patient, authors A.J., A.S., and B.N. reviewed the dermatology consultation note and made a consensus determination as to whether their dermatologic diagnosis was the primary reason for admission. We compared clinical variables in admitted and nonadmitted patients and performed statistical analysis by using the two-tailed Fisher Exact test, with P < 0.05 indicating statistical significance.
RESULTS
We reviewed 204 ED consultations conducted during the period between November 1, 2004, and June 8, 2007. During this period, the total ED census was consistently greater than 100,000 patient visits per year. Patient consultations were performed in the following locations: 172 in the adult ED, 24 in the psychiatric ED, and 8 in the jail ED. The average patient age was 43 ± 14 years (range, 18–92 years). The patients were 62% (126 of 204) male and 38% (78 of 204) female.
Of all patients, 18% (37 of 204) were admitted to an inpatient unit primarily for their cutaneous disease, whereas 82% (167 of 204) were not. Of all nonadmitted patients, the most commonly diagnosed dermatologic disorders were eczematous dermatitis not otherwise specified (NOS) at 8.9% (15 of 167), scabies at 7.2% (12 of 167), contact dermatitis at 6.6% (11 of 167), cutaneous drug eruption at 6.0% (10 of 167), psoriasis vulgaris at 4.2% (7 of 167), and basal cell carcinoma at 3.6% (6 of 167) (Table 1). Of those admitted for their dermatologic condition, the most highly prevalent conditions were erythema multiforme major/Stevens-Johnson syndrome (EMM/SJS) at 22% (8 of 37), pemphigus vulgaris 14% (5 of 37), and severe cutaneous drug eruption at 11% (4 of 37) (Table 2). Severe cutaneous drug eruption encompasses blistering drug eruptions not meeting criteria for EMM/SJS, including lithium hypersensitivity syndrome, phenytoin hypersensitivity syndrome, and drug rash with eosinophilia and systemic symptoms.


Generalized and acute dermatoses required admission at a significantly higher rate. Skin conditions that required admission, compared with nonadmitted cases, were generalized in 92% (34 of 37) and 72% (120 of 167), respectively (P = 0.0104) and were acute (duration less than 1 month) in 81% (30 of 37) and 51% (86 of 167), respectively (P = 0.0005) (Table 3).
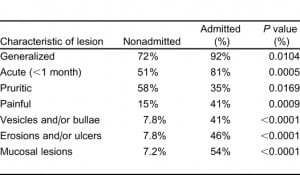
We also observed significant differences in the symptoms associated with the patients’ skin lesions. Nonpruritic, painful lesions required admission at a significantly higher rate. Admitted patients, compared with nonadmitted cases, reported pruritic skin lesions in 35% (13 of 37) and 58% (96 of 165), respectively (P = 0.0169) and painful lesions in 41% (15 of 37) and 15% (24 of 165), respectively (P = 0.0009). We excluded 2 patients from the nonadmitted group because they did not report their symptoms.
We observed the largest differences between the admitted and nonadmitted groups of patients in the physical examination findings of specific skin lesions. Admitted patients, compared with nonadmitted cases, had vesicular or bullous skin lesions in 41% (15 of 37) and 7.8% (13 of 167), respectively (P < 0.0001), eroded or ulcerated skin lesions in 46% (17 of 37), and 7.8% (13 of 167), respectively (P < 0.0001), and had mucosal lesions in 54% (20 of 37) and 7.2% (12 of 167), respectively (P < 0.0001).
Note that we included all consults conducted during the studied time period in these analyses, whether or not they resulted in a definitive diagnosis. We thought that it was important to include the nondiagnostic consults because the same historic and physical characteristics are likely to correlate with admission as in consults resulting in a definitive diagnosis.
DISCUSSION
In accordance with previous reports, a large majority (82%) of ED dermatoses for whom consultation was requested were nonemergency.2,3 Several factors may have contributed to this finding. First, skin disease is common in the United States, with more than 35 million visits to office-based dermatologists in 2000.11 Hanifin and Reed12 reported that 31.6 million Americans complain of symptoms suggestive of eczema. A recent population-based study estimated the prevalence of psoriasis in the United States to be 2.5% for Caucasians and 1.3% for African Americans.14 The American Cancer Society estimates that well over 1 million cases of basal cell and squamous cell carcinoma will occur in the United States in 2008.14 These common conditions were all prevalent in this study. Second, despite the high prevalence of dermatoses in the American population, it is difficult to obtain a timely dermatology appointment. The mean wait time for a new-patient visit to a dermatologist is approximately 33 days.15 At public safety-net hospitals such as ours, wait times are significantly longer because of the higher proportion of patients with limited or no health insurance. Third, as confirmed in a recent Centers for Disease Control and Prevention report, an increased reliance has developed on the ED for routine healthcare, especially by Medicare, Medicaid, and uninsured patients.16 The combination of these 3 factors likely resulted in the high prevalence of nonemergency skin conditions observed in our study.
Because nonemergency skin conditions are commonly found in patients presenting to the ED, it may be helpful for EPs to be familiar with those that are most common: eczematous dermatitis NOS, scabies, contact dermatitis, cutaneous drug eruption, psoriasis vulgaris, and basal cell carcinoma. All of these conditions are itemized in the EM Model of Practice as lower-acuity conditions, with the exception of cutaneous drug eruption, which does not appear.
Of the 18% of the patients receiving dermatologic consultation that were thought to require admission, the most prevalent dermatoses were EMM/SJS, pemphigus vulgaris, and severe cutaneous drug eruptions. Whereas the first 2 are listed as critical and emergency cutaneous conditions on the EM Model, cutaneous drug eruptions do not appear in the cutaneous disorders section. Drug allergies are listed as potentially emergency conditions under the hypersensitivity category in the immune system disorders section. Additionally, the duration, distribution, associated symptoms, and specific skin lesions associated with the presentation may be helpful to determine the need for admission. Lesions that are generalized, acute, painful, and nonpruritic are more worrisome. Moreover, the presence of blistering, erosive, or mucosal lesions is significantly more likely to be associated with an emergency diagnosis.
LIMITATIONS
This study analyzes cases in which a dermatology consultation was initiated. It is important to note that thousands of patients with dermatologic complaints were managed directly by EPs, triaged appropriately to the outpatient setting, or referred to other inpatient services without being evaluated by dermatology (for example, a patient with cellulitis referred to the internal medicine service for admission). As such, it is equally important to understand what circumstances prompted a dermatologic consultation. Common reasons noted for the initiation of dermatology consultation for nonadmitted patients included those with prior visits to the ED who were not responsive to prescribed treatments, those with acute onset of cutaneous findings, those deemed poorly reliable to seek outpatient follow-up, and those who recently started a medication known commonly to cause bullous drug eruptions. The most common reason noted for initiating a consultation in admitted patients was for suspicion of an autoimmune or drug-induced bullous disease.
This creates referral bias, and thus our findings do not represent all cutaneous disease treated in the ED, but merely cutaneous disease that the EPs thought would benefit from a dermatologic consultation. Unfortunately, we do not have data regarding the prevalence of conditions with cutaneous manifestations that were not seen by consulting dermatologists.
As a result of the larger percentage of uninsured and indigent patients seen at our institution, a higher incidence of nonemergency or chronic skin diseases may have been observed. Furthermore, because our institution is a major referral center and teaching hospital, we are fortunate to have dermatologic consultation service available to the ED. The referral and practice patterns at many community EDs likely differ significantly; many do not have ready access to dermatologic consultation, and the number and nature of consultations performed may vary widely in these settings.
Another limitation involves geography. Our data represent only 1 urban center on the southwest coast of the United States, where conditions such as Rocky Mountain Spotted Fever or Lyme disease are much less common. Last, this study did not include consultations performed in the pediatric ED. Our findings cannot be generalized to the pediatric population.
CONCLUSION
This retrospective analysis aims to provide insight into the types of cases being evaluated by consulting dermatologists in a large, urban, adult ED located in the Southwestern United States. Limitations of the study preclude commentary on all dermatologic disease seen and managed by EPs. In addition, we provide an analysis of clinical characteristics that may help in determining the severity of disease in this population. An awareness of these characteristics may assist the EM community in evaluating patients who present to the ED with cutaneous disease.
Footnotes
Supervising Section Editor: Christopher Kang, MD
Submission history: Submitted July 29, 2009; Revision received February 3, 2010; Accepted April 2, 2010
Reprints available through open access at http://escholarship.org/uc/uciem_westjem
DOI: 10.5811/westjem.2010.4.1653
Address for Correspondence: David H. Peng, MD, MPH
Stanford University, Department of Dermatology, 450 Broadway St, Redwood City, CA 94063
E-mail: pengd@stanford.edu
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Trott AT. Hamilton GC, Sanders A, Strange GS, et al, eds. Emergency Medicine: An Approach to Clinical Problem-Solving. 2nd ed. Philadelphia, PA: Saunders;; 2003. Rash; pp. 185–206.
2. Gupta S, Sandhu K, Kumar B. Evaluation of emergency dermatological consultations in a tertiary care centre in North India. J Eur Acad Dermatol Venereol. 2003;;17:303–305. [PubMed]
3. Symvoulakis EK, Krasagakis K, Komninos ID, et al. Primary care and pattern of skin diseases in a Mediterranean island. BMC Fam Pract. 2006;;7:6. [PMC free article] [PubMed]
4. Shivaram V, Christoph RA, Hayden GF. Skin disorders encountered in a pediatric emergency department. Pediatr Emerg Care. 1993;;9:202–204. [PubMed]
5. Auvin S, Imiela A, Catteau B, et al. Paediatric skin disorders encountered in an emergency hospital facility: a prospective study. Acta Derm Venereol. 2004;;84:451–454. [PubMed]
6. Dolan OM, Bingham EA, Glasgow JFT, et al. An audit of dermatology in a paediatric accident and emergency department. J Accid Emerg Med. 1994;;11:158–161. [PMC free article] [PubMed]
7. Thomas HA, Beeson MS, Binder LS, et al. The 2005 Model of the Clinical Practice of Emergency Medicine: the 2007 update. Ann Emerg Med. 2008;;52:e1–17. [PubMed]
8. Cydulka RA, Hancock M. Dermatologic presentations. In: Marx JA, editor. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 6th ed. Philadelphia, PA: Mosby; 2006. pp. 1838–1867.
9. Freiman A, Borsuk D, Sasseville D. Dermatologic emergencies. CMAJ. 2005;;173:1317–1319.[PMC free article] [PubMed]
10. Levine N. Emergency room dermatology. Dermatol Nurs. 1999;;11:331–336. 341–346. [PubMed]
11. Stern RS. Dermatologists and office-based care of dermatologic disease in the 21st century. J Invest Dermatol Symp Proc. 2004;;9:126–130.
12. Hanifin JM, Reed ML. A population-based survey of eczema prevalence in the United States.Dermatitis. 2007;;18:82–91. [PubMed]
13. Gefland JM, Stern RS, Nijsten T, et al. The prevalence of psoriasis in African Americans: results from a population-based study. J Am Acad Dermatol. 2005;52:23. [PubMed]
14. American Cancer Society. Cancer facts and figures 2008. American Cancer Society Web site.Available at: www.cancer.org. Accessed November 2008.
15. Kimball AB, Resneck JS. The US dermatology workforce: a specialty remains in shortage. J Am Acad Dermatol. 2008;59:741–745. [PubMed]
16. Schappert SM, Rechtsteiner EA. Ambulatory medical care utilization estimates for 2006.National Health Statistics Reports; no 8. Hyattsville, MD: National Center for Health Statistics; 2008.


