| Author | Affiliation |
|---|---|
| Rene M. Kukkamalla, MD | Maricopa Medical Center, Department of Emergency Medicine, Phoenix, Arizona |
| Patricia Bayless, MD | Maricopa Medical Center, Department of Emergency Medicine, Phoenix, Arizona; University of Arizona College of Medicine-Phoenix, Department of Emergency Medicine, Phoenix, Arizona |
CASE PRESENTATION
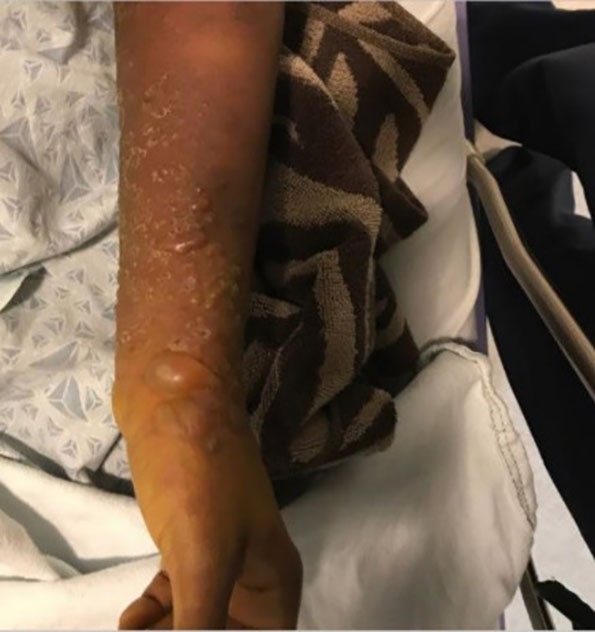
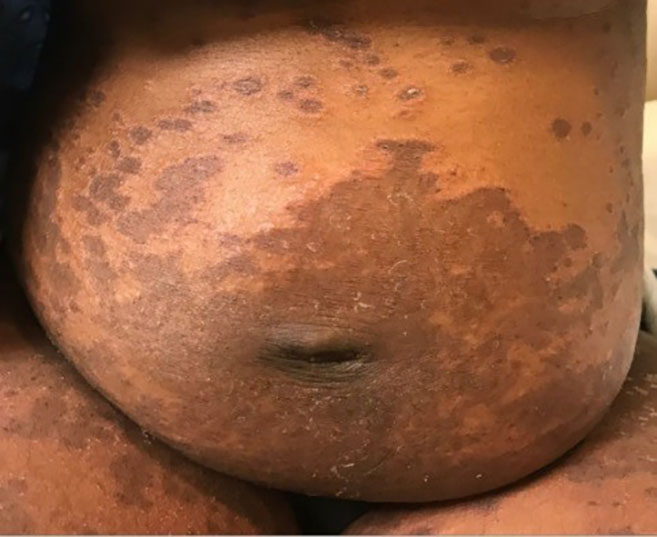
A 32-year-old female gravida 3 para 2 presented to the emergency department (ED) with two weeks of hyperpigmented macular and blistering rash involving bilateral upper and lower extremities (Image 1) and trunk (Image 2). The patient was approximately 16 weeks pregnant at time of presentation. The rash was significantly pruritic. She denied constitutional symptoms or mucous membrane involvement. The patient was seen by obstetrics/gynecology consult who deemed her rash consistent with pemphigoid gestationis (PG). She was started on high-dose steroid therapy with improvement in the rash. ELISA (an enzyme-linked immunosorbent assay that measures autoantibody reactions to the bullous pemphigoid antigen [BP180] with 96% sensitivity and specificity for PG) showed our patient’s values elevated at 30.59 units (reference range less than 9.0 units).1 By the 35th week of pregnancy, her rash had resolved while on a stringent steroid regimen. She developed gestational diabetes that is being managed by her prenatal care provider.
DISCUSSION
PG is considered a rare disease with estimated incidence approximately 1 in 50,000 pregnancies.2 The disease shows a worldwide distribution and no differences in ethnicity. General population studies on the epidemiology of PG are small.4 The rash is characterized by pruritic papular and vesiculobullous eruptions that typically involve the abdomen and extremities. The face is classically spared.2 It is thought to be an autoimmune phenomenon caused by immunoglobulin G antibody to a 180-kilodaltons antigen in the basement membrane.1 Onset of the rash is typically in the second or third trimester and can occur immediately post-partum.3
It is important to distinguish this disease from other pregnancy-associated dermatoses because of the high rate of recurrence with more severe symptoms in later pregnancies.1,4 Typically fetuses are unaffected; however, in less than 5% of cases they can contract transient skin lesions. While fetal outcome is generally good, there is increased risk for intrauterine growth restriction as well as preterm labor.2,4 Diagnosis is made either clinically, by skin biopsy with direct immunofluorescence (showing linear deposits of complement along the basement membrane), or elevated BP180 antibody levels. Treatment includes topical steroids. For more severe cases systemic steroids are appropriate.3, 4
CPC-EM Capsule
What do we already know about this clinical entity?
Pemphigoid gestationis (PG) is well described but rarely encountered.
What is the major impact of the image(s)?
The images demonstrate a true “pemphigoid” rash.
How might this improve emergency medicine practice?
Recognition of PG impacts referral and management of the current and future pregnancies.
Footnotes
Section Editor: Scott Goldstein, DO
Full text available through open access at http://escholarship.org/uc/uciem_cpcem
Documented patient informed consent and/or Institutional Review Board approval has been obtained and filed for publication of this case report.
Address for Correspondence: Rene M. Kukkamalla, MD, Maricopa Medical Center, Department of Emergency Medicine, 2601 East Roosevelt Street, Phoenix, AZ 85008. Email: meghanakukks@gmail.com. 3:79 – 80
Submission history: Revision received June 7, 2018; Submitted October 28, 2018; Accepted November 7, 2018
Conflicts of Interest: By the CPC-EM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Powell AM, Sakuma-Oyama Y, Oyama N, et al. Usefulness of BP180 NC16a enzyme-linked immunosorbent assay in the serodiagnosis of pemphigoid gestationis and in differentiating between pemphigoid gestationis and pruritic urticarial papules and plaques of pregnancy. Arch Dermatol. 2005;141(6):705-10.
2. Dulay AT. Pemphigoid Gestationis. Merck Manual Professional Version. 2017. Available at: https://www.merckmanuals.com/professional/gynecology-and-obstetrics/abnormalities-of-pregnancy/pemphigoid-gestationis. Accessed May 25, 2018.
3. Flangini Cobo M, Giuli Santi C, Wakisaka Maruta C, et al. Pemphigoid gestationis: clinical and laboratory evaluation. Clinics (Sao Paulo). 2009;64(11):1043-7.
4. Saverall C, Sand FL, Thomsen SF. Pemphigoid gestationis: current perspectives. Clin Cosmet Investig Dermatol. 2017;10:441-9.


