| Author | Affiliation |
|---|---|
| Phyllis A. Vallee, MD | Henry Ford Hospital, Department of Emergency Medicine, Detroit, MI |
ABSTRACT
Chilaiditi syndrome, symptomatic interposition of bowel beneath the right hemidiaphragm, is uncommon and usually managed without surgery. Morgagni hernia is an uncommon diaphragmatic hernia that generally requires surgery. In this case a patient with a longstanding diagnosis of bowel interposition (Chilaiditi sign) presented with presumed Chilaiditi syndrome. Abdominal computed tomography was performed and revealed no bowel interposition; instead, a Morgagni hernia was found and surgically repaired. Review of the literature did not reveal similar misdiagnosis or recommendations for advanced imaging in patients with Chilaiditi sign or syndrome to confirm the diagnosis or rule out other potential diagnoses.
INTRODUCTION
Presence of intestinal loops cephalad to the liver is an uncommon radiographic finding. If this bowel is located above the diaphragm, an intrathoracic hernia is present. If located beneath the diaphragm, bowel interposition or Chilaiditi sign is present. When symptoms develop in these conditions, they may have similar presentations; however, management is often very different. Plain radiographs may not accurately distinguish between these two entities. Consideration should be given to evaluation with a computed tomography (CT) scan to establish the correct diagnosis.
CASE REPORT
A 44-year-old female presented to the emergency department (ED) with abdominal pain that began abruptly six hours prior to presentation. The pain, which was located in the epigastric and periumbilical area without radiation, was initially mild but progressed in severity. The quality was both aching and stabbing. Anorexia was noted but no vomiting or diarrhea. The patient’s past medical history included six vaginal deliveries and suction curettage for a second trimester incomplete abortion.
In the ED, the patient was uncomfortable and tearful. Vitals signs were blood pressure 165/93 mm Hg, pulse 112 beats/min, respiratory rate 20 breaths per minute, oral temperature 37.2°C. On examination she was anicteric, lungs were clear to auscultation, and cardiac exam demonstrated tachycardia. Abdominal exam revealed diminished bowel sounds, tenderness with guarding in the epigastric and periumbilical regions and no rebound. Stool was guaiac negative.
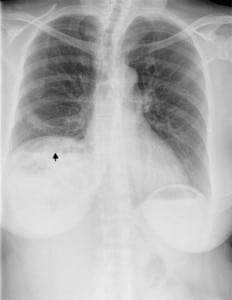
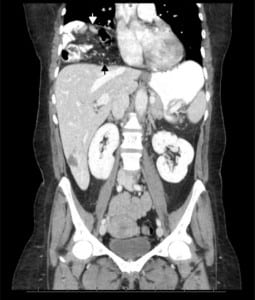
Shortly after examination, the patient developed nonbilious vomiting. She received intravenous fluid, hydromorphone for pain and ondansetron for vomiting. Initial diagnostic evaluation showed normal complete blood count, serum electrolytes, blood urea nitrogen, creatinine, lipase, lactic acid, liver function tests and urinalysis. Pregnancy test was negative. Acute abdominal series (upright chest plus upright and supine abdomen radiographs) reported no free air, bowel obstruction or calcification, but did note a large amount of gas-filled bowel loops positioned at the right subdiaphragmatic region with an elevated right diaphragm (Figure 1) and mild small bowel dilatation in the central abdomen. It was specifically noted that this “interposition pattern” was observed on an abdominal series completed 20 years prior. This earlier report stated: “Note is made of interposition of the hepatic flexure between the anterior abdominal wall and liver, which is a normal anatomic variant.” Based on results of the diagnostic studies, a presumptive diagnosis of Chilaiditi syndrome was made. Because the patient continued to be symptomatic, an abdominal CT with oral and intravenous contrast was ordered to help define the exact etiology of her pain. The scan did not demonstrate bowel interposition; instead it revealed a diaphragmatic hernia on the right containing multiple bowel loops with no evidence of obstruction (Figure 2). The patient was admitted to the surgical service with a diagnosis Morgagni hernia and was subsequently taken to the operating room for repair.
DISCUSSION
This case illustrates two relatively rare clinical diagnoses. In 1910, a small case series presented by Demetrius Chilaiditi described the incidental radiographic finding of bowel interposed between the liver and right hemidiaphragm. This finding is now known as Chilaiditi sign. It is estimated to occur in 0.025–0.28% of the population.1 It is more common in males.2,3
Development of hepatodiaphragmatic interposition has been attributed to multiple factors. Predisposing functional disorders include constipation, diaphragmatic paralysis, increased gastrointestinal motility and aerophagia.1,2,4 Anatomic factors include malfixation or malposition of bowel, redundant or elongated bowel, laxity of hepatic suspensory ligaments, reduced liver volume (i.e. cirrhosis), disorders resulting in increased intraabdominal pressure (i.e. pregnancy), and disorders associated with enlargement of the lower thoracic cavity (i.e. chronic obstructive pulmonary disorder).1,2,4
Asymptomatic patients with Chilaiditi sign require no intervention other than to initially differentiate the radiographic finding from pneumoperitoneum. When patients with Chilaiditi sign present with symptoms the correct terminology is Chilaiditi syndrome.1,2,3 Symptoms range from mild gastrointestinal complaints such as nausea, anorexia and constipation to guarding, rigidity and rebound. The differential diagnosis includes entities that must be distinguished from interposed bowel such as subphrenic abscess, pneumoperitoneum, retroperitoneal masses and posterior liver lesions.1,3,4 The differential also includes disorders related to the specific section of interposed bowel: internal hernias, bowel obstruction, volvulus, intussusception, ischemic bowel or inflammatory conditions, such as appendicitis and diverticulitis.
Treatment of Chilaiditi syndrome is usually non-operative, consisting of hydration, bowel decompression, laxatives, enemas, fiber supplementation and observation.2 However, if pain persists, obstruction fails to resolve, there is evidence of bowel ischemia or development of an acute abdomen, operative intervention may be indicated.4
Morgagni hernia is an internal herniation of abdominal contents into the thoracic cavity through a congenital defect in the anterior diaphragm, although at least one recent publication raises the possibility that acquired defects may be the actual etiology.5 Morgagni hernias are rare, accounting for 2–6% of all diaphragmatic hernias.5,6 Ninety percent are right sided with the rest left sided or bilateral.7 In children, they are more common in males while in adults, the majority occur in women.5,7,8 Most Morgagni hernias are believed to be asymptomatic.6,8 When symptoms occur they include pulmonary complaints (cough, dyspnea, chest pain/pressure) or gastrointestinal complaints (abdominal pain/pressure, indigestion, dysphagia and bleeding).7 Bowel obstruction with or without ischemia may also develop.
Plain radiography of Morgagni hernias may demonstrate a spectrum of findings from obvious intrathoracic bowel loops to ill-defined anterior intrathoracic or mediastinal soft tissue masses. When the radiographic findings are not diagnostic, the differential diagnosis includes multiple intrathoracic and mediastinal neoplasms, pericardial cysts, pneumonia, empyema, lung sequestration, hydatid cysts, diaphragmatic eventration and other diaphragmatic hernias; however, mention of bowel interposition is noticeably absent.6,7 Once diagnosed, the definitive treatment of a Morgagni hernia is surgical repair.
Most of the current literature on Chilaiditi sign/syndrome and diaphragmatic hernias involve case reports and reviews and nearly all fail to include the other in the differential diagnosis. A Medline search revealed only two articles that discussed both entities: a case report of Chilaiditi sign initially diagnosed as a traumatic diaphragmatic hernia and a case report of a patient with Chilaiditi syndrome who had both bowel interposition and a right-sided Bochdaleck hernia.9,10
Emergency physicians evaluate scores of patients with undifferentiated chest pain and abdominal pain. Plain radiographic images may provide a probable diagnosis, but they may be inaccurate. In a patient with appropriate symptoms and a radiographic report of Chilaiditi sign it may be prudent to pursue further diagnostic evaluation with a CT scan to rule out the alternate diagnosis of a Morgagni or other diaphragmatic hernia. Furthermore, nonemergent CT scanning may be indicated in patients with a first time finding of Chilaiditi sign to definitively confirm the diagnosis.
Footnotes
Supervising Section Editor: Sean Henderson, MD
Submission history: Submitted October 5 2010; Revision received October 21 2010; Accepted October 27 2010
Reprints available through open access at http://scholarship.org/uc/uciem_westjem
Address for Correspondence: Phyllis A. Vallee, M.D, Henry Ford Hospital Department of Emergency Medicine, CFP-261,2799 West Grand Boulevard, Detroit, MI 48202
E-Mail: pvallee1@hfhs.org
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Alva S, Shetty-Alva N, Longo WE. Image of the month: Chilaiditi sign or syndrome. Arch Surg.2008;143:93–4. [PubMed]
2. Fisher AA, Davis MW. An elderly man with chest pain, shortness of breath, and constipation.Postgrad Med J. 2003;79:180–4. [PMC free article] [PubMed]
3. Saber AA, Boros MJ. Chilaiditi’s syndrome: what should every surgeon know? Am Surg.2005;71:261–3. [PubMed]
4. Risaliti A, Anna DD, Terrosu G, et al. Chilaiditi’s syndrome as a surgical and nonsurgical problem.Surg Gyn Ob. 1993;176:55–8.
5. McBride CA, Beasley SW. Morgagni’s hernia: believing is seeing. Aust N Z J Surg. 2008;78:739–44.
6. Loong TPF, Kocher HM. Clinical presentation and operative repair of hernia of Morgagni. Postgrad Med J. 2005;81:41–4. [PMC free article] [PubMed]
7. Horton JD, Hofmann LJ, Hetz SP. Presentation and management of Morgagni hernias in adults: a review of 298 cases. Surg Endosc. 2008;22:1413–20. [PubMed]
8. Schneidau A, Baron HJ, Rosin RD. Morgagni revisited: a case of intermittent chest pain. Brit J Radiol. 1982;55:238–40. [PubMed]
9. Kamiyoshihara M, Ibe T, Takeyoshi I. Chilaiditi’s sign mimicking a traumatic diaphragmatic hernia. Ann Thorac Surg. 2009;87:959–61. [PubMed]
10. Hivert B, Der Sahakian G, Claessens YE, et al. Chilaiditi’s sign or syndrome in the emergency department. Emerg Med J. 2008;25:87. [PubMed]


