| Author | Affiliation |
|---|---|
| Michael E. Nelson, MD, MS | John H. Stroger Hospital of Cook County, Chicago, Illinois
Toxikon Consortium, Illinois Poison Control Center, Chicago, Illinois |
| Isam Nasr, MD | John H. Stroger Hospital of Cook County, Chicago, Illinois
Westlake Hospital, Melrose Park, Illinois |
Introduction
Case reports
Discussion
Conclusion
INTRODUCTION
Many cases of hydrocarbon toxicity occur annually due to oral or inhalational exposure. Rarely are hydrocarbons injected subcutaneously or intravenously. These parenteral routes of exposure, however, can have a wide range of consequences ranging from mild skin irritation to tissue necrosis, pulmonary injury, neurologic consequences, cardiovascular collapse, and death. WD-40™ is a commonly used household hydrocarbon containing aliphatic hydrocarbon (45 – 50%), low vapor pressure aliphatic hydrocarbon (12 – 18%), petroleum-based oil (<25%), carbon dioxide (2–3%), surfactant (<2%), and other “non-hazardous ingredients” (<10%).1 We present a pair of cases and associated visual images of complications from intravenous (IV) and subcutaneous (SC) WD-40 injection. Additionally, we will discuss complications from parenteral hydrocarbon exposures, in particular pulmonary injury and local tissue reactions as observed in our cases.
CASE REPORTS
Case 1
A 23-year-old male injected himself with WD-40™ in a suicide attempt approximately 12 hours prior to presentation in the emergency department (ED). The patient stated he was feeling more depressed due to social situations of being unemployed and living out of his car with his fiancée. In a suicide attempt with his fiancée (Case 2), he injected WD-40™ intravenously via the right basilic vein. The couple sprayed the WD-40™ into a cup and used an insulin syringe to aspirate the hydrocarbon to inject 1 mL at a time. He self-injected nearly 15 times (15 mL) throughout the night until roughly 12 hours later he began to feel “heavy in the lungs” and then called Emergency Medical Services (EMS). He complained of nausea with 4 episodes of emesis, difficulty breathing, headache and diffuse joint pain. Past medical history is significant for IV heroin use and he does not take any prescription medications. Vital signs on arrival included a temperature of 101.7 °F, blood pressure of 120/57 mmHg, pulse of 116 beats per minute (bpm), respiratory rate of 20 breaths per minute, and oxygen saturation (SpO2) of 93% on room air. Physical exam noted rales in the right lung base, but no respiratory distress or retractions, and bilateral antecubital skin injection sites with track marks but no overlying skin irritation. Laboratory evaluation revealed a white blood cell count (WBC) of 11.2 k/mm,3 hemoglobin 14 g/dL, serum creatinine 1.39 mg/dL, and arterial blood gas (ABG) on room air with pH 7.45, pCO2 32.8 mmHg, pO2 51 mmHg, HCO3 23 mmol/L, and oxygen saturation of 88%. Urine qualitative drug screen was positive only for opiates. Additionally, serum ethanol, acetaminophen, and aspirin concentrations were non-detectable. Chest radiograph (CXR) in the ED demonstrated pulmonary edema with right lower lobe infiltrate (Figure 1). Radiograph of the patient’s right elbow over the injection site did not demonstrate foreign body or subcutaneous emphysema. The patient was treated with supplemental oxygenation via non-rebreather mask, 40 mg of IV furosemide, 1 gm of ceftriaxone, 800 mg of ibuprofen, and 1 gm of acetaminophen. His maximum temperature was 103.3 °F in the ED. With supplemental oxygenation, the patient’s SpO2 improved to 99%. The patient was admitted to the intensive care unit (ICU). By hospital day 2, his pulmonary edema and chemical pneumonitis improved with supplemental oxygenation and methylprednisolone 125 mg IV once daily. He did not require additional doses of diuretics.
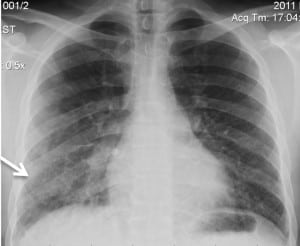
Chest radiograph of Patient 1 on presentation shows pulmonary edema and right lower lobe infiltrate (arrow).
He developed cellulitis of the right upper extremity near the injection site in the right antecubital fossa on the second hospital day and was started on 1 gm of vancomycin and 3.375 gm piperacillin/tazobactam. Repeat laboratory studies on hospital day 2 demonstrated increasing leukocytosis with WBC 16.4 k/mm3 with 5% band neutrophils and 76% segmented neutrophils. The cellulitis progressed into an abscess and on hospital day 7, the patient was taken to the operating room for incision and drainage. The procedure demonstrated liquefied necrotic subcutaneous tissue, which was debrided and excised, and the wound was packed with iodoform gauze. Culture of the abscess revealed no growth of any organisms. After incision and drainage, the patient improved clinically with reduction in pain and redness in his right upper extremity. CXR findings resolved (Figure 2) by hospital day 3, and he was discharged after 9 days to inpatient psychiatric care.
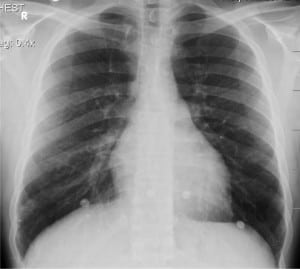
Repeat chest radiograph shows resolution of infiltrates and edema of Patient 1.
Case 2
A 29-year-old female injected herself with WD-40™ in a suicide attempt with her fiancé (Case 1) approximately 12 hours prior to seeking medical attention. She injected herself in the dorsal aspect of her right hand and the palmar aspect of her right wrist. As this patient had “hard-to-find veins,” she did not inject herself as frequently as her fiancé and subsequently injected SC despite attempting the IV route. She complained of pain at the injection site that slowly progressed over the 12 hours prior to calling EMS. She denied shortness of breath, nausea, vomiting, or systemic symptoms. Her history is only significant for IV heroin use. Vital signs included a blood pressure of 104/66 mmHg, pulse of 94 bpm, temperature of 97.5 °F, and SpO2 of 98% on room air. Physical exam demonstrated significant swelling and erythema of her right hand, wrist and forearm with lymphangitic streaking to the proximal forearm and extreme tenderness to palpation. Radial and ulnar pulses were obtained via Doppler probe. Laboratory evaluation revealed a WBC of 19.2 k/mm3 with 34% band neutrophils. Urine qualitative drug screen was positive only for opiates. Additionally, serum ethanol, acetaminophen, and aspirin concentrations were non-detectable. Radiograph of the right hand and wrist demonstrated subcutaneous emphysema (Figure 3). She was given 600 mg of clindamycin and 1 gm of vancomycin and admitted to the ICU. Infectious Disease was consulted for further antibiotic recommendations and 3.375 gm of piperacillin/tazobactam was added for extended coverage. She had severe persistent pain in her right hand and wrist and the surgical service determined the patient had developed compartment syndrome. She was taken to the operating room on hospital day 3. Fasciotomy of the extensor, flexor, and interosseous compartments of the right upper extremity were performed revealing a moderate amount of tissue and fat necrosis (Figure 4). Necrotic tissue was debrided and irrigated without evidence of abscess or progressive infection and the incisions were closed. Wound cultures were negative for growth of any organisms. The patient’s pain improved, and after hospital day 11, she was transferred to an acute inpatient psychiatry unit.
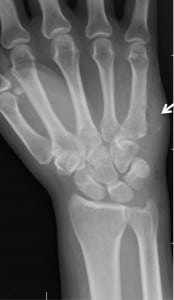
Right upper extremity of Patient 2. Wrist radiograph demonstrates subcutaneous emphysema (arrow) extending from injection site and hand down to forearm.
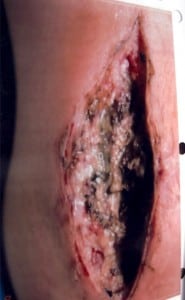
Fasciotomy of forearm shows diffuse fat necrosis of Patient 2.
DISCUSSION
Hydrocarbons naturally occur in crude oil and are a primary energy source in fuel combustion. Household products containing hydrocarbons are typically used as lubricants, automotive chemicals, and degreasers. WD-40™ is one common household hydrocarbon typically used as a lubricant. According to the 2011 National Poison Data System (NPDS), single substance hydrocarbon exposures accounted for 37,194 (1.78%) of total exposures with 17 (3.48%) deaths and 11,512 (1.04%) of pediatric (< 5 years old) exposures with a total of 4 (11.76%) pediatric deaths.2 Reviewing those deaths demonstrates that all had inhalation or ingestion as route of exposure.2 Of the 37,194 single substance hydrocarbon exposures, lubricants (such as WD-40™) accounted for 3933 exposures with 79 moderate effects and 3 major effects but no deaths.2 Unfortunately, it is difficult to discern what those moderate and major effects are and just how many of those were parenteral exposures.
Due to the volatility and surface tension of a particular hydrocarbon, oral ingestion may have a high risk of aspiration. Highly volatile hydrocarbons with low viscosity carry a higher aspiration risk. Fortunately, most unintentional oral exposures do not result in significant complications.3 Suicidal patients, however, pose a different risk given their intent and that they often use greater amounts of a particular substance in comparison to accidental exposures. Additionally, suicidal patients will attempt different routes of exposure than commonly encountered for an accidental exposure. Most reports of parenteral hydrocarbon exposure occur in patients with intent to harm or accidental occupational injury.
Clinical effects vary greatly depending on route of exposure. Oral hydrocarbon exposure classically causes toxicity to the pulmonary system, mostly from inhalation and aspiration. Symptoms include respiratory distress, pleurisy, hypoxemia, and a potentially hemorrhagic pneumonitis.4–6 Inhalational hydrocarbon exposure has caused cardiovascular collapse with sudden sniffing death syndrome. 7 Central nervous system effects vary greatly and range from mild euphoria to lethargy and seizures.4,8 Hematologic effects may include intravascular hemolysis and significant leukocytosis.5,9,10,11 Intravenous hydrocarbon exposure has caused respiratory failure with chemical pneumonitis and interstitial pulmonary edema with hypoxia.15 It has also been associated with multi-organ dysfunction and with renal and hepatic involvement.12 Local injection site reactions occur and can result in cellulitis, fat necrosis, and abscess formation, which tend to be sterile.4,13,14 Subcutaneous injection has resulted in compartment syndrome and the need for fasciotomy.10,13 In particular, WD-40™ subcutaneous exposure is a rare occurrence, yet small volume injection (0.5 mL) has been associated with significant local skin reaction with cellulitis and profound leukocytosis as observed in our cases.15
These 2 cases highlight the possible major effects physicians will encounter from intravenous or subcutaneous hydrocarbon exposure. Although parenteral hydrocarbon exposures are described in the literature, images associated with the outcomes from these parenteral methods rarely accompany reports. The practicing physician should be aware of the potential complications associated with parenteral hydrocarbon exposure. Although no specific antidote or therapy exists for hydrocarbon toxicity, symptom-based goal-directed supportive care remains the mainstay of therapy.
CONCLUSION
Intravenous and subcutaneous hydrocarbon exposures are rare occurrences. We report a pair of cases with these rarely encountered avenues of exposure. The first case involved intravenous WD-40™ exposure in a man that developed pulmonary edema and subsequent cellulitis with sterile abscess at the injection site. The second case was a female with subcutaneous WD-40™ injection that resulted in compartment syndrome requiring a fasciotomy. Both patients fully recovered; however, these cases provide insight and corresponding images for the potential deleterious outcomes associated with these two unique routes of hydrocarbon exposure.
Footnotes
Address for Correspondence: Michael E. Nelson, MD, MS, Department of Emergency Medicine, John H. Stroger Jr. Hospital of Cook County, Toxikon Consortium, Illinois Poison Control Center, 1900 W. Polk St.,10th Floor, Chicago, IL 60612. Email: menelson4@gmail.com. 9 / 2013; 14:431 – 434
Submission history: Revision received December 16, 2012; Submitted March 12, 2013; Accepted March 19, 2013
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1 . WD-40™Material Safety Data Sheet. Revision March 2010. WD-40 Company Website. Available at:http://wd40company.com/partners/msds/usa/
2 Bronstein AC, Spyker DA, Cantilena LR 2011 Annual Report of the American Association of Poison Control Centers’ National Poison Data System (NPDS): 29 Annual Report. Clin Toxicology. 2012; 50:911-1164
3 Anas N, Namasonthi V, Ginsburg C Criteria for Hospitalizing Children Who Have Ingested Products Containing Hydrocarbons. JAMA. 1981; 246:840-843
4 Shusterman EM, Williams SR, Childers BJ Soft Tissue Injection of Hydrocarbons: A Case Report and Review of the Literature. J Emerg Med. 1999; 17:63-65
5 Fink K, Kuehnemund A, Schwab T Suicide attempt by Intravenous Injection of Gasoline: A Case Report. J Emerg Med. 2010; 39:618-622
6 Guerguerian AM, Lacroix J Pulmonary injury after intravenous hydrocarbon injection. Paediatr Child Health. 2000; 5:471-472
7 Bass M Sudden Sniffing Death. JAMA. 1970; 212:2075-2079
8 Kosa F Indictment in a case of fatal intravenous petrol injection. Morphol Igazagugyi Orv. 1981; 21:69-72
9 Banner W, Walson PD Systemic toxicity following gasoline aspiration. Am J Emerg Med. 1983; 3:292-294
10 Farahvash MR, Yegane RA, Bashashati M Surgical approach to hydrocarbon injection in upper extremities: case series. Int J Surg. 2009; 7:382-386
11 Vaziri ND, Jeminson-Smith P, Wilson AF Hemorrhagic pneumonitis after intravenous injection of charcoal lighter fluid. Ann Intern Med. 1979; 90:794-795
12 Domej W, Mitterhammer H, Stuaber R Successful outcome after intravenous gasoline injection. J Medical Toxicology. 2007; 3:173-177
13 Bindlish V Subcutaneous gasoline injection. Am J Emerg Med. 1993; 11:676-677
14 Geoffray C, Chosidow O, Reygagne A Cutaneous necrosis induced by injection of hydrocarbons. Arch Dermatol. 1992; 128:997-998
15 Kleinschmidt K, Goto CS, Roth B Multiple Small-volume Subcutaneous WD-40 Injections with Severe Local and Systemic Toxicity (abstract). Clin Toxicology. 1999; 37:653


