| Author | Affiliation |
|---|---|
| Gus M. Garmel, MD | Stanford University School of Medicine/Kaiser Permanente, Santa Clara |
INTRODUCTION
Patients who present with electrocardiograms (ECGs) demonstrating wide complex tachycardias (WCTs) are often challenging to clinicians. Not only may the patient present with (or be at risk for) hemodynamic compromise, but their treatment may result in hemodynamic collapse if the incorrect pharmacologic agent is selected. In Part 1 of this article,1 the identification, epidemiology, and electrophysiology of WCTs were discussed. In this article, treatment of WCTs and miscellaneous causes of this condition will be described.
In patients presenting with WCTs, correct interpretation of the ECG should not be the primary concern of emergency physicians. In fact, it is appropriate (and may be preferred) to “diagnose” the ECG as “wide complex tachycardia of unknown (or uncertain) etiology.” This may allow the treating clinician to focus on the patient and his or her hemodynamic status, rather than the academic exercise of ECG interpretation. The most important aspect of treating patients who present with WCTs is to select a therapeutic approach that does no harm. Several diagnostic algorithms were provided for the interpretation of WCTs, although none have proven superior over others, and great debate continues among researchers as to the preferred approach. Given this circumstance of uncertainty, proper treatment will be described for conditions resulting in WCTs.
It is critical to note that once a WCT is identified, the use of certain pharmacologic therapies may have deleterious effects on patients. Verapamil and diltiazem are calcium channel blockers (CCBs) that should be avoided in WCTs, as cardiac arrests from hemodynamic collapse have been reported following their administration.2,3 This is especially true in infants. Not only do these agents cause negative inotropy and at times profound vasodilation, but they may also allow WCTs to degenerate into VFIB. CCBs slow conduction at the AV node so that accessory pathways can be preferentially used; this results in ventricular rates that approach atrial rates. In addition, verapamil may shorten the effective refractory period of accessory pathway tissues, which is especially dangerous if AFIB and WPWS coexist (Figure 1). Digoxin should be avoided as well in the pharmacologic management of WCTs, as it may facilitate conduction via the accessory pathway. Shortening the refractory period of this pathway is particularly concerning in individuals with anterograde conduction over an accessory pathway (such as the case in AFIB with WPWS), as lethal ventricular rates may develop in response to fast or chaotic atrial rates. Propranolol (or other beta-blocking agents) may facilitate AV conduction via the accessory pathway, which can increase the ventricular rate to dangerous levels during AFIB. Lidocaine is no longer considered by the American Heart Association (AHA) as the drug of choice in WCTs of uncertain origin; good evidence supports alternative agents as being superior. If lidocaine is used, it should be administered with extreme caution, as it has been demonstrated to speed conduction through bypass tracts in experimental models. The use of oral agents in the emergency management of WCTs has no current therapeutic role.
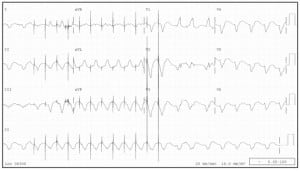
ECG representing Wolff-Parkinson-White Syndrome (WPWS) with Atrial Fibrillation (AFIB). Note the wide QRS complexes, and the irregularly irregular rhythm. In lead II, the axis changes. A slurred delta wave can be identified in the left precordial leads, since the overall rate is not as fast as it might be when these conditions coexist. The R-R interval of the first two QRS complexes seen in leads V1–3 approaches 300, which is extremely dangerous.
The clinical dictum “do no harm” is especially important when it comes to the management of WCTs, as delays to definitive therapy or their mismanagement (or both) can result in considerable morbidity and mortality. The patient’s clinical condition, not the ECG tracing, should be addressed and treated. If the patient is unstable without a pulse, this patient (and the WCT rhythm) should be treated as any patient in ventricular fibrillation, with defibrillation, airway management, and ACLS drugs according to current AHA algorithms. All unstable patients with a pulse should be treated using the unstable VT AHA algorithm, with consideration for sedation prior to synchronized cardioversion. The airway in these patients should be managed with appropriate aggressiveness. The amount of electrical energy needed to cardiovert this WCT to a stable rhythm is generally less than that required for VFIB. In short, all undetermined WCTs should be treated as if they are ventricular in origin (VT). Unless the clinician is absolutely certain that the WCT is supraventricular in origin, pharmacologic agents used in the treatment of SVTs should not be administered (Table 1).
The use of adenosine as a rapid IV push in patients presenting with WCTs deserves special mention. This agent has tremendous efficacy converting SVTs, but on occasion has both diagnostic use as well as success converting some idiopathic causes of VT, especially cases originating in the fascicle.5,6 Adenosine should be used with caution in the diagnosis and management of WCTs, as prolonged AV block is likely to occur. The rapid administration of adenosine may help identify the underlying etiology of certain WCTs by slowing the heart rate or unmasking accessory tracts.7 Despite it being considered safe to use in patients presenting with WCTs,8 there are a few reports of complications following adenosine use. Adenosine may predispose the heart to atrial fibrillation, and may cause the cardiac rhythm to deteriorate into very rapid ventricular rates in patients with pre-excitation syndrome.9 Fortunately, this increase in ventricular rate was not shown to consistently cause hemodynamic deterioration in one study.10 Adenosine has also been reported to induce torsade de pointes11, and has proarrhythmic potential, especially in patients with aberrant conduction pathways, which may produce VT or other WCTs.12Other authors share concern that the extranodal effects of adenosine may ultimately lead to pitfalls and misidentification of WCTs.13 The current AHA guidelines for tachycardia with pulses mentions the use of adenosine for regular wide QRS complexes if SVT with aberrancy is identified as the rhythm. It neither suggests nor recommends its use in a diagnostic trial.4
In several areas of the 2005 AHA Tachycardia with pulses algorithm, “expert consultation” is either advised or should be considered. Once the patient is deemed clinically stable, and a candidate for pharmacologic intervention, the determination of regular versus irregular rhythm is necessary. For regular rhythms, any VT or uncertain rhythm should, according to the guidelines, be treated with IV amiodarone, with preparation for elective synchronized cardioversion (as long as the patient remains clinically stable). For patients with SVT with aberrant conduction, adenosine is suggested. If, on the other hand, the WCT is irregular, pharmacologic therapy depends on whether or not AFIB with aberrancy (in which diltiazem or beta-blockers are appropriate) or AFIB with WPWS (in which amiodarone is the agent of choice, and AV nodal blocking agents [e.g., adenosine, digoxin, diltiazem, verapamil] should be avoided) is most likely. According to the 2006 Guidelines for the Management of Patients with Atrial Fibrillation published in Circulation, “… in hemodynamically stable patients with pre-excitation, type I antiarrhythmic agents or amiodarone may be administered intravenously.” These guidelines further state that if the dysrhythmia causes hemodynamic compromise, early direct current cardioversion is indicated.14
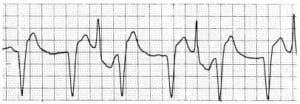
Torsade de pointes is a special type of WCT, during which the electrical axis “twists” around the horizontal axis (Figure 2). It is categorized as a form of polymorphic VT. Cycles of alternating electrical polarity of the QRS complexes occur about the isoelectric axis. Torsade de pointes can be initiated when a premature ventricular contraction (PVC) falls on the T wave, or by ventricular couplets or triplets. It commonly has a long-short initiation sequence, and may be more likely during episodes of bradycardia.15 It has been associated with prolonged QT syndrome, multiple electrolyte abnormalities, many antiarrhythmic agents (ibutilide, sotalol, and the Class Ia agents, for example), phenothiazines, TCAs, and pentamidine.16,17 In addition to withdrawing the causative agent and correcting electrolyte abnormalities, pharmacologic treatment is with a loading dose of IV magnesium sulfate, followed by infusion. Isoproterenol is no longer recommended as treatment for torsade de pointes, as it increases myocardial oxygen consumption and the likelihood for rhythm disturbances. Overdrive pacing to a heart rate of 90 – 130 beats per minute is generally successful in terminating torsade de pointes if it does not respond to magnesium.
It should be noted that neither lidocaine nor procainamide appear in these updated 2005 AHA ACLS treatment algorithm flow diagrams. Procainamide and sotalol do appear in the accompanying text as alternative drugs for wide complex regular tachycardias.18
Miscellaneous WCTs
Several additional causes of WCTs should be considered when evaluating and treating individuals presenting with ECGs demonstrating WCTs (Table 2). Hemodynamic stability remains the main principle directing patient management. These additional causes of WCTs have markedly different treatment strategies, depending on their etiologies.
Pacemaker-mediated tachycardias can be investigated using a pacemaker magnet over the pacemaker generator. As transvenous pacemaker leads are placed in the right ventricle, the QRS complexes generated by the pacemaker are widened. Any pacemaker-mediated tachycardias will therefore be WCTs. Adenosine may elicit hidden atrial activity, and it is particularly safe as the pacemaker should respond if prolonged AV block or a brief period of asystole occurs. With newer pacemakers, this condition is less common.28 Figure 3 demonstrates a wide complex tachycardia in a patient with a pacemaker, although not pacemaker-mediated.
Tricyclic antidepressant (TCA) overdose causes a WCT due to the quinidine-like effects of these drugs. The class IA sodium channel blocking activity widens the QRS complex, with tachycardia being part of the toxidrome caused by these agents. A high index of suspicion should help identify this clinical scenario. Treatment is with IV bicarbonate, aggressive airway protection, and supportive measures. Agents with similar properties have been reported to result in WCTs due to quinidine-like effects on the sodium channels, especially in toxic ingestions or overdoses.
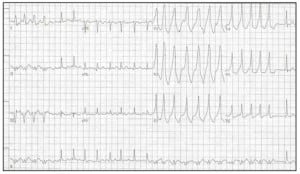
Severe hyperkalemia may present with WCT as a late ECG manifestation of this condition (Figure 4). A high index of suspicion should cause one to consider this etiology, especially in the setting of renal failure. Initial treatment includes IV calcium to stabilize the myocardium, IV bicarbonate, IV glucose and insulin, and inhaled albuterol. An additional therapeutic regimen includes sodium polystyrene sulfonate (Kayexalate) resin, although this treatment does not take immediate effect and can be challenging to administer. Emergent hemodialysis is the definitive treatment for acute hyperkalemia with WCT, and should be arranged as quickly as possible.
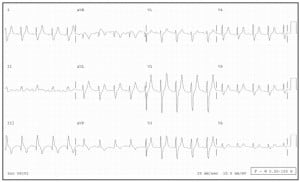
Hyperkalemia causing a WCT in a patient with chronic renal failure (K+ 9.1). The patient’s heart rate is 108 bpm, the QRS duration is 134 msec. Note the prominent, narrow peaked T waves (esp. V2, V3), which, with historical factors, should help identify this diagnosis.
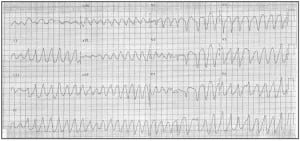
Severe digitalis overdose can cause a bidirectional VT.29,30,31 This WCT generally has a RBBB pattern, with the QRS complexes alternating between right and left axis deviation in the limb leads. This distinct pattern of alternating axis deviation is due to alternating impulse formation in the left posterior and left anterior fascicles (Figures 5a, b). Again, a high index of suspicion should assist in making this diagnosis, as individuals with severe digitalis overdose may have symptoms such as visual changes (especially color vision), changes in behavior, gastrointestinal disturbances, and access to this medication. This condition is more likely in elderly patients with mild dehydration or renal insufficiency, or in individuals following overdose. Treatment includes withdrawal of the offending agent and supportive care; definitive therapy is administration of digitalis-specific antibodies.
CONCLUSION
The treatment of patients presenting with wide complex tachycardias should be based on the clinical or hemodynamic status of the individual, not the ECG. The ECG in WCTs is not always helpful in determining the etiology of the rhythm disturbance. It may not even have clinical relevance in the emergent setting.32,33,34 None of the sets of diagnostic criteria described previously has proven to have 100% accuracy. Therefore, clinicians should always treat the patient, not the ECG, when managing patients presenting with WCTs. Unstable patients require defibrillation or emergent cardioversion (with sedation considered). Pharmacologic treatment of stable patients should occur according to the most updated AHA ACLS guidelines, with “expert consultation” advised. As research continues, newer pharmacologic agents and treatment modalities are likely to become more common in the ED setting.
When the ECG diagnosis of a WCT is uncertain, clinicians should consider it to be VT and treat it as such. Even given referral bias, the literature consistently identifiesVT to be much more likely than SVT with aberrant conduction, which makes up part of the rationale behind this recommendation. More important, however, is that treating WCTs of uncertain etiology as rhythms originating above the ventricle may result in clinical deterioration, including cardiovascular collapse. Clinicians should be familiar with agents to avoid when treating individuals who present with WCTs. Furthermore, some pharmacologic agents used to treat VT may in fact terminate a WCT of supraventricular origin. Finally, clinicians must remain vigilant when evaluating and managing patients presenting with WCTs. They must look for ECGs demonstrating irregular wide QRS complexes, as such ECGs may represent atrial fibrillation with Wolff-Parkinson-White Syndrome (WPWS). Caution should be maintained in patients presenting with a fast, irregular, wide-complex rhythm, as serious consequences may occur from its misidentification or the use of pharmacologic agents that decrease refractory periods in or speed conduction through alternative pathways.
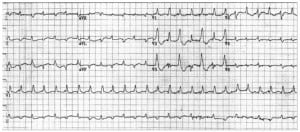
12-lead ECG from a different patient demonstrating bidirectional ventricular tachycardia from digitalis toxicity. The axes of the RBBB-morphology QRS complexes alternate.
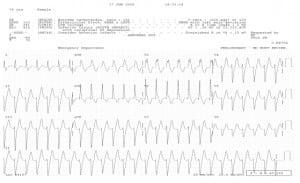
Example of an unusual WCT known as Idiopathic (benign) Ventricular Tachycardia. This is caused by a re-entry loop in the apex of the LV, resulting in the left superior axis and RBBB pattern. Also called Left Ventricular Tachycardia, it often responds to Verapamil. (Note — CCBs should not be used in WCTs unless recommended by a cardiologist or electrophysiologist.)

Summary pearls for Wide Complex Tachycardias
Footnotes
Dr. Garmel would like to recognize Doris Hayashikawa and her staff at Kaiser Permanente Medical Center’s Santa Clara, CA Health Sciences Library for their continued support on this and other academic projects.
Supervising Section Editors: Sean O. Henderson, MD
Submission history: Submitted August 18, 2007; Revision Received October 19, 2007; Accepted November 26, 2007
Full text available through open access at http://escholarship.org/uc/uciem_westjem
Address for Correspondence: Gus M. Garmel, MD, FACEP, FAAEM, Kaiser Permanente, c/o Emergency Department, 700 Lawrence Expressway, Santa Clara, CA 95051
Email: Gus.Garmel@kp.org
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Garmel GM. Wide Complex Tachycardias: Understanding this complex condition (Part 1) WestJEM. 2008;9:28–39. [PMC free article] [PubMed]
2. Buxton AE, Marchlinski FE, Doherty JU, et al. Hazards of intravenous verapamil for sustained ventricular tachycardia. Am J Cardiol. 1957;59:1107–1110. [PubMed]
3. McGovern B, Garna H, Ruskin JN. Precipitation of cardiac arrest by Verapamil in patients with Wolff-Parkinson-White syndrome. Annals Int Med. 1986;104:791–794.
4. 2005 AHA ACLS guidelines (Tachycardia with pulses) Circ. 2005;112:iv-70.
5. Kassotis J, Slesinger T, Festic E, et al. Adenosine-sensitive wide-complex tachycardia: An Uncommon variant of idiopathic fascicular ventricular tachycardia. Angiology.2003;54:369–372. [PubMed]
6. Herbert ME, Votey SR. Adenosine in Wide-Complex Tachycardia. Ann Emerg Med.1997;29:172–174. [PubMed]
7. Ilkhanipour K, Berrol R, Yealy DM. Therapeutic and diagnostic efficacy of adenosine in Wide-Complex Tachycardia. Ann Emerg Med. 1993;22:1360–1364. [PubMed]
8. Marill KA, Wolfram S, DeSouza IS, et al. Adenosine for Wide-Complex Tachycardia: Efficacy and Safety. Acad Emerg Med. 2004;11:502A.
9. Lopez JA, Lufschanowski R, Massummi A. Transesophageal Electrocardiography and Adenosine. Texas Heart. Inst Jour. 1994;21:130–133.
10. Sharma AD, Klein GJ, Yee R. Intravenous adenosine triphosphate during wide QRS complex tachycardia: safety, therapeutic efficacy, and diagnostic utility. Am J Med.1990;88:337–343. [PubMed]
11. Harrington GR, Froelich EG. Adenosine-induced torsade de pointes. Chest.1993;103:1209–1302.
12. Tsai C, Chang W. A wide QRS complex tachycardia following intravenous adenosine.Resusc. 2004;61:240–241.
13. Lee KL-F, Tai Y-T. Adenosine in wide complex tachycardia: Potential pitfalls in diagnostic value. Ann Emerg Med. 1994;24:741–747. [PubMed]
14. Fuster V, et al. ACC/AHA/ESC 2006 Guidelines for the management of patients with atrial fibrillation. Circ. 2006;114:e257–354.
15. Vukmir RB. Torsade de Pointes: A review. Am J Emerg Med. 1991;9:250–255.[PubMed]
16. Keren A, Tzivoni T, Gavish D, et al. Etiology, warning signs and therapy of Torsade de Pointes: A study of 10 patients. Circ. 1981;64:1167–1173.
17. Engrav MB, Coodley G, Magnusson AR. Torsade de pointes after inhaled pentamidine.Ann Emerg Med. 1992;21:1430–1405. [PubMed]
18. 2005 AHA ACLS guidelines. Circ. 2005;112:iv-72.
19. Garmel GM. Wide Complex Tachycardias. Hosp Phys: Emergency Medicine Board Review manual. 1998;2:1–14.
20. Francis J, Hamzeh RK, Lantin-Hermoso MR. Lithium toxicity-induced wide complex tachycardia in a pediatric patient. J Peds. 2004:235–240.
21. Lange RA, Hillis LD. Cardiovascular complications of cocaine use. NEJM.2001;345:351–358. [PubMed]
22. Kerns W, Garvey L, Owens J. Cocaine-induced wide complex dysrhythmia. J Emerg Med. 1997;15:321–329. [PubMed]
23. Levis JT, Garmel GM. Cocaine-associated chest pain. Emerg Med Clin N Am.2005;23:1083–1103.
24. Clark RF, Vance MV. Massive diphenhydramine poisoning resulting in a wide-complex tachycardia: Successful treatment with sodium bicarbonate. Ann Emerg Med.1992;21:318–321. [PubMed]
25. Hollowell H, Mattu A, Perron AD, et al. Wide-complex tachycardia: beyond the traditional differential diagnosis of ventricular tachycardia vs supraventricular tachycardia with aberrant conduction. Am J Emerg Med. 2005;23:876–889. [PubMed]
26. Kefalas S, Ezenkwele U. Wide-complex tachycardia as the presenting complaint in a case of malingering. J Emerg Med. 2006;30:159–161. [PubMed]
27. Knight BP, Pelosi F, Michaud GF, et al. Clinical consequences of electrocardiographic artifact mimicking ventricular tachycardia. NEJM. 1999;341:1270–1274. [PubMed]
28. Barber CR, Garmel GM. Pacemaker-associated Tachycardia. Acad Emerg Med.1997;4:150–153. [PubMed]
29. Kummer JL, Nair R, Krishnan SC. Images in cardiovascular medicine. Bidirectional ventricular tachycardia caused by digitalis toxicity. Circ. 2006;113:e156–e157.
30. Piccini J, Zaas A. Cases from the Osler Medical Service at Johns Hopkins University. Digitalis toxicity with bidirectional ventricular tachycardia. Am J Med. 2003;115:70–71. [PubMed]
31. Ma G, Brady WJ, Pollack M, et al. Electrocardiographic manifestations: digitalis toxicity. J Emerg Med. 2001;20:145–152. [PubMed]
32. Chenevert M, Lewis RJ. Ashman’s phenomenon – a source of nonsustained wide-complex tachycardia: case report and discussion. J Emerg Med. 1992;10:179–183.[PubMed]
33. Smith DC. [letter to the editor] . J Emerg Med. 1993;11:98. [PubMed]
34. Wrenn K. Management strategies in wide QRS complex tachycardia. Am J Emerg Med. 1991;9:592–597. [PubMed]