| Author | Affiliation |
|---|---|
| Kelly Kesler, MD | University of California, Irvine, Department of Emergency Medicine, Irvine, California |
| Shadi Lahham, MD, MS | University of California, Irvine, Department of Emergency Medicine, Irvine, California |
CASE PRESENTATION
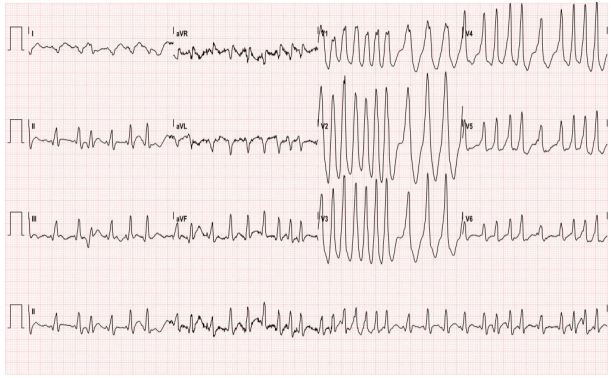
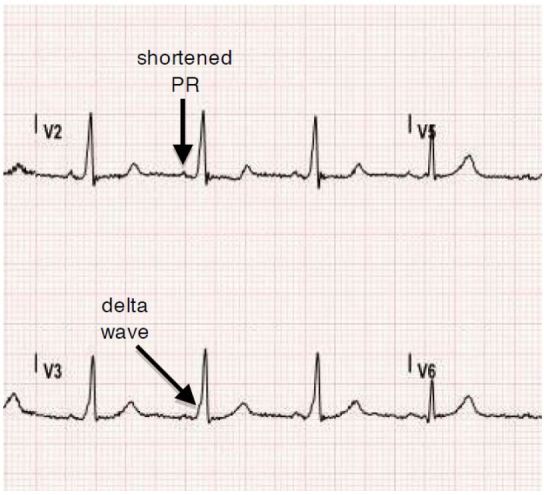
A 29-year-old female with no significant past medical history presented with palpitations, nausea, diaphoresis and lightheadedness. Symptoms began 15 minutes prior to arrival. She reported several similar episodes previously that self-resolved within seconds, but had no previous medical evaluations for these symptoms. Initial vital signs were significant for blood pressure of 93/61, irregular heart rate between 180 and 200, respiratory rate of 18, and oxygen saturation of 99% on room air. Physical examination was otherwise unremarkable. The electrocardiogram (ECG) is shown in Figure 1. This was interpreted as atrial fibrillation with rapid ventricular rate, and the patient was treated with rate control with no effect. The patient later spontaneously converted to normal sinus rhythm and repeat ECG was notable for delta waves concerning for Wolff-Parkinson-White Syndrome (WPW) as seen in Figure 2. She was admitted to cardiology for cardiac ablation.
DIAGNOSIS
Wolff-Parkinson-White (WPW) syndrome is a conduction disorder of the heart caused by pre-excitation accessory pathway resulting in tachyarrhythmias. The prevalence is approximately 0.07% of the population, and many patients often present with the chief complaint of “palpitations.”1 A diagnosis of WPW is made by certain characteristics identified on an ECG. These characteristics include a short PR interval < 0.12 seconds caused by faster electrical conduction through the accessory pathway than the atrioventricular (AV) node, and a delta wave, or upsloping of the QRS (Figure 2), due to rapid ventricular depolarization caused by the rapid conduction through the accessory pathway.2, 3 Diagnosing this disorder can be challenging, specifically when patients present with tachyarrhythmias and the pathognomonic delta wave becomes buried. The inherent rate of the AV node is approximately 180–200. Therefore, when a patient presents in an arrhythmia with a rate upwards of this intrinsic rate, an orthodromic atrioventricular reentrant tachycardia (AVRT) with a re-entrant component, such as WPW, should be immediately suspected 3.
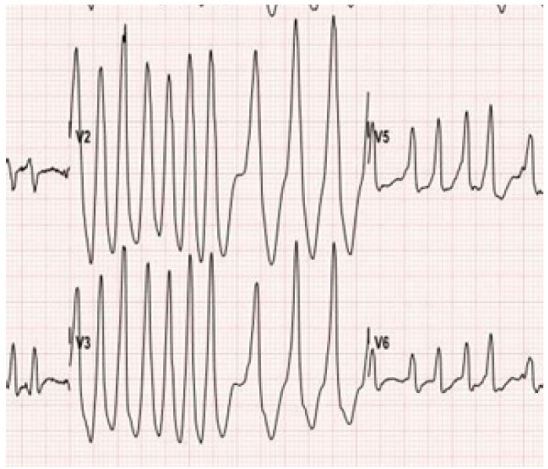
In our case, the patient demonstrated a heart rate of up to 300 on the ECG (Figure 3). Once this patient converted back to normal sinus rhythm, the classic delta wave and short PR interval was easily identifiable (Figure 2). According to the 2014 American Heart Association guidelines for management of patients with atrial fibrillation, the class I recommendation regarding management of patients with pre-excited atrial fibrillation with rapid ventricular response includes IV infusion of procainamide if patient is hemodynamically stable, immediate synchronized cardioversion if the patient is unstable, and subsequent catheter ablation of the accessory pathway.4, 5 Administration of amiodarone, adenosine, beta blockers, and calcium channel blockers should be avoided as these will isolate the accessory pathway and thus predispose to fatal arrhythmias such as ventricular fibrillation by increasing the ventricular rate.3, 4, 5, 6, 7
Footnotes
Section Editor: Rick A. McPheeters, DO
Full text available through open access at http://escholarship.org/uc/uciem_westjem
Address for Correspondence: Kelly Kesler, MD, University of California, Irvine, Department of Emergency Medicine, 333 The City Boulevard, West Suite 640, Orange, CA 92868. Email: kkesler@uci.edu. 7 / 2016; 17:469 – 470
Submission history: Revision received March 10, 2016; Submitted April 8, 2016; Accepted April 13, 2016
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Chiu SN, Wang JK, Wu MH, et al. Cardiac conduction disturbance detected in a pediatric population. J Pediatr. 2008;152:85-89.
2. Wolff L, Parkinson J, White PD. Bundle-branch block with short P-R interval in healthy young people prone to paroxysmal tachycardia. 1930. Ann Noninvasive Electrocardiol. 2006;11:340.
3. Yealy DM, Kosowsky JM. Chapter 79: Dysrhythmia. Rosen’s Emergency Medicine Concepts and Clinical Practice. 2014.
4. January CT, Wann LS, et al. 2014 AHA/ACC/HRS Guideline for the Management of Patients With Atrial Fibrillation: Executive Summary.
5. Blomstrom-Lundqvist C, Scheinman MM, Aliot EM, et al. ACC/AHA/ESC guidelines for the management of patients with supraventricular arrhythmias: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the European Society of Cardiology Committee for Practice Guidelines (Writing Committee to Develop Guidelines for the Management of Patients With Supraventricular Arrhythmias) developed in collaboration with NASPE-Heart Rhythm Society. J Am Coll Cardiol. 2003;42:1493-531.
6. McGovern B, Garan H, Ruskin JN. Precipitation of cardiac arrest by verapamil in patients with Wolff-Parkinson-White syndrome. Ann Intern Med. 1986;104:791-794.
7. Simonian SM, Lotfipour S, Wall C, et al. Challenging the superiority of amiodarone for rate control in Wolff-Parkinson-White and atrial fibrillation. Intern Emerg Med. 2010;5(5):421-6.


