| Author | Affiliation |
|---|---|
| Jason D. Heiner, MD | Madigan Army Medical Center, Department of Emergency Medicine, Fort Lewis, WA |
A 48-year-old male presented to the emergency department with enlarging regions of ecchymoses over the posterior aspect of both legs (Figure 1). Four days earlier he had the sudden onset of severe achy hamstring pain during a 50-yard sprint. He denied weakness, similar prior episodes, or bleeding abnormalities. Both lower extremities had full range of motion, no loss of strength, a normal knee exam, and moderate distal hamstring tenderness without swelling or palpable soft tissue defects. A complete blood cell count, prothrombin time, and partial thromboplastin time were all normal. Clinically, this patient had suffered a second-degree hamstring strain.
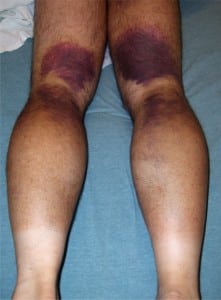
The hamstring muscle complex of the posterior thigh extends from the ischial tuberosity of the pelvis to the proximal tibia and fibula and is the most commonly injured muscle group in sports involving running and sprinting.1 Risk factors for injury include poor flexibility, inadequate warm-up, muscle imbalance and previous hamstring injury.1,2 These injuries are classified by the degree of muscle strain. First-degree strains represent a stretching injury with microscopic damage. Second-degree strains represent a partial tear that may be accompanied by weakness and hematomas within and around the muscle. A functionally disabling third-degree strain is a complete rupture of the muscle-tendon unit that usually occurs as an avulsion injury from the ischial tuberosity.3 Plain radiography may identify the crescent-shaped fragment of a proximal avulsion injury, and ultrasound or magnetic resonance imaging may delineate a macroscopic injury and help to guide therapy and predict prognosis.3 Most hamstring injuries should be acutely treated with rest, ice, compression, elevation, and nonsteroidal anti-inflammatories, but surgery may be indicated to reattach an avulsed fragment or to repair soft tissue ruptures of muscle or tendon.1,2,3 Appropriate referral for individualized rehabilitation may improve a patient’s functional outcome and an athlete’s ability to return to competition.
Footnotes
Supervising Section Editor: Sean Henderson, MD
Submission history: Submitted July 31, 2009; Revised August 17, 2009; Accepted August 18, 2009
Full text available through open access at http://escholarship.org/uc/uciem_westjem
Address for Correspondence: Jason Heiner, MD, Department of Emergency Medicine, Madigan Army Medical Center, 9040 Fitzsimmons Ave, Fort Lewis, WA 98431
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Drezner JA. Practical management: hamstring muscle injuries. Clin J Sport Med. 2003;13:48–52.[PubMed]
2. Mann G, Shabat S, Friedman A, et al. Hamstring injuries. Orthopedics. 2007;30:536–40. [PubMed]
3. Davis KW. Imaging of the hamstrings. Semin Musculoskelet Radiol. 2008;12:28–41. [PubMed]


