| Author | Affiliation |
|---|---|
| Charles V. Pollack, Jr., MA, MD | University of Pennsylvania, Pennsylvania Hospital, Department of Emergency Medicine, Philadelphia, PA |
| David E. Slattery, MD | University of Nevada School of Medicine, Department of Emergency Medicine, Las Vegas, NV |
We are investigating the potential role for vibration response imaging (VRI) in the prompt emergency department (ED) evaluation of patients presenting with dyspnea to aid in differentiation between chronic obstructive pulmonary disease (COPD) and heart failure (HF). VRI is a noninvasive, bedside computer-based technology that creates a visually dynamic two-dimensional image of distribution of vibration within the lungs during the respiratory process. The acoustic signals, recorded from 36 posteriorly positioned surface skin auditory sensors, are transferred to a hardware board where several stages of filtering are applied to select a specific frequency band. The filtered output signal frequencies are presented as a gray-scale coded dynamic image consisting of a series of 0.17 s frames and as a table featuring the percentage contribution of each lung and lung sector (upper, middle, lower) to the total vibration signal. Darker images represent more prominent airway vibration, but do not necessarily differentiate laminar from turbulent flow. These images and calculations may be useful in delineating HF from other lung disease in acutely dyspneic patients.1
The patient whose image is presented here is a 55-year-old male who presented with shortness of breath and bilateral lower extremity edema. Vital signs at triage were pulse of 88 beats per minute, blood pressure of 160/108 mmHg and respiratory rate of 18 breaths per minute. He gave no history of respiratory or cardiac disease but was a long-time heavy tobacco smoker; his portable chest radiograph was unremarkable. Serum brain natriuretic peptide (BNP) was 136 pg/ml. At the bedside, the emergency physician obtained a VRI (Figure).
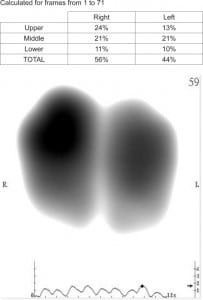
VRI clearly showed bibasilar diminution both in the image (note the darker intensity as well as broader area in the upper lungs) and as quantified in the table. This pattern in VRI is typical for an acute HF presentation. Bedside transthoracic echocardiography revealed an estimated left ventricular ejection fraction of only 35%. The patient was given intravenous diuretic and nitroglycerin therapy resulting in significant improvement in his dyspnea and reduction in his blood pressure to 146/96 mmHg. As an inpatient, serial troponin assays were within normal limits and the patient responded well to therapy for heart failure. The VRI was more helpful than the BNP level in guiding acute management in the ED; the limitations of BNP have been recently discussed.2
VRI may be useful in the ED for differentiating the origin of acute dyspnea. An ED-based prospective trial has begun to investigate this use.
Footnotes
Supervising Section Editor: Sean Henderson, MD
Submission history: Submitted August 16, 2010; Accepted September 13, 2010
Reprints available through open access at http://escholarship.org/uc/uciem_westjem
Address for Correspondence: Charles V. Pollack, Jr., MA, MD, Deparrtment of Emergency Medicine, Pennsylvania Hospital, 800 Spruce St., Philadelphia, PA 19107
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Wang Z, Baumann BM, Slutsky K, et al. Respiratory sound energy and its distribution patterns following clinical improvement of congestive heart failure: a pilot study. BMC Emerg Med. 2010 Jan 15;10(1):1. [Epub ahead of print] [PMC free article] [PubMed]
2. Lokuge A, Lam L, Cameron P, et al. B-type natriuretic peptide testing and the accuracy of heart failure diagnosis in the emergency department. Circ Heart Fail. 2010 Jan;3(1):104–10. [PubMed]


