| Author | Affiliation |
|---|---|
| Thomas E. Terndrup, MD | Penn State College of Medicine, Department of Emergency Medicine, Hershey, Pennsylvania |
| Sameer Ali, MD, MPH | Penn State College of Medicine, Department of Emergency Medicine, Hershey, Pennsylvania |
| Steve Hulse, MEd | JPL Integrated Communications, Inc., Harrisburg, Pennsylvania |
| Michele Shaffer, PhD | Penn State College of Medicine, Department of Public Health Sciences, Hershey, Pennsylvania |
| Tom Lloyd, PhD | Penn State College of Medicine, Department of Public Health Sciences, Hershey, Pennsylvania |
ABSTRACT
Introduction:
Elders who utilize the emergency department (ED) may have little prospective knowledge of appropriate expectations during an ED encounter. Improving elder orientation to ED expectations is important for satisfaction and health education. The purpose of this study was to evaluate a multi-media education intervention as a method for informing independently living elders about ED care. The program delivered messages categorically as, the number of tests, providers, decisions and disposition decision making.
Methods:
Interventional trial of representative elders over 59 years of age comparing pre and post multimedia program exposure. A brief (0.3 hour) video that chronicled the key events after a hypothetical 911 call for chest pain was shown. The video used a clinical narrator, 15 ED health care providers, and 2 professional actors for the patient and spouse. Pre- and post-video tests results were obtained with audience response technology (ART) assessed learning using a 4 point Likert scale.
Results:
Valid data from 142 participants were analyzed pre to post rankings (Wilcoxon signed-rank tests). The following four learning objectives showed significant improvements: number of tests expected [median differences on a 4-point Likert scale with 95% confidence intervals: 0.50 (0.00, 1.00)]; number of providers expected 1.0 (1.00, 1.50); communications 1.0 (1.00, 1.50); and pre-hospital medical treatment 0.50 (0.00, 1.00). Elders (96%) judged the intervention as improving their ability to cope with an ED encounter.
Conclusion:
A short video with graphic side-bar information is an effective educational strategy to improve elder understanding of expectations during a hypothetical ED encounter following calling 911.
INTRODUCTION
Little is known about the impact of public education on how emergency departments (ED) function and understanding how care is provided there. Given the expanding elder population, with its medical complexity (e.g. multiple co-morbidities) and tr higher use rates of ED services, it is important to explore educational strategies in order to evaluate methods of improving their understanding of the ED and the care it provides.1–6
While patient education in the ED can be challenging, preliminary studies have demonstrated its utility in asthma, myocardial infarction, and trauma.7 Not only do elderly patients have a 2- to 2.5-fold higher per capita ED use rate, they have a higher prevalence of communication challenges, making education more difficult. Multimedia technology, which can circumvent both receptive and integrative learning challenges, is recognized as an effective tool for patient education, including elders.8 We tested the hypothesis that specific learning objectives centered on a hypothetical scenario of a patient with chest pain when presented in a multimedia education program could be assessed using audience response technology and that such a program would be effective in educating elders about ED care. Multimedia education scenarios, like this one, are effective with large groups and could provide a cost-effective method to educate elderly patients about ED encounters.
METHODS
Development of video materials
Following development of 3 overall steps in common emergency care, learning objectives were agreed upon by a multidisciplinary group, which included 2 veteran emergency physicians, a multimedia expert with 30 years of experience, a film producer with 25 years of experience and a Penn State College of Medicine teacher with 35 years of experience who created 5 previous multimedia teaching programs. We focused on 3 major areas related to ED care:
1. To demystify ED encounters
To accomplish this we sought to teach our audience that the ED operates differently in comparison to other out-patient clinic or in-patient, hospital-based care. Our goal was to show that in order to assess rapidly evolving emergency care conditions, a team approach is often required. We addressed this in the video by illustrating an emergency visit as a journey, not disorganized chaos, as the public may commonly believe.
2. To teach the viewer the need for multiple healthcare providers in the ED
Patients’ non-ED healthcare usually revolves about a central physician and it is logical for them to expect that their ED care will be more or less the same. We addressed this concept by introducing the viewer to the multiple healthcare providers in the ED and explaining their functions. This was reinforced by a sequential side-bar listing, highlighting the numbers and types of providers involved.
3. To teach the viewer that in the ED the patient and family cannot be in total control
Conflicts may occur when patients and /or their families feel that they do not have the same degree of control of their care as they would have in a non-ED medical encounter, e.g., a visit to their doctor’s office. We designed the program to illustrate that unexpected and unplanned incidents are common in the ED and often require immediate attention. This urgency sometimes precludes the full involvement of the patient or family in the decision-making process in order to provide the most rapid ED care. The above concepts were taught by using 5 clinical care domains in the ED that are different from other arenas of medical care that patients may be more familiar with: 1.) the number of anticipated and common procedures; 2.) the number of healthcare providers involved in care; 3.) the number of ED healthcare providers who keep the patients and family members informed; 4.) the role of the patient and others in the ED with respect to decision making, and 5.) and the role of pre-hospital care providers.
The 18-minute video follows 1 patient from development of an emergency need at home, through the 911 call, the ambulance trip, the intake at the ED, and the sequence of evaluations that often follow a patient complaining of chest pain and associated symptoms. It ends with the patient being counseled about transfer to the catheterization laboratory, for a percutaneous intervention. The “patient” is accompanied by his wife and has encounters with an ambulance medic, an ambulance nurse, an ED technician, an ED charge nurse, a primary and a secondary bedside nurse, a radiology technician, an ED resident physician, an attending ED physician, a cardiology fellow, an attending cardiology physician, a member of the registration staff, and a chaplain. Each of the 13 video scenes was scripted to include at least 1 of the learning objectives, and information about each of the 5 learning areas was presented at least twice. The video is opened and closed by a physician describing for the viewers what they will be seeing and asking them to take notice of specific elements of the journey.
Study Subjects
Data Collection
We used an audience response system (ARS; Turning Technology Youngstown, Ohio 44503) to obtain immediate and confidential responses before and after the group viewing of the video. All participants were given audience response “clickers” at the beginning of each session and instructed in their use. The ARS program was used to format and project the questions. Three warm-up questions were given to the audience to familiarize them with the use of the clickers. Before the video was shown each audience was asked to respond to 4 categorical demographic questions and to choose 1 of the 4 Likert responses for each of the 5 ED journey-related questions. After the video the audience was asked to respond to the same 5 ED-journey questions. At the end of the program, 1 of the investigators facilitated an open question-and-answer program on ED encounters, and participants were asked to complete a 2-question program evaluation form. The study was approved as exempt from further human subjects review by our institutional review board.
Data Management and Analysis
The ARS employs wireless handsets that allow participants to respond to multiple choice or Likert scale questions displayed in interactive (Microsoft PowerPoint) slides. Responses were not displayed to the subjects to prevent group biases in response. The pre- and post-test data for respondents were exported as an Excel (Microsoft, Bellingham Washington) file for analysis. Data are reported as frequencies and percentages. We used the Wilcoxon signed-rank test to compare the pre-and post-test scores. Analyses were performed using SAS software (version 9.1, SAS Institute Inc., Cary, North Carolina).
RESULTS
The multimedia educational program was run for 5 different groups: twice at local churches and 3 times at local senior centers. We collected usable data were collected from 105 female and 37 male participants. The program was advertised for independently living seniors, ages 60 to 80 (Table 1). Participants (97%) were over age 60. There was a nearly equal distribution of educational background of the study population reporting high school, some college, a college degree, or a graduate degree as their highest educational level. The study population was predominantly Caucasian.
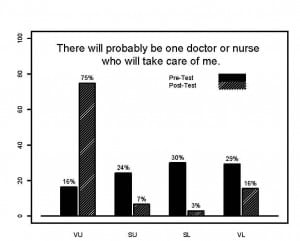
A graphic depiction of the pre- and post- video answers (Figure) to 1 of the 5 test statements is shown. In this case the statement is “There will probably be 1 doctor or nurse who will take care of me” and the study subjects used their ARS clickers to choose 1 of the 4 Likert answers: very unlikely, somewhat unlikely, somewhat likely, or very likely. After watching the video the percent of subjects who thought that it was very unlikely that 1 doctor or 1 nurse would take care of them changed from 16% to 75%. Similar results are presented in Table 2, which compares all of the results for the pre- and post- video questions and shows that overall the learning objectives of the video were achieved. Statistically significant shifts in the responses were seen for 4 of the 5 questions. Therefore, post-test responses were more likely to represent the reality of multidisciplinary ED care. The results of the program evaluation (Table 3) show that 95% reported that they would recommend the program to their friends. Furthermore, 96% reported that, if they had to go to the ED, what they learned from the program would help them to cope with this unique medical care setting.
DISCUSSION
Clinical experiences in the ED can be especially difficult, as patients generally do not anticipate an emergency medical condition or situation. The central goal of this project was to test the efficacy of a short, multimedia program as a tool to educate senior citizens on a very common ED health issue, chest pain. With the goal of conducting a quantitative study on the use of multimedia for education of patients about the ED, we considered the following overarching concepts prior to development of a video-based program: the age group of our target patients, identification of a common, yet serious, ED experience affecting the target patient group, and the major teaching objectives that would benefit such patients. We found that our study population of 142 seniors showed statistically significant improvement for 4 of the 5 question areas while the overall program impact was positive in over 95% of tested subjects.
This study advances our knowledge about an inexpensive multimedia presentation showing an increased understanding of ED encounters, when judged by seniors, a population with significant use of ED resources and frequent misunderstandings about how ED encounters take place.10,11Audience response systems are showing promise in health education and this study confirms their value and adaptability for use by alert, self-selected senior citizens.12,13 The rapid increase in the number of elder patients in America has contributed to strained ED resources and the potential misuse of ED resources by under-educated patients. Since patient education is instruction directed at increasing a patient’s ability to better manage personal health there are several major reasons for developing ways to educate elder patients about care in the ED. First and foremost, adequate patient health knowledge positively influences their health and increases their motivation to follow healthcare instructions. Second, healthcare organizations are mandated by accreditation bodies to provide patient education, and not just at the time of discharge, as is common in ED clinical practice. Third, patient education has been shown to be cost effective. Thus, ED-specific education for elders may improve outcomes and reduce their unnecessary return to the ED.14–17 The ED presents unique challenges to patient education, the most important of which may be that the ED patient is unlikely to be emotionally or physically receptive to health education during an ED visit. Thus, it is important to consider how to provide appropriate ED scenario education to potential elder patients prior to their needing to use what they have learned.18–21
A multimedia approach based on easy-to-follow short videos has several advantages as the mechanism for these educational programs. First, they can be scripted to be both engaging and to carry specific learning objectives. Our use of an ED encounter that begins with chest pain at home is potentially a motivating scenario and may serve as a basis on which other education scenarios could be developed.18 Second, short videos can be used in a wide variety of venues, including, but not limited to, senior community centers, churches, and patient waiting rooms. Third, they can be tested before release to assess their efficacy. Finally, a library of such programs could be of value to community, academic and for-profit healthcare organizations.
LIMITATIONS
This pilot study was conducted to evaluate the effectiveness of multimedia as an education strategy for to teach elders about selected aspects of emergency medicine care. The study intervention did not evaluate reliability or validity. The results are limited to those elders willing and able to participate, and without an acute emergency medical condition. Elders with more profound neurocognitive or chronic medical conditions may not show benefit and were not included in this study. Furthermore, we did not evaluate prior ED visits among participants, which may have influenced understanding of the material presented. Other, more static educational materials may have resulted in similar effects. The sustainability of the benefit may be short-lived, and the perception of an improved understanding may not have led to better use of ED services or a better understanding or acceptability of the ED encounter paradigm. However, this preliminary study was not intended to evaluate long-term ED resource use or knowledge retention. Only a single illness scenario was tested, and others may not have had such an improvement. Positive results may have been increased by the presence of a group format emphasizing positives over negatives. To offset this effect, individual ARS responses were not provided to participants in order to reduce the likelihood of group influences on responses.
CONCLUSION
Multimedia based short educational videos are a promising tool for imparting health education to senior citizens regarding the ED. Further research comparing these and other forms of patient education are needed to better understand the long-term effects on healthcare knowledge and ED use among elders.
Footnotes
Supervising Section Editor: Teresita Hogan, MD
Submission history: Submitted March 27, 2012; Revisions received September 17, 2012; Accepted November 21, 2012
Full text available through open access at http://escholarship.org/uc/uciem_westjem
DOI: 10.5811/westjem.2012.11.12224
Address for Correspondence: Thomas E. Terndrup, MD, 500 University Drive, Penn State College of Medicine, Hershey, Pennsylvania 17033. Email: tterndrup@hmc.psu.edu.
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Samaras N, Chevalley T, Samaras D, et al. Older patients in the emergency department: A review.Ann Emerg Med. 2010;5:261–269. [PubMed]
2. Strange GR, Chen EH. Use of emergency departments by elder patients: A five -year follow-up study. Acad Emerg Med. 1985:1157–1163. [PubMed]
3. Shah MN, Rathouz PJ, Chin MH. Emergency department utilization by noninstitutionalized elders.Acad Emerg Med. 2001;8:267–273. [PubMed]
4. Iwata M, Kuzuya M, Kitagawa Y, et al. Emergency department use by nonagenarian patients.Geriat & Geront Internat. 2006;6:25–31.
5. Shah MN, Glushak C, Karrison TG, et al. Predictors of emergency medical services utilization by elders. Acad Emerg Med. 2003;10:52–58. [PubMed]
6. Horney C, Schmader K, Sanders LL, et al. Health care utilization before and after an outpatient ED visit in older people. Am J Emerg Med. 2011;30(1):135–142. [PMC free article] [PubMed]
7. Wei HG, Camargo CA. Patient education in the emergency department. Acad Emerg Med.2000;7:710–717. [PubMed]
8. Krishna S, Francisco BD, Balas EA, et al. Internet-enabled interactive multimedia asthma education program: A randomized trial. Pediatrics. 2003;111:503–510. [PubMed]
9. Lepofsky J, Nash S, Kaserman B, et al. I’m not a doctor but I play one on TV: E.R. and the place of contemporary health care in fixing crisis. Health & Place. 2006;12:180–194. [PubMed]
10. Gruneir A, Silver MJ, Rochon PA. Review: Emergency department use by older adults: A literature review of needs trends, appropriateness and consequences of unmet health care. Med Care Rs Rev. 2011;68:131–155. [PubMed]
11. Baker DW, Gazmararian JA, Sudano J, et al. The association between age and health literacy among elderly persons. J Gerontology. 2000;55B:S368–S374. [PubMed]
12. Nayak L, Erinieri JP. Audience response systems in medical student education benefit learner and presenters. Acad Radio. 2008;15:383–389. [PubMed]
13. MacGeorge EL, Homan SR, Dunning JB, et al. Student evaluation of audience response technology in large lecture classes. Education Tech Research Dev. 2008;56:125–145.
14. Hazzard WR. Capturing the power of academic medicine to enhance health and health care of the elderly in the USA. Geriat & Geront Internat. 2004;4:5–14.
15. Bernstein E, Goldfrank LR, Kellerman AL, et al. A public health approach to emergency medicine: Preparing for the twenty-first century. Acad Emerg Med. 1994;1:277–286. [PubMed]
16. Fan L, Shah MN, Veazie PJ, et al. Factors associated with emergency department use among the rural elderly. J.Rural Health. 2011;27:39–49. [PMC free article] [PubMed]
17. Hastings SN, Heflin MT. A systematic review of interventions to improve outcomes for elders discharged from the emergency department. Acad Emerg Med. 2005;12:978–986. [PubMed]
18. McCusker J, Cardin S, Bellavance F, et al. Return to the emergency department among elders: Patterns and predictors. Acad Emerg Med. 2000;7:249–259. [PubMed]
19. Ho MT, Eisenberg MS, Litwin PE, Schaefler SM, Damon SK. Delay between onset of chest pain and seeking medical care: The effect of public education. Am J Emerg Med. 1989;28:727–731. [PubMed]
20. Dong XQ, Ssimon MA. Enhancing national policy and programs to address elder abuse. J Am Med Assoc. 2011;305:2460–2461. [PubMed]
21. Baker DW, Wolf MS, Feinglass J, et al. Health literacy and mortality among elderly persons. Arch Intern Med. 2007;167:1503–1509. [PubMed]