| Author | Affiliation |
|---|---|
| Kellee T. James, PharmD | University of California San Francisco, Department of Clinical Pharmacy, San Francisco, California |
| Alissa Detz, MD | Robert Wood Johnson Foundation Clinical Scholar, University of California Los Angeles, Department of Medicine, Los Angeles, California |
| Zlatan Coralic, PharmD | University of California San Francisco, Department of Clinical Pharmacy, San Francisco, CaliforniaUniversity of California San Francisco, Department of Emergency Medicine, San Francisco, California |
| Hemal Kanzaria, MD | Robert Wood Johnson Foundation Clinical Scholar, University of California Los Angeles, Department of Medicine, Los Angeles, California |
A 40-year-old woman presented to the emergency department with a chief complaint of a painful rash. She had noticed lesions on her skin accompanied by burning pain that intensified over a 24-hour period. The patient admitted to smoking “crack” cocaine 4 days prior to presentation. She reported having similar symptoms previously. Her complicated past medical history was significant for hepatitis C, anti-phospholipid antibody syndrome, migraine headaches, and chronic lower back pain. She endorsed smoking cigarettes and polysubstance abuse (marijuana, heroin, and daily cocaine use). The patient’s exam was notable for retiform purpuric skin lesions with eschar on her left external pinnae (Figure 1), tongue, roof of her mouth, and bilaterally on her upper and lower extremities (Figure 2). Pus was expressible on palpation of the tibial skin lesions. Laboratory evaluation revealed a white blood cell count of 3.1×109 cells/L and a positive urine toxicology screen for cocaine. A biopsy obtained from her right thigh during a prior similar presentation showed luminally-thrombosed fibrin-containing small vessels surrounded by neutrophils and nuclear dust. The adjacent dermis contained extravasated erythrocytes.
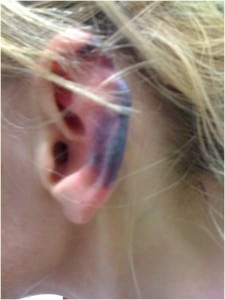
Retiform purpuric skin lesions with eschar on pinnae.
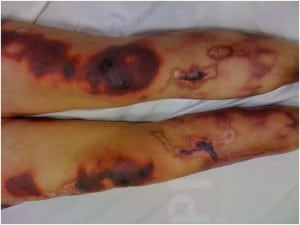
Retiform purpuric skin lesions with eschar on lower extremities.
A vasculitic syndrome associated with levamisole-adulterated cocaine has become increasingly recognized. This syndrome is characterized by purpuric lesions in a retiform pattern that may become necrotic and are commonly distributed on the ears, face, and extremities,1 as evidenced by our patient. Typical laboratory findings include agranulocytosis, leukocopenia, and the production of anti-neutrophil cytoplasmic antibodies.1 There is no evidence for the optimal treatment of levamisole-induced cutaneous vasculitis syndrome. Steroids have been used, but have an unclear benefit. 2 Permanent discontinuation of levamisole-adulterated cocaine use should be advocated. When appropriate, surgical debridement has been used to contain the progression of necrotic tissue spread.2
Footnotes
Address for Correspondence: Zlatan Coralic, PharmD. University of California San Francsico School of Pharmacy, 505 Parnassus Avenue, M39, San Francisco, CA 94122. Email: Zlatan.Coralic@ucsfmedctr.org.
Submission history: Revision received February 23, 2013; Accepted March 25, 2013
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1 Gross RL, Brucker J, Bahce-Altuntas A A novel cutaneous vasculitis syndrome induced by levamisole-contaminated cocaine. Clin Rheumatol. 2011; 30:1385-1392
2 Change A, Osterloh J, Thomas J Levimasole: A Dangerous Cocaine Adulterant. Nature. 2010; 88:408-411


