| Author | Affiliation |
|---|---|
| Malford T. Pillow, MD | Baylor College of Medicine, Section of Emergency Medicine, Houston, Texas |
| Adrienne Hughes, MD | Baylor College of Medicine, Section of Emergency Medicine, Houston, Texas |
CASE REPORT
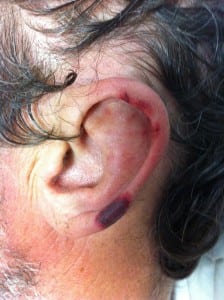
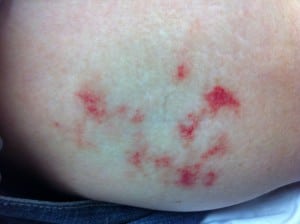
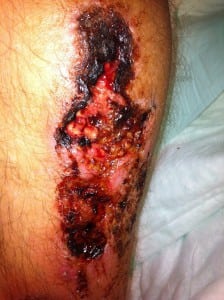
A 40-year-old man with Hepatitis C and a history of cocaine abuse presented with multiple stages of painful rashes on his extremities and ears. On examination, the patient had several areas of purpuric macules and retiform purpura to his legs and ears (Figures 1 and 2), as well as large ulcerations with erythematous borders on bilateral lower extremities (Figure 3). Laboratory studies revealed mild leukopenia (white blood cell 3.8 K/uL), positive anti-nuclear antibody (ANA), and negative cryoglobulins. Anti-myeloperoxidase antibodies (MPO-ANCA) and anti-proteinase-3 (PR3-ANCA) were also positive. Skin biopsy revealed dermal purpura and thrombi.
DISCUSSION
This patient presented with characteristic findings of levamisole-toxicity. Levamisole is not an inert substance but an antihelmithic drug and potent immunomodulator that was once used for treating cancer and certain autoimmune diseases.1–2 Levamisole is also an increasingly popular cocaine-adulterant3 linked to a growing number of cutanousvasculitis cases characterized by neutropenia or leukopenia, purpuric rash, and production of certain autoantibodies.4 It was these side effects that caused Levamisole to be withdrawn from the market in 2000. It is unknown why Levamisole has become an increasingly popular cocaine adulterant in the U.S. and Canada. It has been hypothesized that the cutting agent may intensify or prolong the stimulant properties of cocaine by its effects on the metabolism of monoamine neurotransmitters, specifically dopamine.5,6 Levamisole’s chemical properties also make detecting it in street purity tests difficult. Resolution of the cutaneous and hematologic effects often occurs spontaneously with discontinuation of the drug.
Footnotes
Supervising Section Editor: Sean O. Henderson, MD
Submission history: Submitted April 14, 2012; Revision received September 1, 2012; Accepted September 10, 2012
Full text available through open access at http://escholarship.org/uc/uciem_westjem
DOI: 10.5811/westjem.2012.9.12486
Address for Correspondence: Malford T. Pillow, MD. Baylor College of Medicine, Section of Emergency Medicine, 1504 Taub Loop, Mail Stop 25, Houston, TX 77004. Email: tysonpillow@gmail.com.
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Amery WK, Bruynsells JP. Levamisole, the story and the lessons. Int J Immunopharmacol.1992;14(3):481–486. [PubMed]
2. Tanphaichitr P, Tanphaichitr D, Sureeratanan J, et al. Treatment of nephrotic syndrome with levamisole. J Pediatr. 96:490–493. [PubMed]
3. Centers for Disease Control and Prevention (December 2009) Agranulocytosis associated with cocaine use – four States, March 2008–November 2009. MMWR Morb. Mortal. Wkly. Rep. 58:1381–1385. [PubMed]
4. Bradford M, Rosenberg B, Moreno J, et al. Bilateral necrosis of earlobes and cheeks: another complication of cocaine contaminated with levamisole. Ann Intern Med. 152(11):758–759.[PubMed]
5. Spector S, Munjal I, Schmidt DE. Effects of the immunostimulant levamisole, on opiate withdrawal and levels of endogenous opiate alkaloids and monoamine neurotransmitters in rat brain.Neuropsychopharmacoogy. 1998;19:417–427. [PubMed]
6. Chang A, Osterloh J, Thomas J. Levamisole: a dangerous new cocaine adulterant. Clin Pharmacol Ther. 2010;88:408–411. [PubMed]