| Author | Affiliation |
|---|---|
| Tara D. Dixon, MD | University of California, Irvine Medical Center, Department of Surgery |
| Darren J. Malinoski, MD | University of California, Irvine Medical Center, Department of Surgery |
INTRODUCTION
Perhaps one of the greatest achievements in medicine to date, organ transplantation has transformed the lives of thousands – bringing life to those who would surely have died without it. This achievement is dependent upon a generous gift from another person. From one deceased donor up to 55 lives may be saved or improved.1 With progressive advances in the trauma system, emergency physicians (EPs) are faced with more severely injured trauma patients, including the potentially brain-dead. The purpose of this three-part series is to present the components of determining brain death, to discuss the pathophysiology unique to brain-dead patients and to outline an algorithm based on that physiology to improve the care of the brain-dead patient. Rather than selectively neglect the brain-dead patient, active management while the patient is still in the emergency department (ED), specialty consultation and critical care can significantly enhance the likelihood of successful organ donation, turning a tragic loss into a rewarding patient encounter.
The majority of transplanted organs come from brain-dead or cadaveric donors. As most of these donors enter the healthcare system through the ED as either trauma patients with brain injuries or medical patients with acute intracranial hemorrhage, EPs are often involved in the diagnosis, referral, and initial stabilization of these patients. When these injuries would not benefit from neurosurgical or neurologic intervention and are deemed to be non-survivable, they are “devastating brain injuries.” The EP’s goal shifts to maintaining hemodynamic stability to diagnose brain death, should it occur. Furthermore, we must prepare the family for devastating news and allow them to begin the grieving process. EPs and trauma surgeons are often involved in discussions of end-of-life care and intensive care management of critical illness and injury. Therefore, both groups have the ability to impact organ donation, transplant frequency and success.
Organ Donation and Transplantation
Dr. Joseph Murray performed the world’s first transplant at Brigham and Women’s Hospital in 1954, and since then over 400,000 transplants have been performed.2 In 2007 there were 21,403 transplants performed in the United States (U.S.) alone.3 In medically suitable patients, transplantation for end-stage organ failure is the standard of care.4 The most commonly needed and transplanted organs, in descending order, are the kidney, liver, heart, lung, and pancreas. Kidney transplants made up 60% of all transplants in 2007 in the U.S. and have been shown to improve quality of life and to be cost-effective compared to hemodialysis.5
To comprehend the potential impact of organ donation, several statistics are relevant. The five-year survival rates for patients on the transplant waiting list compared to those that are transplanted are 80.3% vs. 91% for pancreas, 66.5% vs. 92% for kidney, and 37.7% vs. 48% for lung. Two-year survival rates for heart transplantation wait-listed patients range from 44–70%, depending on the severity of heart failure, while the five-year survival after heart transplantation is 73%. Similarly, the one-year survival rate for patients awaiting liver transplantation based on severity ranges from 0–60% and the five-year survival after liver transplantation is 73%. It has been estimated that an average of 30 life-years are saved per organ and tissue donor, based on 2002 statistics, and 55 life-years would be saved if all organs were maximally utilized.6 Despite this potential, there are currently 98,161 people on the United Network for Organ Sharing (UNOS) waiting list3, 77,758 patients went without transplant in 2007, and approximately 7,000 died waiting.7
There are several strategies to address the mismatch between available and needed organs. Education programs increase awareness of transplant needs and thereby increase the number of people who choose to donate, while prevention efforts lessen the burden of chronic diseases that require a transplant. Additionally, UNOS has an extended criteria donor program, which matches high-risk patients with advanced age or chronic diseases such as Hepatitis with high-risk donors. Expanding the donor pool from brain-dead donors to living donors and donors after cardiac death also helps to close the gap. Finally, this series of articles focuses on improving premortem care of brain-dead donors, which decreases the number who succumb to cardiovascular collapse, and increases the number and function of viable organs procured per donor.10
In the first part of this series, we examine the concept and definition of brain death and provide an overview of the organ donation process. We will outline the clinician’s role in determining brain death and introduce our Devastating Brain Injury Algorithm, Figure 1, which is the basis of this series.

BRAIN DEATH
The concept of brain death has caused great controversy in medicine and politics. It is debated by ethicists, law professors, government agencies and healthcare workers.8–11First introduced by Mollaret and Goulon in 1959, brain death was originally described as a persistent vegetative state or permanent coma.12 After 1959, the definition evolved until 1968 when a Harvard Medical School ad hoc committee created the current definition, which was later affirmed by the Uniform Determination of Death Act in 1981.12,13
In general, brain death is the irreversible loss of all brain function. Most agree that complex mental abilities alone do not singularly constitute being alive, lest those in a vegetative state or with severe cerebral malformations be inappropriately declared devoid of life.14 Ultimately, the brainstem controls brain function and is responsible for regulating breathing, heart rate, and reflexes such as gagging or coughing when the airway is obstructed, withdrawal from pain, and pupillary function. Without a functioning brainstem, life cannot exist. Therefore, diagnosing brain death requires the absence of brainstem function.
To establish a diagnosis of brain death, the clinician must first identify the underlying causes and determine that they are irreversible.12 Trauma, stroke, cerebral hypoxia, intracranial hemorrhage, tumors, meningitis, and encephalitis are all well-known causes.15 All confounding factors must be eliminated, such as hypothermia (< 35°C), hypoxia, intoxication by legal or illegal drugs, shock/hypotension, and severe electrolyte disturbances.12 Figure 2 shows the brain death declaration form and instruction sheet used at our institution.

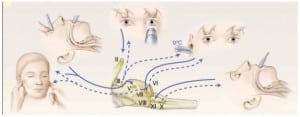
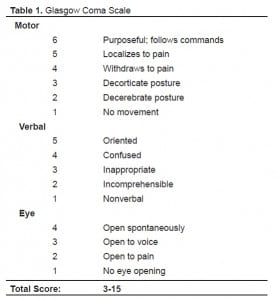
The clinical brain death assessment is usually made in the intensive care unit (ICU), but if delayed in the ED, patients may warrant a brain death exam before admission. This evaluation involves three steps: verifying unconsciousness, documenting absent brainstem reflexes, and performing the apnea test. To verify unconsciousness, a Glasgow score of 3 is required (Table 1). The five brainstem reflexes that should be assessed in adults are shown in Figure 3 and Table 2.12 If all brainstem reflexes are absent, an apnea test is performed. The patient should have a pCO2 within the normal range and be pre-oxygenated with 100% FiO2. The apnea test ensures the patient has lost the drive to breathe and confirms the diagnosis of brain death.

An overview of the procedure and an example of our institution’s brain death declaration protocol can be found in Table 3 and Figure 2, respectively. Criteria for a positive apnea test include: no attempt to breathe while disconnected from the ventilator (as oxygen is still delivered to the airway), a pCO2 greater than 60mmHg or a rise greater than 20mmHg above base-line, and an arterial pH less than 7.3. It usually takes 5–10 minutes of apnea for the pCO2 to meet criteria, and we recommend drawing blood gasses every three minutes reflexes, until either brain death is confirmed or the patient becomes hemodynamically unstable, at which point the patient should be reconnected to the ventilator. Some institutions recommend that the clinical exam, including the apnea test, be performed twice, six hours apart for adults and as much as 48 hours apart for neonates, but second assessment remains controversial.9,12

If the patient is hemodynamically unstable and would not tolerate even a few minutes off the ventilator for fear of causing cardiopulmonary arrest, other confirmatory tests may be used (Table 4). The most common in the U.S. is cerebral angiography. If the carotid arteries cut off at the base of the skull and there is no blood flow within the calvarium, the patient is brain dead. Recently, clinicians have used magnetic resonance or computed tomography angiograms in lieu of more invasive traditional angiography.16Electroencephalography (EEG) is well-validated and frequently used to confirm brain death with absent electrical activity. The disadvantage of EEG is that devices in the ICU may cause artifacts, leading to spurious results.12 Other tests include transcranial Doppler ultrasound to assess cerebral blood flow and nuclear imaging to assess uptake of tracer in the brain. The latter is preferred for secondary confirmation in our institution. None of these confirmatory tests replaces the clinical exam.
Since children are more resilient than adults, a longer time between assessments has been advocated.12 Additionally, many institutions require other confirmatory tests, in addition to the apnea test, in children less than one year of age. Deciding who is qualified to determine brain death is another variable. Some centers advocate that at least two clinicians concur on the diagnosis of brain death and that at least one of those clinicians be a neurologist or neurosurgeon. Beyond these minor differences, the declaration of brain death is otherwise similar worldwide.
Once declared brain dead, the patient may become an organ donor with family consent or advanced directive. This may be verified by living wills or, in some states, registration when obtaining a driver’s license.3 Brain death can be a challenging concept for a patient’s family, and it is important to equate brain death with the layperson’s understanding of bodily death, which usually means that the heart has stopped. The essential connection between brain function and conscious thought may not be obvious to laypersons, and should be stated explicitly.
It is imperative to separate end-of-life discussions surrounding brain death and the withdrawal of medical support from conversations about organ donation, to avoid any perceived conflict of interest. It is recommended that healthcare providers NOT approach family about organ donation without first consulting with their local organ procurement organization (OPO). In general, representatives from the OPO who are formally trained to talk with families about organ donation make the first, formal approach after end-of-life discussions have taken place. Healthcare providers with a close relationship to the family may be involved in the process as well.
Donor Management
The goal prior to and after the determination of brain death is to maintain perfusion of vital organs. This is, at times, as much the responsibility of the EP as the intensivist. After a family consents to donate organs, the OPO assumes care of the donor, both medically and financially, but physician involvement is still important to perform procedures and provide expert critical care advice. The brain is so central to bodily homeostasis, that once dead, it wreaks havoc on all other organ systems. Preserving organs is quite challenging in bythe face of brain death, and it is not uncommon to lose donors to the spiral of hormonal and cardiovascular collapse.
Recently, studies have proven that aggressive donor management (ADM) can improve the quantity and quality of donated organs from brain dead donors.4,17–19 After a dedicated team of physicians assumed responsibility for the management of all potential organ donors at the Los Angeles County/University of Southern California Medical Center, there was an 82% increase in the number of organ donors and a 71% increase in the number of organs recovered.4 Furthermore, organizing the care of the brain-dead donor into an evidence-based clinical protocol has been shown to both decrease donors lost to cardiovascular collapse, as well as increase the number of organs procured per brain-dead donor.17
The intensive care of the brain-dead donor does increase overall cost of care, but there is no cost to the donor’s estate or family.20 The cost-effectiveness of transplantation has been well established and has been most extensively reviewed for kidney transplantion.3,20–24Furthermore, it is imperative to remember that the care of the donor potentially benefits eight patients with end-stage organ failure, and many more who will benefit from tissue donation.6, 25 Traditionally, 75% of U.S. transplantations have been paid by Medicare.22The transplanted patient or the patient’s insurance company pay for the remaining 16% and 9%, respectively.22 Costs incurred while caring for the brain-dead donor are ultimately distributed amongst the patients receiving the donated organs and are usually covered through insurance or Medicare/Medicaid.26
CONCLUSION
The active participation of all healthcare providers involved in the care of patients with severe neurologic insults preserves the option of organ donation for patients and their families. This care often begins in the ED. Recently, our institution implemented a Devastating Brain Injury Pathway – an evidence-based protocol designed to improve care of this unique population. The primary purposes of the pathway are to maintain hemodynamic stability by providing comprehensive critical care in order for brain death to be diagnosed, should it occur; to give families time to come to the hospital and grieve; and to preserve the opportunity of donation for patients and their families. It is imperative to explicitly state that the primary purpose is not to improve the number of organs that can be transplanted, as this would represent a potential conflict of interest for the physician caring for the injured patient. However, the pathway does represent sound neurologic critical care that will improve perfusion to the brain and has the potential to turn a devastating brain injury into a salvageable one. If a patient does regress to brain death, organ perfusion will be maintained should the patient’s family decide to donate. In the next two reviews we will discuss the pathophysiology of brain death that causes so many donors to be lost to cardiovascular collapse (part 2) and the resuscitation and management of these donors to preserve the maximum amount and function of organs per donor (part 3).
Footnotes
Supervising Section Editor: Kurt R. Denninghoff, MD
Submission history: Submitted February 06, 2008; Revision Received November 07, 2008; Accepted November 09, 2008.
Full text available through open access at http://escholarship.org/uc/uciem_westjem
Address for Correspondence: Darren Malinoski, MD, Department of Surgery, University of California, Irvine, 333 The City Blvd West, The City Tower, Suite 705, Orange, CA 92868
Email: malinosd@uci.edu
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. Dr. Malinoski received honoraria for speaking and consulting from OneLegacy, Southern California’s non-profit organ procurement organization.
REFERENCES
1. United Network for Organ Sharing. Talking about transplantation: what every patient needs to know. 2004. Available at: http://www.unos.org.
2. Transplant pioneers recall medical milestone. Morning Edition, NPR. December 20. 2004. Available at: http://www.npr.org.
3. United Network for Organ Sharing. Dec 21, 2007. Available at: http://www.unos.org.
4. Salim A, Velmahos GC, Brown C, et al. Aggressive organ donor management significantly increases the number of organs available for transplantation. J Trauma.2005;58:991–994. [PubMed]
5. Smith CR, Woodward RS, Cohen DS, et al. Cadaveric versus living donor kidney transplantation: a medicare payment analysis. Transplant. 2000;69:311–314.
6. Schnitzler MA, Whiting JF, Brennan DC, et al. The life-years saved by a deceased organ donor. Am J of Transplant. 2005;5:2289–2296. [PubMed]
7. Novitzky D, Cooper DKC, Rosendale JA, et al. Hormonal therapy of the brain-dead donor: experimental and clinical studies. Transplant. 2006;82:1396–1401.
8. Hanto DW. Ethical challenges posed by the solicitation of deceased and living organ donors. NEJM. 2007;356:1062–1066. [PubMed]
9. Shemie SD, Pollack MM, Morioka M, et al. Forum. Lancet Neurol. 2007;6:87–92.[PubMed]
10. Sheehy E, Conrad SL, Brigham LE, et al. Estimating the number of potential organ donors in the United States. NEJM. 2003;349:667–674. [PubMed]
11. Capron AM. Brain death – well settled yet still unresolved. NEJM. 2001;344:1244–1246. [PubMed]
12. Wijdicks EFM. The diagnosis of brain death. NEJM. 2001;344:1215–1221. [PubMed]
13. Todd PM, Jerome RN, Jarquin-Valdivia AA. Organ preservation in a brain dead patient: information support for neurocritical care protocol development. J Med Libr Assoc. 2007;95:238–245. [PMC free article] [PubMed]
14. Bagheri A. Individual choice in the definition of death. J Med Ethics. 2007;33:146–149. [PMC free article] [PubMed]
15. Karcioglu O, Ayrik C, Erbil B. The brain-dead patient or a flower in the vase: the emergency department approach to the preservation of the organ donor. Eur J Emerg Med. 2003;10:52–57. [PubMed]
16. Young GB, Shemie SD, Doig CJ, et al. Brief review: the role of ancillary tests in the neurological determination of death. Can J Anesth. 2006;53:533–539. [PubMed]
17. Salim A, Martin M, Brown C, et al. The effect of aggressive donor management: implications for the national organ donor shortage. J Trauma. 2006;61:429–432.[PubMed]
18. Rosendale JD, Chabalewski FL, McBride MA, et al. Increased transplanted organs from the use of a standardized donor management protocol. Am J Transplant. 2002;2:761–768. [PubMed]
19. Roth BJ, Sher L, Murray JA, Belzberg H, Mateo R, Heeran A, Romero J, Mone T, Chan L, Selby R. Cadaveric organ donor recruitment at Los Angeles County Hospital: improvement after formation of a structured clinical, educational and administrative service. Clin Transplant. 2003;17(suppl9):52–57. [PubMed]
20. Donate Life America. December 26, 2007. Available at: http://www.donatelife.net.
21. Suthanthiran M, Strom TB. Renal transplantation. NEJM. 1994;331:365–376.[PubMed]
22. Evans RW, Kitzmann DJ. An economic analysis of kidney transplantation. Surg Clin N Amer. 1998;78:149–174. [PubMed]
23. Kim SJ, Gordon EJ, Powe NR. The economics and ethics of kidney transplantation: perspectives in 2006. Curr Opin Nephrol Hypertens. 2006;15:593–598. [PubMed]
24. Oostenbrink JB, Kok ET, Verheul RM. A comparative study of resource use and costs of renal, liver and heart transplantation. Transpl Internat. 2005;18:437–443.
25. Meier-Kriesche H, Schold JD, Gaston RS, et al. Kidneys from deceased donors: maximizing the value of a scarce resource. Am J Transpl. 2005;5:1725–1730.
26. United States Department of Health and Human Services January 8, 2008. Available at: http://answers.hrsa.gov via www.organdonor.gov.



