| Author | Affiliation |
|---|---|
| Manu Kaushik, MD | Creighton University Medical Center, Department of Internal Medicine, Omaha, NE |
| Ritu Madan, MD | Creighton University Medical Center, Department of Internal Medicine, Omaha, NE |
| Prateek K Gupta, MD | Creighton University Medical Center, Department Of Surgery, Omaha, NE |
| Janardan Gorthi, MD | Creighton University Medical Center, Department of Internal Medicine, Omaha, NE |
| Venkata M Alla, MD | Creighton University Medical Center, Department of Internal Medicine, Omaha, NE |
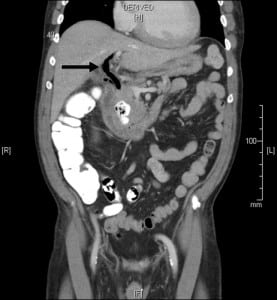
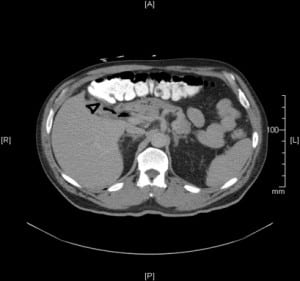
A 60-year-old male presented with self-limited transient right upper quadrant abdominal pain associated with dyspepsia of a few days duration. Examination revealed right upper quadrant tenderness with negative Murphy’s sign. Laboratory results showed abnormal ALT (129u/L), AST(165 u/l), total bilirubin (1.3mg/dl) and WBC count (12,800/microL). Ultrasound of the abdomen demonstrated gall bladder stones with thickened gall bladder, and his symptoms were attributed to cholecystitis. His pain exacerbated two days later. Total bilirubin rose to 3.1 mg/dl and alkaline phosphatase increased from normal to 257 u/L. However, this pain resolved spontaneously within a day with subsequent improvement of liver function tests. Patient simultaneously developed transient self-limited lower GI bleed. A computed tomography scan showed presence of pneumobilia (Figure 1) with a collapsed gallbladder closely apposed to transverse colon (Figure 2). The clinical condition of the patient continued to improve, supporting resolution of cholangitis. The patient later underwent a laparoscopic cholecystectomy and was identified to have cholecysto-colonic fistula that we presume decompressed the biliary system. This fistula was the most likely source of lower gastrointestinal bleed since a colonoscopy ruled out other causes. Cholecysto-intestinal fistulae are an unusual but established cause of gastrointestinal bleed.1 They often occur in association with Mirizzi’s syndrome and rarely may accompany gall bladder malignancy. Pneumobilia is usually considered an indicator of worsening cholangitis in a patient with deteriorating clinical condition. Nonetheless, physicians and surgeons should be aware that it could be a hallmark of fistulization of the biliary system into the gut in a clinically improving patient of cholecystitis or cholangitis.
Footnotes
Supervising Section Editor: Sean Henderson, MD
Submission history: Submitted January 16, 2010; Revision Received January 19, 2010; Accepted January 25, 2010
Full text available through open access at http://escholarship.org/uc/uciem_westjem
Address for Correspondence: Manu Kaushik, MD, Suite 5850, 601N. 30th Street, Omaha, NE- 68131
E-mail: drmanukaushik@gmail.com
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Kunasani R, Rastogi V, Boonswang P, et al. Cholecystocolonic fistula presenting as massive lower GI hemorrhage. Gastrointest Endosc. 2003;58(1):142–4. [PubMed]


