| Author | Affiliation |
|---|---|
| Kris Chiles, MD | University of California, Irvine School of Medicine, Department of Emergency Medicine, Orange, CA |
| Eric F. Silman, MD | University of California, San Francisco, Department of Emergency Medicine |
| Mark I. Langdorf, MD, MHPE | University of California, Irvine School of Medicine, Department of Emergency Medicine, Orange, CA |
| Shahram Lotfipour, MD, MPH | University of California, Irvine School of Medicine, Department of Emergency Medicine, Orange, CA |
A 56-year-old Hispanic male presented to the emergency department (ED) complaining of right lower quadrant abdominal pain for two days. The pain was gradual in onset with a throbbing, burning quality, and 10 out of 10 severity. He reported diarrhea but denied fever, chills, nausea or vomiting. In the ED the patient was afebrile with normal vital signs, and his abdomen was soft and mildly tender in the right lower quadrant with normal bowel sounds. Computed Tomography (CT) of the pelvis with oral and intravenous contrast showed a thickened cecal wall with radiographic findings consistent with appendicitis (Figure 1). The patient went to the operating room for laparoscopic appendectomy and was found to have right-sided colonic diverticulitis involving the cecum, as well as a normal appendix.
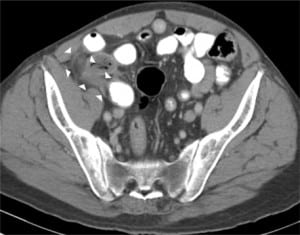
Right-sided colonic diverticulitis was first described in 1912 by Potier.1 Right-sided diverticulae are true, involving all layers of the intestinal wall, in contrast to left-sided which are false, only involving the mucosa and submucosa; however, the pathological mechanism that leads to diverticulitis is the same throughout the colon.2 In a majority of cases the underlying cause is secondary to obstruction by a faecolith.3 This pathologic mechanism mimics appendicitis and as such, the clinical presentation of right-sided diverticulitis is identical.4 Diverticulitis is initially managed non-operatively with antibiotics, unlike appendicitis which mandates surgical intervention. This difference underscores the importance of radiographic evidence along with a high index of suspicion for correctly identifying this uncommon diagnosis.
Despite its low incidence, right-sided colonic diverticulitis remains an important differential diagnosis to consider in the presentation of an older patient with acute right lower quadrant pain. CT for acute appendicitis is good but not perfect. A systematic review showed CT to be 94 percent sensitive and 95 percent specific.5 Therefore, correct radiographic diagnosis, coupled with astute clinical judgment, may avoid unnecessary laparotomy.
Footnotes
The authors wish to acknowledge Dr. Allen Cohen for his expertise and assistance in interpretation of the CT scan.
Supervising Section Editor: Michael Menchine MD, MPH
Submission history: Submitted April 09, 2008; Revision Received September 21, 2008; Accepted November 10, 2008
Full text available through open access at http://escholarship.org/uc/uciem_westjem
Address for Correspondence: Shahram Lotfipour, MD, MPH, Department of Emergency Medicine, University of California Irvine School of Medicine, 101 The City Drive, Rte 128-01 Orange, CA 92868
Email: SHL@uci.edu
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Potier F. Diverticulite et appendicite. Mem Soc Anat Paris. 1912;137:29–31.
2. Magness LJ, Sanfelippo PM, van Heerden JA, et al. Diverticular disease of the right colon. Surg Gynecol Obstet. 1975;140:30–32. [PubMed]
3. Henry FC. Acute diverticulitis of the cecum: Report of three cases diagnosed preoperatively as acute appendicitis. Ann Surg. 1949;129:109–18. [PMC free article][PubMed]
4. Junge K. Caecal Diverticulitis: A rare differential diagnosis for right-sided lower abdominal pain. Colorectal Disease. 2003;5:241–245. [PubMed]
5. Terasawa T, Blackmore C, Bent S, et al. Systematic Review: Computed Tomography and Ultrasonography to detect Acute Appendicitis in adults and adolescents. Ann Intern Med. 2004;141:537–46. [PubMed]


