| Author | Affiliation |
|---|---|
| Demis N. Lipe, MD | Carl R. Darnall Army Medical Center, Department of Emergency Medicine, Fort Hood, Texas |
| Randi Lindstrom, DO | Carl R. Darnall Army Medical Center, Department of Emergency Medicine, Fort Hood, Texas |
| Dustin Tauferner, DO | Carl R. Darnall Army Medical Center, Department of Emergency Medicine, Fort Hood, Texas |
| Christopher Mitchell, MD | Carl R. Darnall Army Medical Center, Department of Emergency Medicine, Fort Hood, Texas |
| Peter Moffett, MD | Carl R. Darnall Army Medical Center, Department of Emergency Medicine, Fort Hood, Texas |
Introduction
Methods
Results
Discussion
Limitations
Conclusion
ABSTRACT
Introduction
We compared the efficacy of Karl Storz CMAC Tip™ with inline suction to CMAC with traditional suction device in cadaveric models simulating difficult airways, using media mimicking pulmonary edema and vomit.
Methods
This was a prospective, cohort study in which we invited emergency medicine faculty and residents to participate. Each participant intubated 2 cadavers (one with simulated pulmonary edema and one with simulated vomit), using CMAC with inline suction and CMAC with traditional suction. Thirty emergency medicine providers performed 4 total intubations each in a crossover trial comparing the CMAC with inline suction and CMAC with traditional suction. Two intubations were performed with simulated vomit and two with simulated pulmonary edema. The primary outcome was time to successful intubation; and the secondary outcome was proportion of successful intubation.
Results
The median time to successful intubation using the CMAC with inline suction versus traditional suction in the pulmonary edema group was 29s and 30s respectively (p=0.54). In the vomit simulation, the median time to successful intubation was 40s using the CMAC with inline suction and 41s using the CMAC with traditional suction (p=0.70). There were no significant differences in time to successful intubation between the 2 devices. Similarly, the proportions of successful intubation were also not statistically significant between the 2 devices. The proportions of successful intubations using the inline suction were 96.7% and 73.3%, for the pulmonary edema and vomit groups, respectively. Additionally using the handheld suction device, the proportions for the pulmonary edema and vomit group were 100% and 66.7%, respectively.
Conclusion
CMAC with inline suction was no different than CMAC with traditional suction and was associated with no statistically significant differences in median time to intubation or proportion of successful intubations. [West J Emerg Med. 2014;15(4):548–553.]
INTRODUCTION
Emergency physicians (EP) manage most of the airways including difficult intubations that occur in emergency departments (ED).1,2 Endotracheal intubation can be difficult for many reasons, including limited time until oxygen desaturation and suboptimal views of the cords due to c-collars, blood, vomit and other secretions in the airway.3 Obscured airway secondary to secretions may require suctioning to adequately visualize the vocal cords and the endotracheal tube passing through the cords. EPs may already start with a suboptimal view of the airway, and first attempt failure increases potential complications for the patient.4
The CMAC inline suction device is a novel device (Karl Storz, El Segundo, CA) with a suction catheter attached to the tip. The inline suction device fits in a groove alongside the CMAC blade with the suction opening on the tip of the blade. The suction device is not adjustable once placed
Figure 1. Karl Storz CMAC inline suction device.
The CMAC laryngoscope is shaped like a traditional Macintosh laryngoscope blade and it also attaches directly to an LCD screen. This allows for direct laryngoscopy (DL) in addition to video laryngoscopy. We attempted to evaluate the new Storz inline suction device created for the CMAC device in cadavers with simulations of airway secretions of different viscosities representing pulmonary edema and vomit.
The primary objective of this study was to determine if the CMAC with inline suction was superior to the CMAC with traditional suction when comparing time to intubation. The secondary objective was to compare the proportion of successful intubations.
METHODS
This was a prospective, cohort study using the CMAC inline suction device versus CMAC with traditional handheld suction device in simulated cadaveric airways, complicated by simulation vomit or pulmonary edema. Vomit was simulated by placing 60 ml of cream of mushroom soup into the oropharynx of fresh frozen cadavers prior to start time. Pulmonary edema was simulated by placing baking soda in the oropharynx and then adding vinegar with red food coloring, just prior to starting the intubation attempt.
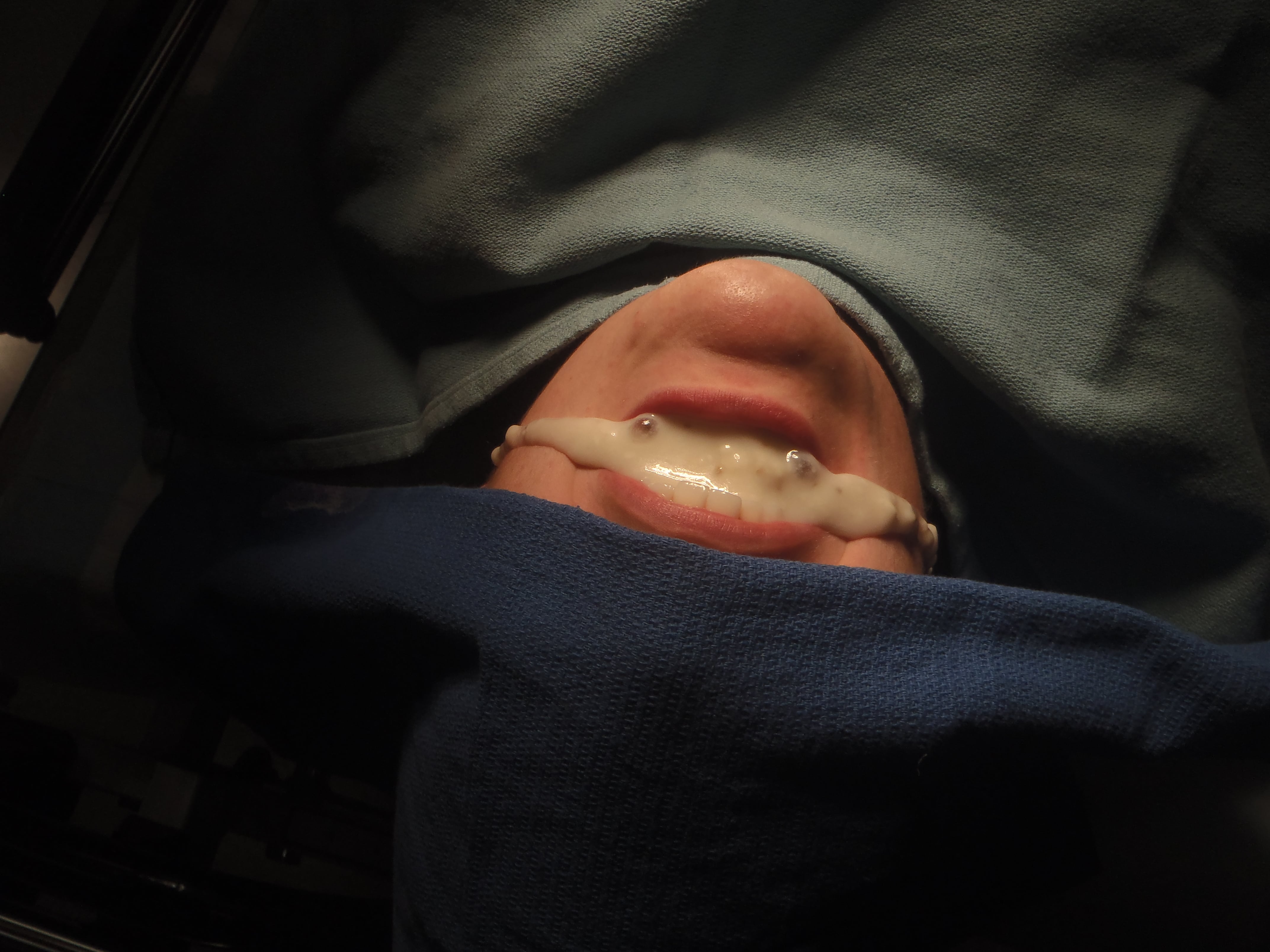
Figure 2. Vomit simulated fluid.
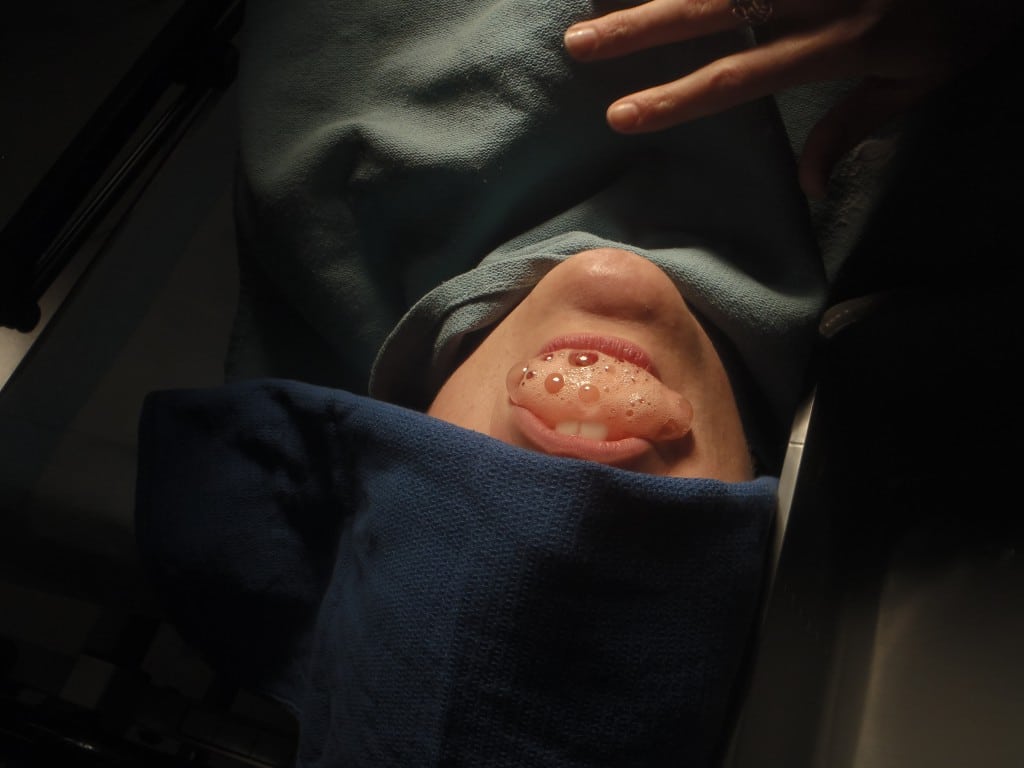
Figure 3. Pulmonary edema simulated fluid.
To simulate vomit, we used canned condensed cream of mushroom soup (Campbell’s, Camden NJ). The pulmonary edema simulation was done by adding 1 tablespoon of baking soda (Arm and Hammer, Church and Dwight Company, Princeton NJ) and mixing it with 10 ml of vinegar (Heinz, H.J. Heinz Company, Pittsburgh Pennsylvania) with 1 teaspoon of red food coloring (McCormick, McCormick & Company, Sparks Maryland). Mixing this just prior to the intubation attempt, allowed for a more realistic simulation as the bubbles of the reaction collected at the surface of the mix simulated a pink, frothy sputum. The simulated fluids have not been previously validated; however, they have face validity and were considered to be good training aids by the participants during informal feedback.
Thirty participants volunteered from 2 U.S. Army emergency medicine residency programs. The volunteers consisted of a combination of resident physicians (post-graduate year (PGY)1, PGY2, and PGY3 skill levels), as well as physician assistants and attending physicians. Intubations were attempted on 6 different fresh frozen cadavers. Equal number of participants started on each of the cadavers, and each participant endotracheally intubated 2 cadaver models. Participants were asked to intubate the cadavers using a 7.5 mm internal diameter cuffed endotracheal tube with a CMAC size 3 using the inline suction and with traditional handheld suction. The participants were given instruction on the handling of both the CMAC with inline suction and traditional handheld suction prior to the study. In both groups the suction catheters were connected to standard emergency medicine portable suction devices at maximal suction (for SSCOR Inc SCORT II Model 15006 this is approximately −525 mmHg).
We timed each participant for successful intubation, which was measured via stopwatch. Time was assessed beginning when tools were picked up from the table and stopped after the endotracheal (ET) tube cuff was inflated and stylette removed. Each participant was only allowed 1 attempted intubation per CMAC, suction, and vomit or edema combination. Successful intubation was confirmed with video and direct laryngoscopy by a single reviewer for each simulated substance. We recorded the number of successful versus unsuccessful intubations, in addition to time.
We excluded participants who were unsuccessful at intubation or placed the ET tube in the esophagus from our primary data because we were looking at overall time to successful intubation. However, as a secondary outcome we looked at the overall proportion of successful intubation for the inline versus traditional suction.
After breaking down the participants into skill groups, we performed a post-hoc analysis on both the primary and secondary outcomes Novice intubators were considered to be physician assistants, post-graduate level 1, and post graduate level 2 residents. Experienced intubators were considered to be post-graduate level 3 residents and attending physicians. This breakdown was considered appropriate in this data set since the data collection occurred toward the beginning of an academic year and therefore participants had only been in their year group for approximately 2 months.
The standard adjunct to assist endotracheal intubation has been traditional “wall mounted” suction, which can operate from −120 mmHg to −300 mmHg in our hospital. For this study, a portable suction device was used to replicate this handheld suction. Participants acted as their own controls in regards to their time to successful intubation with simulated vomit and pulmonary edema using the inline suction device versus their time to intubation with the handheld suction device. The subjects randomly selected 1 of the 4 simulations to start with so that approximately 1/4 of the subjects started on different simulations.
There were no prior studies to suggest a likely effect size, so we did not undertake a formal power analysis. The sample size was based on convenience and included all participants in a scheduled training event for residents. We described all time data with medians and interquartile ranges, and performed statistical analysis by comparing time to intubation using Mann-Whitney as the data was not parametrically distributed. We compared the proportions of successful intubation using Fischer’s Exact Chi Square. A p-value <0.05 was considered significant.
RESULTS
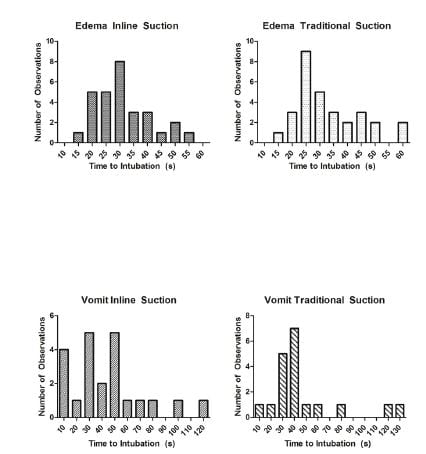
The data failed normality tests as they were non-parametrically distributed. The distributions suggest positive skew, but are equal within comparison groups (edema with inline suction versus edema with traditional suction; vomit with inline suction versus vomit with traditional suction) and therefore comparison is possible. Due to the non parametric distributions we presented the medians.
Figure 4. Frequency distribution of time to intubation for each simulated media and technique. Time to intubation is noted in 10 second intervals. “Inline Suction” refers to the CMAC with attached suction device and “Traditional Suction” refers to CMAC with detached standard suctioning.
The median time to successful intubation in the pulmonary edema simulation group using the CMAC with traditional suction was 30 seconds (s), while the median for inline suction was found to be 29s (p=0.54). Similarly, when comparing the CMAC with traditional suction in vomit simulation, the median time to successful intubation was 40s versus 41s with the inline suction (p=0.70). Neither result was statistically significant (Table).
The secondary outcome was overall proportion of successful intubation (Table). The simulated pulmonary edema group had an overall success rate of 100% with the handheld suction device, while the success rate with inline suction was 96.7%, (p=1.0). Success rates for the vomit simulation were 73.3% for inline suction and 66.7% with traditional suction (p=0.78).
Table. Time to intubation and intubation success rates with two different suction devices.
| Inline suction | Traditional suction | p-value* | |
|---|---|---|---|
| Time to intubation (s)† | |||
| Edema fluid | 29 (24–38) | 30 (25–41) | 0.54 |
| Novice‡ | 28 (23–44) | 27 (25–44) | 0.91 |
| Experienced§ | 29 (25–38) | 31( 26–40) | 0.57 |
| Vomit | 41 (23–52) | 40 (31–56) | 0.70 |
| Novice | 32 (11–45) | 40 (24–62) | 0.39 |
| Experienced | 49 (29–74) | 39 (31–60) | 0.82 |
| Intubation success (%)|| | |||
| Edema fluid | 96.7% | 100% | 1.0 |
| Novice | 100% | 92.3% | 1.0 |
| Experienced | 100% | 100% | n/a¶ |
| Vomit | 73.3% | 66.7% | 0.78 |
| Novice | 69.2% | 69.2% | 1.0 |
| Experienced | 76.4% | 64.7% | 0.71 |
*Time to intubation compared using Mann-Whitney-U. Intubation success compared using Fischer’s Exact Chi Square. †Median with interquartile range ‡Total (13), Physician assistant (1), Post graduate Level 1 (5), Post graduate level 2 (7) §Total (17), Post graduate level 3 (12), Attending (5) ||Proportion ¶No calculation possible with <5 observations per cell
As described previously, we conducted a post-hoc analysis of several subgroups. In both subgroups (novice and experience intubators) there were no statistically significant differences in either time to intubation or successful intubation (Table).
DISCUSSION
Overall, we found no statistical difference between the CMAC with inline suction and the CMAC with traditional suction when measuring time to intubation and proportion of successful intubations in a cadaveric model. Time to successful intubation and proportion of successful intubations are important measures in the ED. Multiple intubation attempts or a prolonged time to successful intubation are both associated with increased complications and adverse events. 5–7
Several studies have looked at managing difficult airway using the CMAC with inline suction or other similar devices.8–12 As Wadman et al8 reported, they found no significant difference in the success rates when comparing the CMAC inline suction device versus the CMAC with traditional suction. Their study however, did not check time to successful intubation and only included one type of airway secretion. Mitterlechner et al11,12 studied the effects of a suction laryngoscope that they created and compared the device to a regular Macintosh blade with traditional suction. They found no difference in time to intubation in a manikin study; however the success rate of orotracheal intubation was increased with the integrated suction laryngoscope. Other studies, such as the one conducted by Aziz et al13 compared the effectiveness of the CMAC video laryngoscope versus direct laryngoscopy in the setting of the predicted difficult airway. They found that there was an increase in first attempt success at intubation with the CMAC but the time to intubation was on average 13 seconds longer than traditional direct laryngoscopy. This study did not include any secretions; therefore, suction was not used.
Our current study was different in several regards. First, we used the Storz inline device, instead of making our own. The lumen of the inline suction had a predetermined size and could not be adjusted. All of the subjects performing the intubations were emergency medicine provides. We also used two mediums with different consistency as the simulated difficult airway. To our knowledge, the specific mediums had not been tested before. This allowed us to collect data on the performance of this new integrated suction device as sold commercially.
By using two different media we ensured a broader experience for our participants. While our simulated secretion models were not previously tested, they appeared to be consistent with secretions found in the ED. Informal feedback after the study suggested that these were good simulated models; however, formal evaluation of them was not performed. Future studies could formally investigate these novel models.
Our primary outcome was time to successful intubation. Overall, patients presenting to the ED that need to be intubated have a less desirable clinical condition when compared to those of the operating room environment. According to Taryle et al there was an increase in number of prolonged intubation attempts in their study of patients with acute respiratory failure in the ED versus the operating room.4 Their study looked at the complications of intubation in the ED and how those complications related to the survival of the patients. As mentioned, complications in a controlled operating room environment are usually limited to sore throat and soft tissue trauma that is considered minor. Complications of ED intubations include increased prolonged intubation attempts (>90 seconds) and aspiration among others. Since our study shows no difference in time to intubation when testing the two different suction models, this might potentially indicate that either method could be useful in the ED. Prior studies have reported time to successful intubation while using a CMAC or integrated suction ranging from 33 s to 52 s.11–13 Our results are similar to these previously reported times.
Our secondary outcome was proportion of successful intubations. Other studies have suggested that there was no statistical difference in overall success rate when comparing different intubating devices, including the CMAC.14–16 Emergency physicians would like to minimize the number of intubation attempts, especially in a difficult airway as multiple and prolonged attempts lends itself to increased complications for the patients, such as hypoxia, trauma of airway, aspiration and even cardiac arrest.4–7 Several studies have reported first attempt success rates from 82.2% to 87.3% for emergency physicians with several different intubating devices.16–20 While our simulated pulmonary edema success rate appears to be higher, our vomit medium success rates appear to be lower than the previously reported average. This is likely due to the addition of simulated media in our study making it difficult to directly compare successful intubation rates.
Although other studies have shown that level of training has an effect on first pass success, our analysis of the subgroups based on level of training did not show a statistical difference in success rates.20–22 It is possible that with an increase in subject size, a statistically significant difference may be discovered. And while there might be a possibility that the devices are equivalent, a non-inferiority design would be more useful to make this conclusion.
Overall, our results suggest no difference between the inline device and traditional suctioning when compared in 2 simulated media. This is in line with other studies that have studied various devices, but without the addition of simulated secretions.
LIMITATIONS
Our study has several limitations. As with all simulation studies, evaluating the performance of a technical skill in a controlled setting does not allow for variation in patients, preference of tools, or preparation. Therefore, generalizing results to real patients is difficult. Also given the environment of a simulation participants may have had less emphasis on proper technique; it is difficult to distinguish those who had a decreased level of skill from those who simply could not “suspend disbelief.” We do believe that each subject, however acted as their own control when comparing the 2 suction devices thus minimizing potential bias.
As this was a trial performed on fresh frozen cadavers, the tissue may have responded differently than live tissue and may not be generalized to clinical practice. In addition, the study was performed on a select number of cadavers with multiple intubation attempts. Even though cadavers were switched throughout the study, it is likely that repetitive trauma and distortion of the airway contributed to difficulty recognizing the airway and successful placement. Slight variations in the amount and consistency of the simulated secretions could also have affected time to successful intubation and we could not simulate continuous airway secretions as a clinical scenario may present.
The simulated vomit and pulmonary edema models have not been previously validated. Formal validation of these models may be possible in the future using direct surveying of experienced providers; however, informal feedback sessions during the study had overwhelming positive feedback on the realistic nature of the simulated fluids.
There were no prior studies to suggest an effect size, and so a power analysis was not completed. As such, it is difficult to know if the study was underpowered to detect a difference. The study included 60 intubations (30 intubations per group for each of the 2 simulated substances). It is possible a larger study would show a statistically significant difference between the two devices.
In regards to the video laryngoscopy using the CMAC device, while most resident physicians were novices to the device, some of the attending physicians might not have been. The exact number of those familiar with the CMAC with inline suction was not formally evaluated before the study. All subjects were given an orientation to the CMAC device before use. While we were evaluating the inline suction, a confounding factor to time to successful intubation would be the inexperience of operators with the CMAC device itself. Comparison of the 2 devices (inline suction versus traditional suction) might pose a bias if the operators are not equally trained or equally proficient.21,22
Finally, subjects randomly selected which simulation they wanted to start with. This may allow for learning; however with only one intubation attempt allowed per device per simulated media (4 total), the significance of this is likely limited. Randomization was not performed as it was felt that to truly randomize the subjects, randomization would have to be done for each attempt for each subject. If not, then subjects would simply start with a different simulation but proceed in the same order. As learning across 4 attempts seemed limited, and randomizing all steps added complication, it was not attempted.
CONCLUSION
This prospective, laboratory study suggests that the Karl Storz CMAC suction tip device and traditional means of suctioning are no different. Differences in times to successful intubations were not statistically significant and neither were proportion of successful intubations.
Footnotes
Full text available through open access at http://escholarship.org/uc/uciem_westjem
Address for Correspondence: Demis N. Lipe, MD. Department of Emergency Medicine, Carl. R. Darnall Army Medical, 36000 Darnall Loop, Fort Hood, TX 76544. Email: demis.ros@gmail.com. 7 / 2014; 15:548 – 553
Submission history: Revision received February 28, 2013; Accepted March 31, 2014
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The device used in this project was provided by C-MAC™, along with an unrestricted education grant. The device manufacturer had no role in study design, data analysis, preparation or review of the manuscript. The views expressed herein are solely those of the authors and do not represent the official views of the Department of Defense or Army Medical Department.
REFERENCES
1. Bair AE, Filbin MR, Kulkarin RG, et al. The failed intubation attempt in the emergency department: analysis of prevalence, rescue techniques and personnel. J of Emerg Med. 2002;23:131-140.
2. Walls RM, Brown CA, Bair AE, et al. Emergency airway management: a multi-center report of 8937 emergency department intubations. J of Emerg Med. 2011;41:347-354.
3. Fogg T, Annesley N, Hitos K, et al. Prospective observational study of the practice of endotracheal intubation in the emergency department of a tertiary hospital in Sydney, Australia. Emerg Med Australas. 2012; 24:617-624.
4. Taryle DA, Chandler JE, Good JT, et al. Emergency Room Intubations-Complications and Survival. Chest. 1979;75:541-543.
5. Hasegawa K, Shigemitsu K, Hagiwara Y, et al. Association between repeated intubation attempts and adverse events in emergency departments: An analysis of a multicenter prospective observational study. Ann Emerg Med. 2012;60:749-755.
6. Mort TC. Emergency tracheal intubation: complications associated with repeated laryngoscopic attempts. Anesth Analg. 2004;99:607-613.
7. Mort TC. Complications of emergency tracheal intubation: Immediate airway-related consequences: Part II. J Intensive Care Med. 2007;22:208-215.
8. Wadman M, Nicholas TA, Bernhagen BS, et al. A comparison of an integrated suction blade versus a traditional videolaryngoscope blade in the endotracheal intubation of a hemorrhagic cadaver model-a pilot study. Stud Health Technol Inform. 2012;173:534-536.
9. Nicholas TA, Pang H, Bernhagen MA, et al. Performance comparison of laryngoscopy and suction techniques in a hemorrhagic airway manikin simulator: direct laryngoscopy with yankauer vs storz CMAC with attached suction tip. Stud Health Technol Inform. 2012;173:307-309.
10. Boekeker BH, Bernhagen M, Miller D, et al. User preference comparing a conventional videolaryngoscope blade vs. a novel suction videolaryngoscope blade in simulated hemorrhagic airway intubation. Stud Health Technol Inform. 2012;173:72-74.
11. Mitterlechner T, Nerbl N, Herff H, et al. Effects of a suction laryngoscope in a model with simulated severe airway hemorrhage. Crit Care and Trauma. 2008;106:1505-1508.
12. Mitterlechner T, Maisch S, Wetsch WA, et al. A suction laryngoscope facilitates intubation for physicians with occasional emergency medical service experience-a manikin study with severe simulated airway haemorrhage. Resus. 2009;80:693-695.
13. Aziz MG, Dillman D, Fu R, et al. Comparative effectiveness of the C-MAC video laryngoscope versus direct laryngoscopy in the setting of the predicted difficult airway. Anesth. 2012;116:629-636.
14. Kilicasla A, Topal A, Tavlan A, et al. Effectiveness of the C-MAC video laryngoscope in the management of unexpected failed intubations. Rev Bras Anestesiol. 2014;64:62-65.
15. Nelson JG, Wewerka SS, Woster CM, et al. Evaluation of the Storz CMAC, Glidescope GVL, AirTraq, King LTS-D, and direct laryngoscope in a simulated difficult airway. American Journal of Emergency Medicine. 2013;31:589-592.
16. Mosier J, Chiu S, Patanwala AE, et al. A comparison of the GlideScope video laryngoscope to the C-MAC video laryngoscope for intubation in the emergency department. Ann Emerg Med. 2013;61:414-420.
17. Sagarin MJ, Barton ED, Chng YM, et al. Airway management by US and Canadian emergency medicine residents: a multicenter analysis of more than 6,000 endotracheal intubation attempts. Ann Emerg Med. 2005;46:328-336.
18. Sakles JC, Mosier J, Chiu S, et al. A comparison of the C-MAC video laryngoscope to the Macintosh direct laryngoscope for intubation in the emergency department. Ann Emerg Med. 2012;60:739-748.
19. Sackles JC, Laurin EG, Rantapaa AA, et al. Airway management in the emergency department: a one-year study of 610 trachel intubations. Ann Emerg Med. 1998;31:325-332.
20. Kim C, Kang HG, Lim TH, et al. What factors affect the success rate of the first attempt at endotracheal intubation in the emergency departments?. Emerg Med J. 2013;30:888-892.
21. Behringer EC, Kristensen MS Evidence for benefit vs novelty in new intubation equipment. Anaesthesia. 2011;66:57-64.
22. Bernhard M, Mohr S, Weigand MA, et al. Developing the skill of endotracheal intubation: implication for emergency medicine. Acta anaesthesiol Scand. 2012; 56:164-171.