| Author | Affiliation |
|---|---|
| Monica H. Swahn, PhD, MPH | Georgia State University, School of Public Health, Atlanta, Georgia |
| Robert M. Bossarte, PhD | University of Rochester, Department of Psychiatry, Rochester, New York Center of Excellence for Suicide Prevention, Department of Veterans Affairs, Canandaigua, New York |
| Jane B. Palmier, JD, MPH | Georgia State University, School of Public Health, Atlanta, Georgia |
| AuHuang Yao, MAhor | Georgia State University, School of Public Health, Atlanta, Georgia |
Introduction Methods Results Discussion
ABSTRACT
Introduction: A growing body of empirical research documents a significant co-occurrence of suicide attempts and interpersonal violence among youth. However, the potential role of early alcohol use initiation and current heavy alcohol use as correlates of this comorbidity has not been examined in a nationally representative sample of high school students.
Methods: We based our analyses on cross-sectional data from the 2009 Youth Risk Behavior Survey, which includes a nationally representative sample (n=16,410) of high school students in grades 9 through 12 in the United States. Multinomial logistic regression analyses were conducted to test the associations between measures of alcohol use (early alcohol use initiation and heavy drinking) and comorbid suicidal and violent behavior while controlling for potential confounders.
Results: Among high school students, 3.6% reported comorbid physical fighting and suicide attempt in the past year. Early alcohol use (prior to age 13) and heavy drinking (5 or more drinks in a row) were strongly associated with comorbid reports of physical fighting and suicide attempts (Adj. odds ratio [OR]=3.12; 95% confidence interval [CI]:2.49–3.89) and (Adj. OR=3.45; 95%CI:2.63–4.52).
Conclusion: These findings underscore the importance of both early alcohol use initiation and heavy drinking as statistically significant correlates of comorbid fighting and suicide attempts among youth. While future research is needed to determine the temporal ordering between problem drinking and violent or suicidal behaviors, existing prevention programs may benefit from including components aimed at reducing and delaying alcohol use.
INTRODUCTION
Recent research on adolescents suggests a strong link between violence involving other persons and self-directed violence.1–10 Previous studies have reported a comparatively high prevalence of comorbid self-directed and interpersonal violence among youth in the United States (U.S.) and in Africa.2–4,8,9,11–12While the overlap appears significant and of great concern to the general public health community, few studies have examined specific and potentially modifiable risk factors associated with co-occurring interpersonal and self-directed violence.
Early alcohol use initiation has been identified as a strong risk factor for a number of adverse health outcomes including self-directed and interpersonal violence.8,13–23 Recent research has documented that early alcohol use initiation is associated with both self-directed violence8,13,14,21–23 and interpersonal violence.8,17 However, there is a scarcity of research that has examined specific alcohol factors that may contribute to involvement in co-occurring violent and suicidal behaviors. The extent to which early alcohol use initiation is specifically associated with the overlap of self-directed and interpersonal violence has not been previously reported.
Reviews of prior research indicate that both suicidal and violent behaviors may share several characteristics associated with increased risk for both forms of violence.10 In particular, it is clear that aggressiveness, impulsivity, and correlates of poor mental health, such as substance abuse, depressive symptomology and hopelessness, can increase risk of both suicidal and violent behaviors.10,24,25Moreover, research also shows that youth who perform poorly in school have reported higher levels of suicidal ideation, interpersonal violence and substance use.26,27 However, there is little existing literature on the extent to which co-occurring violent and suicidal behavior actually share common risk factors identified with either suicidal behavior or interpersonal violence.11,12 Among youth, early alcohol use initiation is of particular importance because of the existing research linking early alcohol use to different forms of violence and evidence that early alcohol use may be reduced by existing prevention strategies.
The purpose of the current study is to examine early alcohol use initiation, prior to age 13, as a specific risk factor associated with co-occurring suicidal and violent behaviors among a nationally representative sample of boys and girls in the U.S. Other factors that have been associated with violence or suicidal behaviors, either empirically or theoretically, in earlier studies and that are available within the Youth Risk Behavior Survey were included as potential confounders (ie, sadness, low academic grades, binge drinking, weapon carrying, and drug use.1,10,27,28 The current study will determine the role of early alcohol use initiation in the comorbidity of self-directed and interpersonal violence and findings can be used to guide prevention and intervention programs.
METHODS
We based our analyses on data obtained from the 2009 national Youth Risk Behavior Survey (N=16,410). Students voluntarily completed the anonymous, self-administered questionnaire during a regular class period, following parental consent. Details of the study and the sampling strategy have been described elsewhere.29 Briefly, the survey employed a 3-stage cluster sample design to produce a nationally representative sample of students in grades 9–12. All regular public, Catholic, and other private school students, in grades 9 through 12, in the 50 States and the District of Columbia were included in the sampling frame. Puerto Rico, the trust territories, and the Virgin Islands were excluded from the frame. Moreover, schools were selected systematically with probability proportional to enrollment in grades 9 through 12 using a random start. The survey sampled 196 schools. In terms of the class selection, all classes in a required subject or all classes meeting during a particular period of the day, depending on the school, were included in the sampling frame. Systematic equal probability sampling with a random start was used to select classes from each school that participated in the survey. The overall response rate was 71% (school response rate 81% and student response rate 88%). Analyses of this complex multistage survey were conducted with the SAS 9.1 and SUDAAN 10.0 statistical software packages to accommodate the sampling design and to produce weighted estimates.
Risk factors included in multivariate analyses were based on previous research and incorporated measures of low academic grades, weapon carrying, sadness, binge drinking and other drug use. The specific wording of these questions and the prevalence for each measure are provided in Table 1. All variables included in the analyses were already dichotomized in the public domain dataset. However, early alcohol use initiation and the outcome variables were manually recoded as described below. Consistent with past research, we coded early alcohol use initiation as a three 3-level variable to include those initiating alcohol use prior to age 13, those who initiated alcohol use after age 13, and those who were not alcohol users.8,13,21,22 The outcome measure was based on the 2 questions that assessed any involvement in a suicide attempt or any involvement in physical fighting, both within the past 12 months. We combined the 2 measures to create a 4-level outcome variable to indicate involvement in both suicide attempts and physical fighting, involvement in physical fighting only, involvement in suicide attempts only, and involvement in neither suicide attempt nor physical fighting.

STATISTICAL ANALYSES
Weighted prevalence estimates for each of the risk factors are presented in Table 1. We conducted multinomial logistic regression analyses to determine the associations between early alcohol use initiation and suicide attempts and physical fighting, suicide attempt only, and physical fighting only relative to neither suicidal nor violent behaviors while controlling for the other potential confounders.
RESULTS
Overall, the prevalence of any physical fighting was 31.5%, and the prevalence of suicide attempt was 6.3% (Table 1). The prevalence of co-occurring physical fighting and suicide attempts was 3.6% (3.0% for boys and 4.2% for girls) in the national sample (Table 2). However, among early drinkers the prevalence of co-occurring physical fighting and suicide attempts was 9.4% (7.6% for boys and 11.5% for girls).
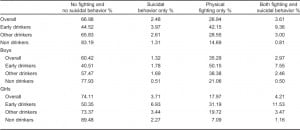
In the national sample, early drinking (Adj.odds ratio [OR]=5.42; 95% confidence interval [CI]: 3.36–4.17) was significantly associated with co-occurring physical fighting and suicide attempts (Table 3) relative to those who did not report early drinking and when controlling for possible confounders. Early drinking was associated with co-occurring physical fighting and suicide attempts for both boys (Adj.OR=4.17; 95% CI: 1.47–11.87) and girls (Adj.OR=6.50; 95% CI: 3.84–11.00) but appeared stronger for girls. For girls, initiating drinking later was also associated with co-occurring physical fighting and suicide attempts (Adj.OR=2.28; 95% CI: 1.26–4.11), but this association was not statistically significant among boys (Adj.OR=2.23; 95% CI: 0.81–6.17).
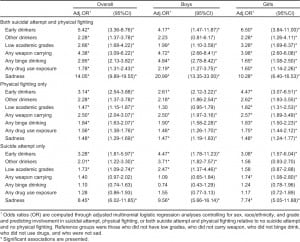
In terms of predicting physical fighting, early drinking (Adj.OR=3.14; 95% CI: 2.54–3.88) was significantly associated physical fighting only (Table 3) relative to those who did not report early drinking and this finding was observed for both boys and girls in stratified analyses. Similarly, in terms of predicting suicide attempt only, early drinking (Adj.OR=3.28; 95%CI: 1.81–5.97) was significantly associated suicide attempt only (Table 3) relative to those who did not report early drinking and this finding was observed for both boys and girls in stratified analyses.
DISCUSSION
The prevalence of involvement in both suicide attempts and physical fighting in this study was similar to reports from earlier studies of youth and suggest that the patterns and prevalence of co-occurrence remain similar over time and across populations of youth in different settings.8,11,30 Moreover, early alcohol use initiation, prior to age 13, was significantly associated with all levels of the outcome variable. However, the strongest associations were noted between early alcohol use initiation and co-occurring suicide attempt and physical fighting for girls (Adj. OR=6.50). The associations between early alcohol use initiation and co-occurring suicide attempt and physical fighting and also between early alcohol use initiation and with physical fighting appeared stronger for girls than for boys. This finding is intriguing and warrants further research of potential sex differences in early alcohol use and associated outcomes.
While many of the confounders examined were statistically significant especially for co-occurring suicide attempt and physical fighting, the patterns varied greatly for suicide attempt only. In fact, the fewest statistically significant associations were observed when examining correlates of suicide attempt alone. As has been noted previously and also found in the current study, there is a robust association between reports of sadness and co-occurring suicidal and violent behaviors.11,25,26 Consistent with earlier reports, we identified a strong association between sadness and co-occurring suicide attempt and physical fighting among both boys and girls. More importantly, while sadness was a significant correlate of all levels of the outcome, sadness had by far the strongest association with co-occurring suicide attempt and fighting. This was particularly noted among boys, where the association between sadness and co-occurring suicide attempt and physical fighting was remarkably high (Adj. OR=20.99).
Results from previous studies have found a strong link between suicidal behavior and violent behavior. In one study of school shootings in the U.S., for example, it was noted that the majority of perpetrators exhibited suicidal ideation or suicidal behavior prior to or during the violent attack.31 Perhaps more intriguingly, more than half of the perpetrators in these school shootings had no history of prior violence. It is clear that the link between suicidal and violent behavior is complex. Researchers have suggested that unrecognized or untreated suicidality may be highly prevalent among violent perpetrators.10 Future research on the predictors and correlates of suicidal behaviors among violent perpetrators is recommended, as is research into the link between suicidal behavior and violence at the population level.
LIMITATIONS
Several limitations of this study should be considered when interpreting the findings. First, the findings are based on high school students and therefore the findings do not reflect experiences of those who have dropped out of school. Second, the findings are based on self-reported data and have not been corroborated with other sources. Third, the findings are based on cross-sectional survey data, which do not permit determination of the temporal ordering of the risk factors relative to the outcome. Fourth, the assessment of co-occurring suicidal and violent behaviors only indicates the presence of both suicidal and violent behaviors within the past 12 months. Based on how the survey questions were asked, more specific timing of the presence of suicidal or violent behavior cannot be provided or inferred. Fifth, the survey is limited in the number and types of correlates that were examined, and it is possible that other potential confounders, if available, and included in the analyses, could have impacted our findings. Sixth, the confidence intervals for the odds ratios for some of the risk factors were relatively wide, indicating that some associations, while strong, were possibly unstable. Finally, it is possible that bias associated with social desirability may have contributed to an underreporting of high risk and violent behaviors.
Previous research has suggested that there is a significant overlap among both suicidal behavior and violent behaviors among youth.8,10,11 However, because of our relatively limited understanding of how different types of violent behavior overlap, efforts to design prevention programs that can address multiple types of violence, such as fighting and suicidal behaviors, have been limited.8,10 Findings from this study and others underscore how important it may be to develop programs that may be relevant across multiple forms of violent behaviors that span across self-directed and interpersonal violence.8,10,11 The current study is one of very few that seeks to better understand the potentially shared and modifiable risk factors between involvement in violent and suicidal behaviors.
In future studies of shared risk factors for co-occurring suicidal and violent behaviors, it is particularly important to assess modifiable factors that can be addressed by current evidence-based strategies and intervention. Meanwhile, the findings from our study indicate that early alcohol use initiation is an important predictor of suicidal and violent behaviors among both boys and girls. The specific mechanism linking suicidal and violent behavior is not well known nor is the role of early alcohol use initiation among these youth. Therefore, longitudinal research that can better assess the temporal ordering between early alcohol use initiation, suicidal and violent behavior is needed.
In terms of clinical practice and implications, these findings combined with earlier research calls for screening of early alcohol use initiation in pediatric populations prior to their teen years, by healthcare providers, because of the high incidence of alcohol use initiation among youth.8 However, prevention efforts are also needed to further delay the initiation of use and many of the associated adverse health linked to early alcohol use. Pediatricians as well as emergency physicians and other healthcare providers are in a unique and very important position to discuss alcohol use and its potential hazards with their pediatric patients and parents, particularly when patients are seen for injuries or risk for self-harm.32–34
Finally, based on the findings, it is clear that youth who report co-occurring suicidal and violent behaviors appear to experience a range of negative experiences including low academic grades, weapon carrying, binge drinking and drug use exposure that may further exacerbate the severity of their current health problems. While they are a small percentage of the youth population overall, they appear to be particularly vulnerable and in need of services.
Footnotes
Supervising Section Editor: Abigail Hankin, MD, MPH
Submission history: Submitted December 19, 2012; Revision received February 6, 2013; Accepted March 6, 2013
Full text available through open access at http://escholarship.org/uc/uciem_westjem
DOI: 10.5811/westjem.2013.3.15705
Address for Correspondence: Monica H. Swahn, Ph.D, MPH., Professor, School of Public Health, Partnership for Urban Health Research, Georgia State University, P.O. Box 3995, Atlanta, GA 30302. Email: MSwahn@gsu.edu.
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The preparation of this manuscript was partially supported by R01 CE001395 from the Centers for Disease Control and Prevention to Drs. Bossarte and Swahn. The authors disclosed no other potential sources of bias.
REFERENCES
1. Borowsky IW, Ireland M, Resnick MD. Adolescent suicide attempts: risks and protectors. Pediatrics.2001;107:485–93. [PubMed]
2. Bossarte RM, Simon TR, Swahn MH. Clustering of adolescent dating violence, peer violence and suicidal behavior. J Interper Violence. 2008;23(6):815–833. [PubMed]
3. Cleary SD. Adolescent victimization and associated suicidal and violent behaviors. Adolescence.2000;35(140):671–682. [PubMed]
4. Evans WP, Marte RM, Betts S. et al. Adolescent suicide risk and peer-related violent behaviors and victimization. J Interpers Violence. 2001;16(12):1330–1348.
5. Flannery DJ, Singer MI, Wester K. Violence exposure, psychological trauma, and suicide risk in a community sample of dangerously violent adolescents. J AmAcad Child Adolesc Psychiatry.2001;40(4):435–442. [PubMed]
6. Orpinas PK, Basen-Engquist K, Grunbaum JA. et al. The co-morbidity of violence-related behaviors with health-risk behaviors in a population of high school students. J Adolesc Health. 1995;16(3):216–225. [PubMed]
7. Silverman JG, Raj A, Mucci LA. et al. Dating violence against adolescent girls and associated substance use, unhealthy weight control, sexual risk behavior, pregnancy, and suicidality. JAMA.2001;286:572–579. [PubMed]
8. Swahn MH, Bossarte RM, Sullivent EE. Age of alcohol use initiation, suicidal behavior, and peer and dating violence victimization and perpetration among high-risk seventh-grade adolescents. Pediatrics.2008;121(2):297–305. [PubMed]
9. Swahn MH, Lubell KM, Simon TR. Suicide attempt and physical fighting among high school students – United States, 2001. MMWR Morb Mortal Wkly Rep. 2004;53(22):474–476. [PubMed]
10. Lubell KM, Vetter JB. Suicide and youth violence prevention: The promise of an integrated approach. Aggression and Violent Behavior. 2006;11(2):167–175.
11. Swahn MH, Gaylor E, ossarte RM. et al. Suicide Attempts and Physical Fighting: A Comparison between Urban, Suburban and Rural High School Students. Vulnerable Children & Youth Studies.2010;5(4):353–362.
12. Swahn MH, Bossarte RM., Musa Elimam D, Gaylor E, Jayaraman S. Prevalence and Correlates of Suicidal Ideation and Physical Fighting: A Comparison between Students in Botswana, Kenya, Uganda, Zambia, and the U.S.A. International Public Health Journal. 2010;2(2):195–205.
13. Bossarte RM, Swahn MH. The Associations between Early Alcohol Use and Suicide Attempts among Adolescents with a History of Major Depression. Addict Behav. 2011;36(5):532–535. [PubMed]
14. Cho H, Hallfors DD, Iritani BJ. Early initiation of substance use and subsequent risk factors related to suicide among urban high school students. Addict Behav. 2007;32(8):1628–1639. [PubMed]
15. Ellickson PL, Tucker JS, Klein DJ. Ten-year prospective study of public health problems associated with early drinking. Pediatrics. 2003;111:949–955. [PubMed]
16. Hingson R, Heeren T, Jamanka A. et al. Age of drinking onset and unintentional injury involvement after drinking. JAMA. 2000;284:1527–1533. [PubMed]
17. Hingson R, Heeren T, Zakocs R. Age of drinking onset and involvement in physical fights after drinking. Pediatrics. 2001;108:872–877. [PubMed]
18. Hingson R, Heeren T, Winter MR. et al. Early age of first drunkenness as a factor in college students’ unplanned and unprotected sex attributable to drinking. Pediatrics. 2003a;111:34–41. [PubMed]
19. Hingson R, Heeren T, Zakocs R. et al. Age of first intoxication, heavy drinking, driving after drinking and risk of unintentional injury among U.S. college students. J Stud Alcohol. 2003b;64:23–31.[PubMed]
20. Hingson RW, Heeren T, Winter MR. Age at drinking onset and alcohol dependence: age at onset, duration, and severity. Arch Pediatr Adolesc Med. 2006;160:739–746. [PubMed]
21. Swahn MH, Bossarte RM. Gender, early alcohol use, and suicide ideation and attempts: Findings from the 2005 Youth Risk Behavior Survey. J Adolesc Health. 2007;41(2):175–181. [PubMed]
22. Swahn MH, Bossarte RM, Ashby J. Early Alcohol Use and Suicide Attempts among Middle and High School Students: Findings from the 2006 Georgia Student Health Survey. Addict Behav.2010;35(5):452–8. et al. [PubMed]
23. Swahn MH, Bossarte RM, Choquet M. Substance Use Initiation and Suicide Ideation and Attempts among Students in France and the U.S. 2011 Apr 27. [Epub ahead of print] [PubMed]
24. Plutchik R. Outward and inward directed aggressiveness: The interaction between violence and suicidality. Pharmacopsychiatry. 1995;28(Suppl. 2):47–57. [PubMed]
25. Trezza GR, Popp SM. The substance user at risk of harm to self or others: Assessment and treatment issues. J Clin Psychol. 2000;56(9):1193–1205. [PubMed]
26. Eggert LL, Thompson EA, Herting JR. et al. Prevention research program: Reconnecting at-risk youth. Issues Ment Health Nurs. 2004;15(2):107–135. [PubMed]
27. US Department of Health and Human Services. Youth violence: A report of the surgeon general.Centers for Disease Control and Prevention, National Center for Injury Prevention and Control, Substance Abuse and Mental Health Services Administration, Center for Mental Health Services, National Institutes of Health, National Institute of Mental Health; 2001. Available at:http://www.surgeongeneral.gov/library/youthviolence/youvioreport.htm.
28. Department of Health and Human Services. The Surgeon General’s call to action to prevent suicide.Washington, DC: Department of Health and Human Services; 1999. Available at:http://www.surgeongeneral.gov/library/calltoaction/default.htm.
29. Centers for Disease Control and Prevention. Youth risk behavior surveillance – United States, 2007. Surveillance Summaries. MMWR Morb Mortal Wkly Rep. 2008;57(No. SS-4):1–136.
30. Eaton DK, Kann L, Kinchen S. et al. Centers for Disease Control and Prevention (CDC). Youth risk behavior surveillance – United States, 2007. MMWR Morb Mortal Wkly Rep. 2008;57(4):1–131.[PubMed]
31. Vossekuil B, Fein R, Reddy M. Final report and findings of the safe school initiative: Implications for the prevention of school attacks in the United States. Washington, DC: U.S. Department of Education, Office of Elementary and Secondary Education, Safe and Drug-Free Schools Program, and U.S. Secret Service, National Threat Assessment Center; 2002. Available at:http://www.secretservice.gov/ntac/ssi_final_report.pdf.
32. Kulig JW, American Academy of Pediatrics, Committee on Substance Abuse Tobacco, alcohol, and other drugs: the role of the pediatrician in prevention, identification, and management of substance abuse. Pediatrics. 2005;115(3):816–821. [PubMed]
33. American Academy of Pediatrics, Committee on Substance Abuse. Alcohol use and abuse: a pediatric concern. Pediatrics. 2001;108(1):185–189. [PubMed]
34. American College of Emergency Physicians. Clinical & Practice Management: Alcohol Screening in the Emergency Department. Approved April, 2011. Available at: http://www.acep.org/Clinical—Practice-Management/Alcohol-Screening-in-the-Emergency-Department/


