| Author | Affiliation |
|---|---|
| Adam Janicki, MD | Alpert Medical School of Brown University, Department of Emergency Medicine, Providence, Rhode Island |
| Otto Liebmann, MD | Alpert Medical School of Brown University, Department of Emergency Medicine, Providence, Rhode Island |
CASE
A 64-year-old woman presented to the emergency department after falling when she tripped on a rock while doing yard work. Physical examination revealed an open deformity of the left forearm (Figure 1). Radial pulse was palpable, sensation was intact, and she had normal range of motion of the fingers. While awaiting radiographs, bedside ultrasound was performed (Video).
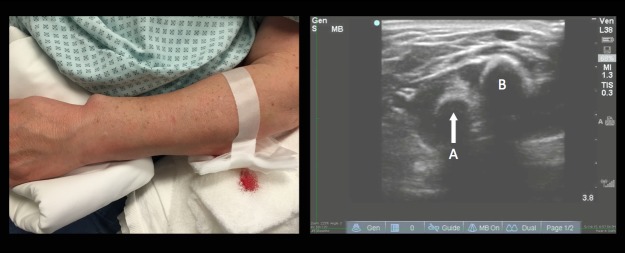
Ultrasound revealed intact radius and ulna and a large linear foreign body. The wooden foreign body was removed at the bedside (Figure 2) and patient was admitted for observation and intravenous antibiotics.
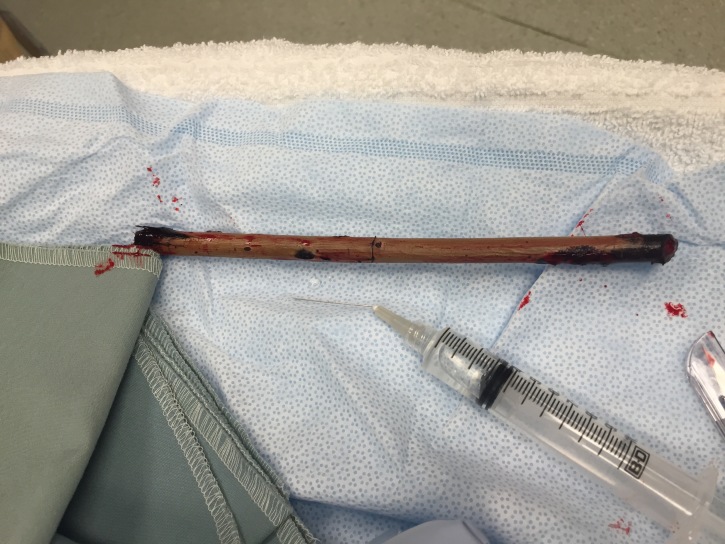
DISCUSSION
Wounds containing foreign bodies are at increased risk of delayed healing and infection. Wood, in particular, is extremely inflammatory and should be removed.1 Although radiopaque materials (metal, glass) are often visualized on plain radiography, radiolucent objects such as wood are often not.2 Sensitivity of plain films for the detection of wooden foreign bodies is estimated as low as 15%.3
The accuracy and availability of sonography make it an excellent modality for evaluation of foreign bodies.4 Sensitivity of ultrasound for the detection of foreign bodies is estimated between 50% to 100%, increasing when clinical information is available.5,6 The linear, high-frequency transducer is best for examining the superficial soft tissues. Most foreign bodies are hyperechoic with a surrounding hypoechoic area corresponding to granulation tissue, edema, or hemorrhage.7 Foreign body size estimation is often dependent on its orientation in relation to the ultrasound beam and can be affected by local tissue reaction.5 Multiple tissue planes may disguise a foreign body or give the appearance of one when none is there. Air can limit the penetration of ultrasound waves or itself masquerade as a foreign body.5
Literature supports ultrasound’s effectiveness in evaluating for fracture, and our case demonstrates the potential of emergency physician-performed ultrasound in the evaluation of all injured extremities.8,9
Footnotes
Section Editor: Sean O. Henderson, MD
Full text available through open access at http://escholarship.org/uc/uciem_westjem
Address for Correspondence: Adam Janicki, MD, Alpert Medical School of Brown University, 55 Claverick St., Providence, RI 02903. Email: adam_janicki@brown.edu. 1 / 2016; 17:61 – 62
Submission history: Revision received October 21, 2015; Accepted November 1, 2015
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Lammers RL. Chapter 49 Soft Tissue Foreign Bodies. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 7e. 2011. Available at: http://accessmedicine.mhmedical.com/content.aspx?bookid=348&Sectionid=40381513. Accessed Jun 23, 2015.
2. Dean AJ, Gronczewski CA, Costantino TG. Technique for emergency medicine bedside ultrasound identification of a radiolucent foreign body. J Emerg Med. 2003;24(3):303-8.
3. Anderson MA, Newmeyer WL, Kilgore ES. Diagnosis and treatment of retained foreign bodies in the hand. Am J Surg. 1982;144(1):63-7.
4. Borgohain B, Borgohain N, Handique A, et al. Case report and brief review of literature on sonographic detection of accidentally implanted wooden foreign body causing persistent sinus. Crit Ultrasound J. 2012;4(1):10.
5. Graham D. Ultrasound in the Emergency Department: Detection of Wooden Foreign Bodies in the Soft Tissues. J Emerg Med. 2002;22(1):75-9.
6. Crystal CS, Masneri DA, Hellums JS, et al. Bedside Ultrasound for the Detection of Soft Tissue Foreign Bodies: A Cadaveric Study. J Emerg Med. 2009;36(4):377-80.
7. Dumarey A, De Maeseneer M, Ernst C. Large wooden foreign body in the hand: recognition of occult fragments with ultrasound. Emerg Radiol. 2004;10(6):337-9.
8. Neri E, Barbi E, Rabach I, et al. Diagnostic accuracy of ultrasonography for hand bony fractures in paediatric patients. Arch Dis Child. 2014;99(12):1087-90.
9. Rabiner JE, Khine H, Avner JR, et al. Accuracy of point-of-care ultrasonography for diagnosis of elbow fractures in children. Ann Emerg Med. 2013;61(1):9-17.


