| Author | Affiliation |
|---|---|
| Matthew Hysell, MD | Spectrum Health-Lakeland, Department of Emergency Medicine, St. Joseph, Michigan |
| Jennifer Finch, MD | Holy Family Memorial Medical Center, Department of Emergency Medicine, Manitowoc, Wisconsin |
| David E. McClendon, MS | Michigan State University College of Osteopathic Medicine, Department of Emergency Medicine, East Lansing, Michigan |
ABSTRACT
Case Presentation
A 37-year-old man presented from jail reporting foreign body ingestion of a sprinkler head. While initial radiography did not reveal the foreign body, subsequent imaging with computed tomography demonstrated the sprinkler head. When confronted with this discrepancy the patient admitted to having the sprinkler head in his possession and choosing to swallow it after his initial radiography.
Discussion
This case demonstrates the importance of maintaining a high threshold for real illness in situations where there is suspected malingering, a situation not infrequently encountered in the emergency department.
CASE PRESENTATION
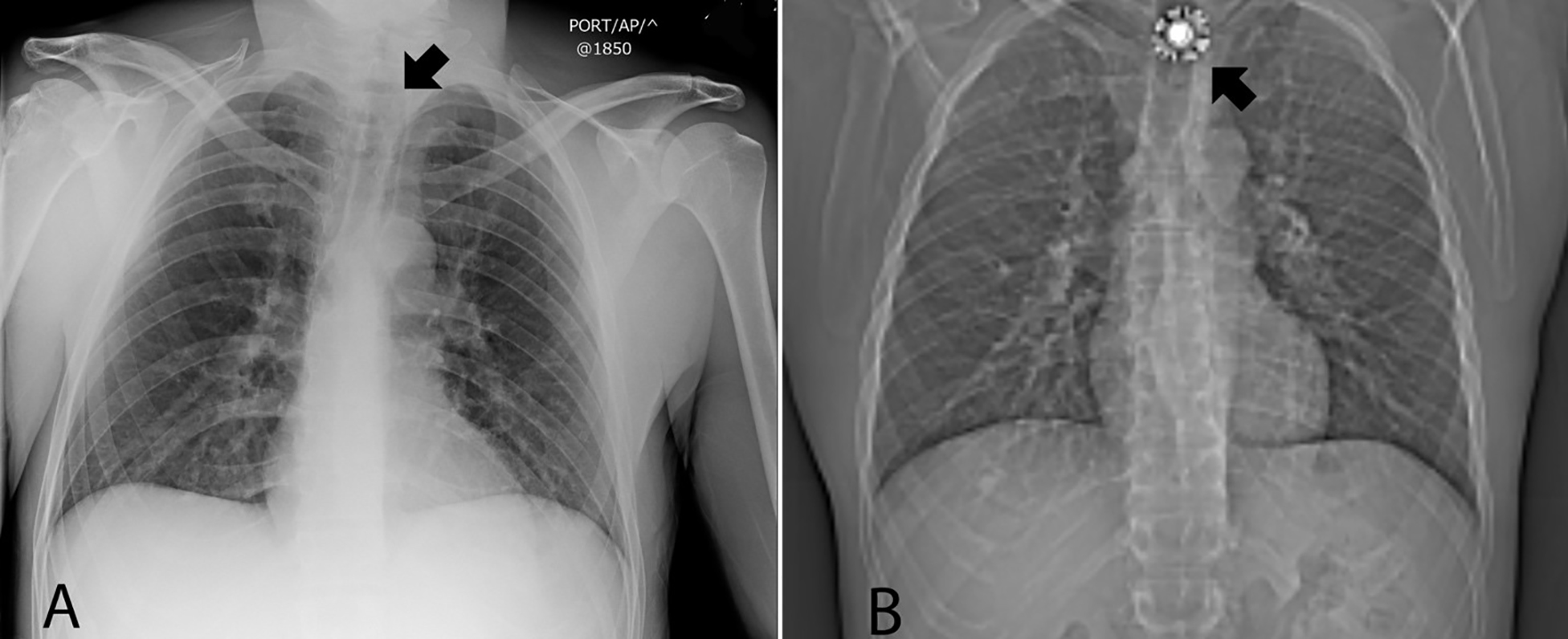
A 37-year-old man presented to the emergency department (ED) from jail reporting foreign body ingestion. The patient reported other prisoners had repeatedly punched him; guards informed him a provider would see him the following day. He then reported swallowing his jail cell’s sprinkler head, successfully triggering evaluation. Physical exam demonstrated periorbital ecchymosis. Head computed tomography (CT) revealed facial fractures. Chest radiograph was unremarkable (Image A). The negative chest radiograph was discussed with the patient, who vehemently insisted he had swallowed the sprinkler head and reported globus. Chest CT demonstrated a metallic foreign body in the upper esophagus (Image B) at a level visualized by radiography. The patient later admitted to possession of the sprinkler head through his course in the ED, ultimately swallowing it covertly after the radiograph. Endoscopic removal was successful.
DISCUSSION
Ingestion of foreign bodies by inmates and psychiatric patients is well documented.1,2 The delay in medical treatment following the patient’s assault offers a possible motive for his claim to have swallowed the foreign body. However, it was only after the patient arrived to the hospital and received medical care that he chose to swallow the sprinkler head. With negative initial testing it would have been easy for providers to have followed the actions of the villagers in “The Boy Who Cried Wolf” and to terminate further work-up. In this case the patient cried wolf so to speak, and then proceeded to release the wolf in the form of the sprinkler head ultimately demonstrated in the upper esophagus. While the patient’s rationale for the ingestion of the foreign body remains unclear, it is possible he wished to avoid return to jail where he had just been assaulted.3 This case demonstrates that maintaining a high threshold for real illness and listening to the patient, even in situations where malingering is suspected, is always necessary in the ED.
CPC-EM Capsule
What do we already know about this clinical entity?
The ingestion of foreign objects by inmates is well documented. Clinicians are also frequently faced with histories that may not be accurate.
What is the major impact of the image(s)?
First image demonstrates that initially provided history of foreign body ingestion was inaccurate. But upon subsequent imaging the foreign body was clearly visualized.
How might this improve emergency medicine practice?
This case demonstrates the importance of maintaining a high threshold for real illness even in situations where malingering is suspected or even demonstrated.
Footnotes
Section Editor: Rick A. McPheeters, DO
Full text available through open access at http://escholarship.org/uc/uciem_cpcem
The authors attest that their institution requires neither Institutional Review Board approval, nor patient consent for publication of this case report. Documentation on file.
Address for Correspondence: Matthew Hysell, MD, Spectrum Health-Lakeland, Department of Emergency Medicine, 1234 Napier Ave., St. Joseph, MI 49085. Email: mhysell@lakelandhealth.org. 4:283 – 284
Submission history: Revision received January 13, 2020; Submitted April 7, 2020; Accepted April 1, 2020
Conflicts of Interest: By the CPC-EM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Evans D. Intentional ingestions of foreign objects among prisoners: a review. World J Gastrointest Endosc. 2015;7(3):162.
2. O’Sullivan S, Reardon C, McGreal G, et al. Deliberate ingestion of foreign bodies by institutionalized psychiatric hospital patients and prison inmates. Ir J Med Sci. 1996;165(4):294-6.
3. Berry S. Deciphering when patients feign symptoms to avoid incarceration. JEMS. 2014;8(39):66.


