| Author | Affiliation |
|---|---|
| Katherine DeAmbrosis, MBBS | Department of Surgery, Ipswich Hospital, Ipswich, Queensland, Australia |
| Manjunath S. Subramanya, MBBS, MRCS | Department of Surgery, Ipswich Hospital, Ipswich, Queensland, Australia |
| Breda Memon, RGN, LLB, PGCEd | Department of Surgery, Ipswich Hospital, Ipswich, Queensland, Australia |
| Muhammed A. Memon, MBBS, MA, DCH | Department of Surgery, Ipswich Hospital, Ipswich, Queensland, Australia |
ABSTRACT
Traumatic duodenal hematoma is a rare condition that is encountered in the paediatric age group following blunt abdominal trauma. It poses both a diagnostic and therapeutic challenge. The main concern is increased morbidity secondary to delayed diagnosis and associated occult injuries to the adjacent structures. Most of these hematomas resolve spontaneously with conservative management, and the prognosis is good. We present a case of a 15-year-old boy who had a delayed presentation of duodenal hematoma and acute pancreatitis, which was treated conservatively with complete resolution.
INTRODUCTION
Intramural hematoma is a rare duodenal injury, usually occurring in association with blunt abdominal trauma. It can result in partial or complete high intestinal obstruction often with a slow insidious onset leading to delay in diagnosis. Diagnosis and treatment remain controversial. We present a case of delayed onset of such an injury complicated by acute pancreatitis in a 15-year-old boy wearing a seat belt in a high speed motor vehicle accident.
CASE REPORT
A 15-year-old male re-presented to the emergency department (ED) four days after involvement as a restrained rear seat, driver-side passenger in a front-on collision at 60 km per hour. In the absence of demonstrable external injury or clinical signs of trauma, the patient was discharged home from the ED following six hours of stable observation. Over the subsequent four days, he developed increasing abdominal distension and pain, with hematemesis developing in the hours preceding his second presentation to hospital.
On examination the patient was hypovolaemic with persistent tachycardia. He had a tense, distended abdomen with a paucity of bowel sounds. An urgent oral and intravenous (IV) contrast computed tomography (CT) of the abdomen demonstrated significant duodenal hematoma with no evidence of acute extravasation of oral contrast. The hematoma was associated with a degree of gastric outlet obstruction with minimal contrast observed in the small bowel. To further investigate the level and degree of gastric outlet obstruction, an oral Gastrogaffin meal study was performed six hour later, which showed complete gastric outlet obstruction (Figure 1).
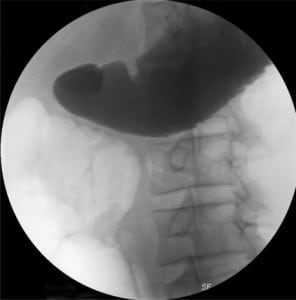
Based on the combination of clinical and radiological findings, the patient was managed conservatively with a nasogastric tube (free drainage and four hourly aspirations) and total parenteral nutrition. The patient initially displayed high daily nasogastric outputs (∼1500 ml), but this started decreasing gradually over the subsequent two-week period. A few days after admission, the patient developed sudden elevation of serum lipase levels raising the suspicion of delayed manifestation of pancreatic injury. A repeat contrast enhanced CT of the abdomen excluded any such injury. The lipase levels normalized over the subsequent 72 hours and the patient continued to improve. A repeat Gastrogaffin meal on day 18 post injury revealed residual narrowing of the lumen of the second and third part of the duodenum but complete resolution of the gastric outlet obstruction (Figure 2). Based on these findings, the patient was given clear fluids, then advanced to a full diet soon thereafter. The patient was discharged from the hospital without sequelae 22 days later.
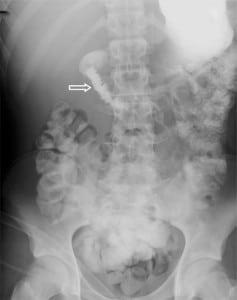
DISCUSSION
Intestinal hematoma following blunt abdominal trauma is a rare condition most commonly affecting the duodenum followed by the jejunum and colon.1 Shearing forces may lead to bleeding from small vessels either within the intestinal wall or from the surrounding structures. Therefore, the hematoma can occur either between the intestinal layers (i.e. in the submucosal or subserosal layers) or in the retroperitoneum, causing extrinsic pressure. Blunt abdominal trauma accounts for approximately 60% of the cases of the paediatric duodenal hematoma.2–3
Motor vehicle accidents and direct blows to the epigastrium and right upper quadrant are the usual mechanisms of injury. The duodenum is compressed against the lumbar spine resulting in contusion and hematoma and, ultimately, luminal obstruction. The retroperitoneal fixation of the duodenum, closely associated vascular pedicles, poorly developed abdominal wall musculature, and the wide costal angle in children contribute significantly to this type of injury.2–4 Other causes of intestinal hematomas include coagulation defects, penetrating abdominal injury and iatrogenic causes such as anticoagulation therapy and endoscopic duodenal biopsy.6–9 Pancreatitis is associated late sequelae due to the close anatomical duodenopancreatic relationship; one review of such injuries estimated an incidence of 21%.9
Intramural duodenal hematoma can be suspected from signs and symptoms of high intestinal obstruction following a clear history of blunt abdominal trauma. The preferred imaging tool is a dual (i.e. oral and IV) contrast-enhanced CT especially in the acute setting as it provides global information on all the structures surrounding the duodenum.10 In the absence of CT, a barium meal study can provide quick information regarding the level and type of intestinal obstruction (complete v.s. partial). Felson and Levin11 first described the appearance of intramural hematoma on barium study as “coiled spring” resulting from crowding of circular mucosal folds. Others have described a “picket fence sign” because of disappearance of the circular folds of the duodenum with mucosal pinching and spiculation occurring perpendicular to lumen. Both of these signs occur in a minority of cases and are considered non-specific. In our case the combination of CT and barium meal provided a satisfactory diagnosis.
The other modalities of diagnosis include magnetic resonance imaging (MRI), ultrasound and endoscopic studies. MRI demonstrates a characteristic “concentric ring sign” produced by hematoma surrounded by hemosiderin deposit and fluid.12 This is best seen on T1 weighted images two to three weeks after injury and is a tissue-specific MR feature.12 Given the delayed appearance of this finding, MRI has limited use in diagnosing duodenal injury in the acute setting.
Management of intramural duodenal hematoma is a challenging task and depends on the condition of the patient and the associated injuries. Operative management was the gold standard for such an injury until 1964. Since then conservative management has proven to be a successful and safe alternative in the absence of any life-threatening injuries.
Nasogastric decompression and total parenteral nutrition can be safely employed for up to three weeks after which the patient is re-evaluated.3–13 Coagulopathic states should be excluded and close monitoring maintained for any evidence of delayed pancreatic injury or inflammation.5,7 A possible late sequelae of conservative management is intestinal fibrosis, which may require surgery.1 Our patient was successfully managed along these lines with complete resolution of his condition. A repeat barium study showed slight residual narrowing of his duodenum, which we hope will resolve in time.
Surgical exploration for duodenal hematoma in the absence of any other life-threatening injuries to the surrounding organs is reserved for selected cases including those who demonstrate no clinical signs of improvement despite conservative therapy for approximately three weeks.14 If there is no improvement, laparotomy may be required to rule out other causes of duodenal obstruction,such as duodenal perforation or injury to the head of the pancreas.3
The most common and simple surgical approach is primary drainage of hematoma. However, complex duodenal injuries may require diversion to allow healing of the duodenal repair and prevent complications. Such repairs involve pyloric exclusion and gastrojejunostomy, omental patch and feeding jejunostomy. These procedures may result in complications such as duodenal fistulae formation (2%–14%), anastomotic leaks and hematoma reformation, which may necessitate further surgical intervention.14,15 These patients can be fed immediately post operatively through a feeding jejunostomy tube that allows for earlier discontinuation of parental nutritional support.5There are no documented late sequelae of surgical intervention for isolated duodenal hematomas.15
CONCLUSION
In the pediatric age group, duodenal injury from a blunt abdominal trauma resulting in an intramural hematoma is rare. This case illustrates the characteristic delayed presentation of a duodenal hematoma following a blunt injury from a motor vehicle accident and the associated sequelae of delayed pancreatitis. Total parenteral nutrition and gastric decompression provide an effective conservative treatment of the gastric outlet obstruction associated with this injury. Surgical intervention is only reserved for those patients who continue to show the clinical and radiological signs of complete high obstruction despite conservative management for three weeks.
Footnotes
Supervising Section Editor: Sean Henderson, MD
Submission History: Submitted April 10, 2010; Revision received June 30, 2010; Accepted October 11, 2010
Reprints available through open access at http://scholarship.org/uc/uciem_westjem
Address for Correspondence: Muhammed A. Memon, FRACS, Ground Floor, 8 Gordon Street, Ipswich,Queensland 4305, Australia
Email: mmemon@yahoo.com
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Czyrko C, Weltz CR, Markowitz RI, et al. Blunt abdominal trauma resulting in intestinal obstruction: when to operate? J Trauma. 1990;30:1567–71. [PubMed]
2. Weigelt JA. Duodenal injuries. Surg Clin North Am. 1990;70:529–39. [PubMed]
3. Degiannis E, Boffard K. Duodenal Injuries. Br J Surg. 2000;87:1473–9. [PubMed]
4. Voss M, Bass DH. Traumatic duodenal haematoma in children. Injury. 1994;25:227–30. [PubMed]
5. Ikeda T, Koshinaga T, Inoue M, Goto H, et al. Traumatic intramural hematoma of duodenum with thrombasthenia in childhood. Pediatr Int. 2007;49:668–71. [PubMed]
6. Shilyansky J, Pearl RH, Kreller M, et al. Diagnosis and management of duodenal injuries in children. J Pediatr Surg. 1997;32:880–6. [PubMed]
7. Polat C, Dervisoglu A, Guven H, et al. Anticoagulant-induced intramural intestinal hematoma. Am J Emerg Med. 2003;2:208–11. [PubMed]
8. Borsaru AD, Nandurkar D. Intramural duodenal haematoma presenting as a complication after endoscopic biopsy. Australas Radiol. 2007;51:378–80. [PubMed]
9. Jewett TC, Jr, Caldarola V, Karp MP, et al. Intramural haematoma of the duodenum. Arch Surg.1988;123:54–8. [PubMed]
10. Allen GS, Moore FA, Cox CS, Jr, et al. Delayed diagnosis of blunt duodenal injury: an avoidable complication. J Am Coll Surg. 1998;187:393–9. [PubMed]
11. Felson B, Levin EJ. Intramural hematoma of the duodenum: a diagnostic roentgen sign.Radiology. 1954;63:823–31. [PubMed]
12. Hahn PF, Saini S, Stark DD, et al. Intraabdominal haematoma: the concentric-ring Sign in MR.AJR. 1987;148:115–9. [PubMed]
13. Rickard MJ, Brohi K, Bautz PC. Pancreatic and duodenal injuries: keep it simple. ANZ J Surg.2005;75:581–6. [PubMed]
14. Fang JF, Chen RJ, Lin BC. Surgical treatment and outcome after delayed diagnosis of blunt duodenal injury. Eur J Surg. 1999;165:133–9. [PubMed]
15. Xeropotamos NS, Tsakayannis DE, Kappas AM. Intramural post-traumatic haematomas of the duodenum: are there any late sequelae of operative intervention? Injury. 1997;28:349–52.[PubMed]


