| Author | Affiliation |
|---|---|
| Annie Quysner, MD | Christus Spohn Texas A&M Emergency Medicine Residency Program |
| Salim Surani, MD, MPH | Christus Spohn Texas A&M Emergency Medicine Residency Program |
| Daniel Roberts, MD | Christus Spohn Texas A&M Emergency Medicine Residency Program |
A 45-year-old male with a one-month history of dyspnea and cough presented with productive sputum consisting of bronchial casts for several days prior to admission. Chest computed tomography showed bilateral opacifications (Figure 1). Several casts were expectorated daily (Figure 2). Pulmonary function tests revealed moderate restrictive lung disease. Bronchoscopy showed evidence of a cast in the right lung. Cast pathology and bronchial washings revealed no evidence of atypical cells or fungi, few inflammatory cells and a predominance of fibrin. No microorganisms were found. The patient was treated with antibiotics, as well as nebulized N-acetyl cysteine, with improvement in cast expectoration. The patient was asymptomatic at his two-week follow up. Repeat chest radiograph and pulmonary function tests were normal. The patient was diagnosed with plastic bronchitis.
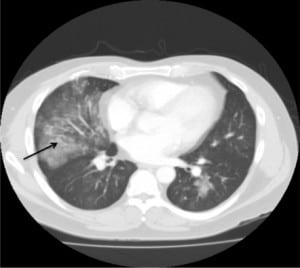
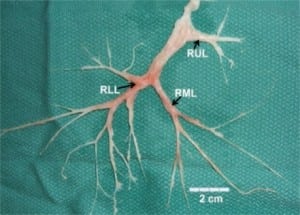
The underlying pathology of plastic bronchitis is not well understood. It is characterized by the presence of large, thick, mucofibrinous plugs filling the broncho-pulmonary tree, leading to severe respiratory distress.1,2 While commonly seen among children, few cases have been described among adults. It usually occurs in patients with inflammatory conditions, where the casts are fibrinous with eosinophilic material, or acellular cast composed mainly of mucin with little fibrin and no inflammatory cells, except for occasional mononuclear cells, as seen in patients with cardiovascular disease.3,4 Plastic bronchitis has been seen in several conditions, such as asthma, allergic bronchopulmonary aspergillosis, cystic fibrosis, smoke inhalation, after Fontans operation, H1N1 infection and idiopathic.4,5
Footnotes
Supervising Section Editor: Sean Henderson, MD
Submission history: Submitted September 4, 2010; Revision received September 28, 2010; Accepted October 11, 2010
Reprints available through open access at http://escholarship.org/uc/uciem_westjem
Address for Correspondence: Salim Surani, MD, 613 Elizabeth Street, Suite 813, Corpus Christi, Texas 78404
Email: srsurani@hotmail.com
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Park JY, Elshami AA, Kang DS, et al. Plastic Bronchitis. Eur Resp J. 1996;9:612–4.
2. Preciado D, Verghese S, Choi S. Aggressive bronchoscopic management of plastic bronchitis. Int J of Pediatric Otolaryngology 2010. 74:820–2.
3. Seear M, Hui H, Magee F, et al. Brobchial casts in children a proposed classification based on nine cases and a review of the literature. Am J Resp Crit Care Med. 1997;155:364–70. [PubMed]
4. Castello J, Steinhorn D, McColley S, et al. Treatment of plastic bronchitis in a Fontan patient with tissue plasminogen activator. A case report and review of the literature. Pediatrics. 2002;109(4):1–3. [PubMed]
5. Terano C, Miura M, Fukuzawa R, et al. Three children with plastic bronchitis associated with 2009 H1N1 influenza virus infection. Pediatr infect Dis J. 2010 Aug 3; (Epub ahead of print).www.ncbi.nlm.gov/pubmed.


