| Author | Affiliation |
|---|---|
| Justin Hamilton, MD | Madigan Army Medical Center, Department of Emergency Medicine, Tacoma, Washington |
| Matthew Mossanen, MD | University of Washington Medical Center, Department of Urology, Seattle, Washington |
| Jared Strote, MD, MS | University of Washington Medical Center, Department of Emergency Medicine, Seattle, Washington |
A 36-year-old male presented to the emergency department (ED) complaining of “lumps in my penis.” The patient described 2 firm, raised areas on the dorsum of his penis that had been present 1 week. He had no pain at rest or with palpation but mild discomfort with erection. He denied trauma, dysuria, hematuria, or discharge. He had no prior medical history and took no medications.
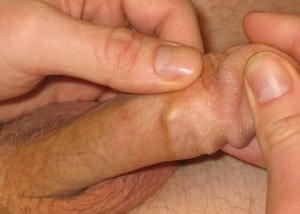
On physical exam, the patient had 2 palpable, firm cords wrapping around the dorsum of his penis just proximal to the glans (Figure). The affected area was non-tender and without swelling, erythema, or warmth. The skin was intact without lesions or signs of trauma. The rest of his exam was normal.
An ultrasound showed 2 short areas of noncompressibility consistent with superficial venous thrombosis. The urology consult recommended conservative treatment with non-steroidal anti-inflammatory drugs and warm compresses. When the patient was called 2 days after ED presentation, he reported that his symptoms had almost completely resolved.
Penile superficial venous thrombosis is an uncommon and little known benign genital condition; the largest case series in the literature describes 25 patients.1 The incidence is unknown and the condition may occur more frequently than reported given its benign symptomatology, frequent spontaneous resolution, and the possibly embarrassing nature of the complaint.
Penile Mondor’s disease affects sexually active men of any age. No specific cause has been determined, but detailed history frequently reveals prolonged or vigorous sexual intercourse causing stretching and torsion of penile veins. The disease has also been associated with other risk factors for localized and generalized clot formation.1, 2
Conservative treatment is effective in the vast majority of patients.1 For clots persisting longer than 6 weeks or persistent symptoms despite medical management, thrombectomy or superficial penile vein resection may be recommended.1, 2
Footnotes
Supervising Section Editor: Sean O. Henderson, MD
Submission history: Submitted August, 8 2012; Accepted August 13, 2012
Full text available through open access at http://escholarship.org/uc/uciem_westjem
DOI: 10.5811/westjem.2012.8.13276
Address for Correspondence: Jared Strote, MD, MS, Box 356123, Division of Emergency Medicine, University of Washington, 1959 NE Pacific Street, Seattle, WA 98195. Email: strote@uw.edu
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.