| Author | Affiliation |
|---|---|
| Aki Morishima, MD | Naval Hospital Okinawa |
| Joel M. Schofer, MD | Naval Hospital Okinawa |
| Pierre Pelletier, MD | Naval Hospital Okinawa |
| James M. McKee, MD | Naval Hospital Okinawa |
A 41-year-old African American female with a history of alcoholism in remission developed acute vomiting, chills, and severe left upper quadrant abdominal pain while climbing Mt. Fuji (Shizuoka Prefecture, Japan). She presented to a Japanese hospital and was diagnosed with cholelithiasis. The studies obtained are unknown and were unavailable.
She presented two days later to a military emergency department in Okinawa, Japan (a two hour flight from Mt. Fuji) with continued severe left upper quadrant pain, increased with inspiration. Her only medication was disulfiram. The remainder of her history was unremarkable. Her vitals signs were normal, except for a blood pressure of 158/93 mm Hg. She appeared to be in moderate distress. Her physical examination was significant for tenderness in the left upper quadrant with guarding but no rebound. She had left costovertebral angle tenderness. Her urinalysis showed small blood on the urine dipstick with negative microscopy. A non-contrast CT scan of the abdomen and pelvis, obtained to look for urolithiasis, showed cholelithiasis.
A contrast enhanced CT of the abdomen and pelvis was consistent with splenic infarction (Figure 1). Hemoglobin electrophoresis obtained upon admission was consistent with sickle cell trait. Splenic infarction in patients with sickle cell trait was first reported during the Korean War in African American pilots flying in unpressurizedaircraft.1
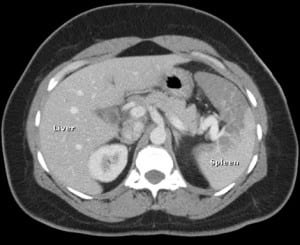
Contrast abdominal CT at the level of the splenic hilum shows lack of contrast enhancement in a large area of the anterior spleen.
Patients with sickle cell trait inherit a normal hemoglobin A gene from one parent and an abnormal hemoglobin S gene from the other parent. In the United States, it occurs in 7–10% of African Americans and is rare in people of other ethnicities.2 Although patients with sickle cell trait are usually asymptomatic, they can develop splenic infarctions in hypoxic environments.3
Signs and symptoms typically include epigastric and left upper quadrant pain developing over 48 hours and may include guarding, rebound, splenomegaly, fever, anorexia, and vomiting. Laboratory data often show increases in lactate dehydrogenase, leukocystosis, thrombocytopenia, and anemia.1,2,3, A CT scan with intravenous contrast will demonstrate areas of multifocal splenic infarcts. Splenic rupture is a rare complication. Treatment with supportive care including oxygen, analgesia, and hydration is usually adequate. Patients who are unstable may require splenectomy.2 In this case, supportive care was provided and the patient recovered without sequelae. Physicians should consider splenic infarction in patients who develop suspicious symptoms after exposure to a high altitude environment.3
Footnotes
Supervising Section Editor: Matthew Strehlow, MD
Submission history: Submitted April 7, 2008; Revision Received May 12, 2008; Accepted May 30, 2008
Full text available through open access at http://escholarship.org/uc/uciem_westjem
Address for Correspondence: Joel M. Schofer, MD, PSC, 482 Box 2827 FPO, AP 96362
Email: jschofer@gmail.com
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Chamberland DL. Splenic infarction in an African-American male with sickle cell trait.Am J Hemat. 2006;82:86–87. [PubMed]
2. Tiernan CJ. Splenic crisis at high altitude in 2 white men with sickle cell trait. Ann Emerg Med. 1999;33:230–233. [PubMed]
3. Sheikha A. Splenic syndrome in patients at high altitude with unrecognized sickle cell trait: splenectomy is often unnecessary. Can J Surg. 2005;48:377–381.[PMC free article] [PubMed]


