| Author | Affiliation |
|---|---|
| Lisa D. Mills, MD | University of California, Davis, Department of Emergency Medicine, Davis, CA |
| Karen May, MD | Louisiana State University at New Orleans, Section of Emergency Medicine, New Orleans, CA |
| Frank Mihlon, MD | University of Colorado Denver, Department of Radiology, Denver, CO |
ABSTRACT
The use of ultrasound by emergency physicians has improved the evaluation of pharyngeal infections. We present a unique case of concomitant peritonsillar abscess and uvular hydrops in which ultrasound provided accurate, timely information in the evaluation.
INTRODUCTION
We present a case of uvular hydrops with a peritonsillar abscess (PTA) concerning for airway compromise. Uvular hydrops is an uncommon and usually self-limited idiopathic process. Rarely, it can cause acute airway obstruction. The most common etiologies of uvular edema are allergic reaction or hereditary angioedema.1,2 There are reports of uvular hydrops with an infectious etiology.3–8
PTA is a focal, purulent infection in the posterior oropharynx. These abscesses generally respond quickly to incision and drainage (I and D) or needle aspiration and antibiotics without complication. However, the mass effect of the abscess and concomitant edema can obstruct the airway.
To our knowledge, there is no published report of uvular hydrops coincident with PTA. As a result, there is no knowledge of the airway implications of the dual condition.
CASE REPORT
A 40-year-old African-American male presented to the emergency department (ED) with sore throat for one week. The patient took ampicillin from a previous prescription for two days at an unknown dosage and interval and noted improvement in his sore throat. Several days following the antibiotic, the throat pain recurred and increased in severity over three days. The patient described the pain as “like a ball is stuck in my throat,” with subjective shortness of breath and fever for two days. The patient also reported pain but no difficulty swallowing.
The patient denied any past medical or surgical history, including history of allergic reactions and angioedema. He smoked 1–2 packs of cigarettes per day for approximately 20 years and used crack cocaine, remote from the ED presentation. The patient denied prescription medications other than the ampicillin.
On physical exam, the patient was afebrile with normal vital signs and oxygen saturation. He was in no apparent distress and conversed without difficulty. The patient was noted to have a “hot potato” voice and was spitting frequently, but had no trismus or stridor.
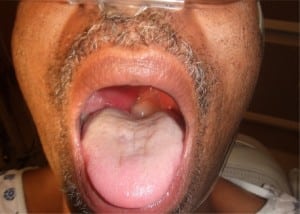
The head and neck exam showed bilateral erythematous tonsils with the right tonsil enlarged to 2.0 cm. The uvula was pale and edematous, measuring approximately 1×1 cm and deviated leftward (Figure 1). The exam revealed dental caries and eroded teeth. The patient had tender and enlarged right anterior cervical lymph nodes. The rest of the physical exam was normal.
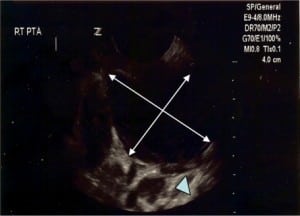
A lateral soft tissue radiograph of the neck showed no epiglottis involvement. The right tonsillar mass was evaluated with transoral ultrasound using the endocavitary probe on the Zonare Z.one (Zonare, Mountain View, CA), which confirmed a PTA (Figure 2). Computed tomography of the soft tissues of the neck revealed a right PTA with significant right-sided parapharyngeal edema and hydropic uvula, but no extension of the abscess or infectious process into the uvula. A basic metabolic panel and complete blood cell count with differential were normal except for a white blood cell count of 17,000/mm3.
The patient received clindamycin and methylprednisolone to treat the infection and edema of the PTA. No intervention was performed for the uvular hydrops. There was no change in the patient’s condition in the ED. In light of the negative history of allergic reaction and angioedema, no antihistamines were administered.
The otolaryngologist drained the PTA at the bedside without incident, and the patient was admitted to the intensive care unit to monitor his respiratory status. The patient was continued on clindamycin and steroids in the hospital. Symptoms completely resolved on day three and he was discharged.
DISCUSSION
To our knowledge, this is the only published report of uvular hydrops in association with a PTA. There is scant literature regarding uvular hydrops, prognosis and treatment and almost none regarding uvular hydrops in association with an infectious mass effect in the posterior oropharynx.7,8
Uvular hydrops associated with an infectious etiology is represented in anectodotal reports in the literature.3–8 Pain, odynophagia, fever, and an elevated white blood cell count points to infection. Known offending organisms include Group A beta hemolytic streptococcus, Hemophilus influenzae, and Streptococcus pneumoniae. These organisms are also commonly implicated in cases of pharyngitis, tonsillitis, and epiglottitis.2
Neither uvular hydrops nor PTA commonly obstruct the airway. Both conditions are usually managed as outpatients. However, both have been independently implicated in airway compromise. When present concurrently, there is no data on which to base prognosis. For this reason, the patient was admitted for observation of airway status. This patient had no complications or airway compromise. More experience is required to establish the occurrence of airway compromise with coexistent hydrops and PTA.
The development of a PTA is one of the most common complications of oropharyngeal infections and can also be a cause of significant airway compromise. It is most common in patients 20–40 years of age.9 Patients often present with dysphagia, drooling, trismus, and referred otalgia. The classic clinical finding is inferior medial displacement of the tonsil by the abscess with contralateral deviation of the uvula. These abscesses are generally unilateral and located at the superior aspect of the tonsil.10,11
The diagnosis of a PTA can be clinical, but radiographic studies such as CT scan or ultrasound may be helpful in confirming the diagnosis or ruling out other disease processes.9 In one study,12 it was found that clinical diagnosis alone has a sensitivity and specificity as low as 78% and 50%, respectively. With the use of CT scan the sensitivity approaches 100%. Intraoral ultrasound has sensitivity between 90 and 100%, is a quick alternative to CT scan, and it is generally well tolerated by patients.13–16 In patients with severe trismus who cannot tolerate the intraoral route, cervical transcutaneous ultrasound can be helpful. While it has a lower sensitivity (80%), it has specificity around 90%.14 The use of these two adjuncts together can greatly decrease missed or delayed diagnoses.
Treatment of PTA primarily consists of incision and drainage (I&D) or needle aspiration, antibiotics, and steroids.10,11 Most resolve without further incident with timely treatment. Intraoral ultrasound can be especially helpful to emergency physicians to facilitate needle aspiration. This can decrease the need for immediate sub-specialist consultation. CT scan before I&D can identify surrounding anatomy and decrease the risk of complications such as carotid artery perforation.9
Uvular hydrops is often idiopathic and self-limited. It can be a result of an acute allergic reaction or angioedema. The diagnosis is clinical, based on an edematous uvula. Neither imaging nor laboratory results contribute to ED diagnosis. Uvular hydrops may be accompanied by a sore throat or difficulty swallowing.1 The uvula will appear swollen and pale. This can be associated with significant hypopharyngeal edema. In this setting it is more likely to be associated with airway compromise. In the setting of hypopharyngeal edema, treatment for anaphylaxis is indicated. More commonly, the only indicated treatment for uvular hydrops is reassurance.
CONCLUSION
Bedside sonography augments clinical decision-making and enhances procedural accuracy. The application of ultrasonography to this patient with complicated oropharyngeal disease facilitated the timely diagnosis and appropriate management.
Footnotes
Supervising Section Editor: J Christian Fox MD, RDMS
Submission history: Submitted May 11, 2009; Revision Received November 29, 2009; Accepted November 29, 2009
Full text available through open access at http://escholarship.org/uc/uciem_westjem
Address for Correspondence: Lisa D Mills, MD, Section of Emergency Medicine, Louisiana State University, New Orleans, University Hospital, 2020 Gravier 7th Floor New Orleans, La 70112
Email: LMORR1@lsuhsc.edu
Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources, and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. McNamara RM. Clinical characteristics of acute uvulitis. Am J Emerg Med. 1994;12(1):51–2.[PubMed]
2. Goldberg R, Lawton R, Newton E, et al. Evaluation and management of acute uvular edema. Ann Emerg Med. 1993;22(2):251–5. [PubMed]
3. Murray A, Gardiner DS, McGuiness RJ. Primary mycobacterial infection of the uvula. J Laryngol Otol. 1998;112:1183–5. [PubMed]
4. Li KI, Kiernan S, Wald ER, et al. Isolated uvulitis due to Haemophilus influenzae type b. Pediatrics.1984;74:1054. [PubMed]
5. Aquino V, Terndrup TE. Uvulitis in three children: etiology and respiratory distress. Pediatr Emerg Care. 1992;8:206. [PubMed]
6. Brook I. Uvulitis caused by anaerobic bacteria. Pediatr Emerg Care. 1997;13:221. [PubMed]
7. McNamara R, Koobatian T. Simultaneous uvulitis and epiglottitis in adults. Am J Emerg Med.1997;15:161. [PubMed]
8. Jerrard DA, Olshaker J. Simultaneous uvulitis and epiglottitis without fever or leukocytosis. Am J Emerg Med. 1996;14:551. [PubMed]
9. Khayr W, Taepke J. Management of peritonsillar abscess: needle aspiration versus incision and drainage versus tonsillectomy. Am J Ther. 2005;12(4):344–50. [PubMed]
10. Melio F. Marx: Rosen’s Emergency Medicine: Concepts and Clinical Practice. 6th ed. Los Angeles, CA: Mosby; 2006. Upper Respiratory Tract Infections.
11. Lamkin RH, Portt J. An outpatient medical treatment protocol of peritonsillar abscess. Ear Nose Throat J. 2006;85(10):658, 660. [PubMed]
12. Scott Pm, Loftus UK, Kew J, et al. Diagnosis of peritonsillar infections: a prospective study of ultrasound, computed tomography, and clinical diagnosis. J Laryngol Otol. 1999;113(3):229–32.[PubMed]
13. Buckley AR, Moss EH, Blokmanis A. Diagnosis of peritonsillar abscess: value of intraoral sonography. American Journal of Roentgenology. 1994;162:961–4. [PubMed]
14. Filho B, Sakae F, Sennes L, et al. Intraoral and transcutaneous ultrasound in the differential diagnoses of peritonsillar cellulitis and abscess. Revista Brasileirra de Otorrinolaringlogia.2006;72(3)
15. Lyon M, Blaivas M. Intraoral ultrasound in diagnosis and treatment of suspected peritonsillar abscess in the emergency department. Acad Emerg Med. 2005;12(1):85–8. [PubMed]
16. Blaivas M, Theodoro D, Duggal S. Ultrasound-guided drainage of peritonsillar abscess by the emergency physician. Am J Emerg Med. 2003;21(2):155–8. [PubMed]
17. Lyon M, Glisson P, Blaivas M. Bilateral Peritonsillar Abscess Diagnosed on the Basis of Intraoral Sonography. J. Ultrasound Med. 2003;22(9):993–6. [PubMed]


