| Author | Affiliation |
|---|---|
| James Liang, DO | Naval Medical Center San Diego, Department of Emergency Medicine, San Diego, California |
| Adam Field, MD | Naval Medical Center San Diego, Department of Emergency Medicine, San Diego, California |
| Kimberly Liang, PharmD | Naval Medical Center San Diego, Department of Pharmacy, San Diego, California |
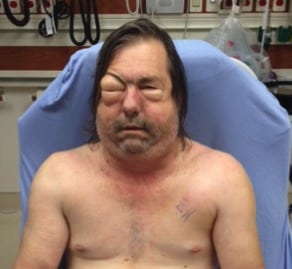
A 58-year-old man presented to the emergency department with diffuse swelling and crepitus of his face, chest, and extremities due to subcutaneous air (Figure). The patient had a history of lung cancer and had undergone a video-assisted transthoracic surgery (VATS) with decortications. His airway was maintained, and the patient reported only minimal shortness of breath with change in his phonation. Computed tomography of the chest showed a tumor at the left lung and an associated pneumothorax, along with extensive subcutaneous emphysema and pneumomediastinum throughout the thorax. An air source was found from the left chest due to a bronchopleural fistula (BPF).
A BPF is often a fatal complication of lung surgery postoperatively. It is defined as an abnormal communication between the bronchial tree and the pleural space.1–2 Air dissects along the bronchi and pulmonary vessels into the mediastinum, and may move into the subcutaneous space of the face and neck.3 The fistula is usually very small (about the size of a pinhole). The incidence is around 1–4% in patients undergoing lung surgery. The mortality rate ranges from 16–72%.4–6 Risk factors associated with the development of a BPF include diabetes, malignancy, and immunosuppressive therapy.7 A BPF that occurs in the early postoperative period is thought to be due to incomplete stapling or suturing of the bronchial stump. A BPF that occurs after 7 days postoperatively is usually secondary to ischemia or necrosis due to a tumor or extension of an empyema.2 Treatment includes suturing, omentopexy, and muscle plumbage. For small BPFs, minimally invasive techniques have also been used, such as a stent insertion, fibrin sealants, and one-way valve insertion.1
Subcutaneous emphysema usually resolves spontaneously, with minimal intervention. There are case reports of severe airway obstruction. If stridor develops, then upper airway obstruction is a possibility and endotracheal intubation should be done without delay.8 In a patient requiring intubation, consideration should be given to placement of a prophylactic chest tube, as the positive intrathoracic pressure can worsen the subcutaneous emphysema.9
Footnotes
Address for Correspondence: James Liang, DO. Department of Emergency Medicine, Naval Medical Center San Diego, 34800 Bob Wilson Drive, San Diego, CA 92134. Email: jmcl73@yahoo.com.
Submission history: Revision received November 1, 2012; Submitted December 31, 2012; Accepted January 28, 2013
Conflicts of Interest : By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none.
REFERENCES
1. Tanka S, Yajima T, Magi A, et al. Successful management of a large bronchopleural fistula after lobectomy: report of a case. Surgery Today. 2011;41:1661–1664. [PubMed]
2. Kilic A, Sciurba F, Luketich J, et al. Spontaneous bronchopleural fistula following lung volume reduction surgery for emphysema. Interactive Cardiovascular and Thoracic Surgery. 2009;8:442–443.[PubMed]
3. Battisella FD, Benfield JR. Blunt and penetrating injuries of the chest wall, pleura, and lungs. In: Shields TW, LoCicero J III, Ponn RB, editors. General Thoracic Surgery. 5th ed. Philadelphia: Lippincott Williams & Wilkins; 2000. p. 815.
4. Asamura H, Naruke T, Tsuchiya R, et al. Bronchopleural fistulas associated with lung cancer operations. Univariate and multivariate analysis of risk factors, management, and outcome. J Thoracic Cardiovascular Surgery. 1992;104:1456–1464. [PubMed]
5. Stephan F, Boucheseiche S, Hollande J, et al. Pulmonary complications following lung resection: a comprehensive analysis of incidence and possible risk factors. Chest. 2000;118:1263–1270. [PubMed]
6. Ponn RB. Complications of pulmonary resection. In: Shields TW, editor. General thoracic surgery.Philadelphia: Lippincott, Williams & Wilkins; 2005. pp. 554–586.
7. Galetta D, Veronesi G, Solli P, et al. A safe and effective method for an immediate bronchopleural fistula repair. Minerva Chirurgica. 2007;62:137–139. [PubMed]
8. Gibney RT, Finnegan B, FitzGerald MX, et al. Upper airway obstruction caused by massive subcutaneous emphysema. Intensive Care Med. 1984;10:43–44. [PubMed]
9. Zimmerman JE, Colgan DL, Mills M. Management of bronchopleural fistula complicating therapy with positive end expiratory pressure (PEEP) Chest. 1973;64:526–529. [PubMed]